Introduction
Hepatic encephalopathy (HE) is a disorder of the brain caused by hepatic insufficiency and/or portosystemic shunting. Manifestations of HE include a wide range of neurological or psychiatric abnormalities, affecting motor, cognitive, and mental neuropsychiatric function [1]. Patients with covert HE have neuropsychological and/or neurophysiological abnormalities but without disorientation or asterixis. By contrast, patients with overt HE have obvious clinical signs of HE, which may present with directional and computational impairment, asterixis, drowsiness, and even coma. According to the underlying liver disease, HE can be divided into three types, including type A (acute liver failure), type B (portosystemic shunting), and type C (cirrhosis) [1]. The severity of overt HE is classified into grade I, II, III, and IV according to the West-Haven criteria [2]. The incidence of HE in patients with liver cirrhosis is reportedly 30-45% [3–5]. The one-year survival rate of patients with HE is less than 50%, and the three-year survival rate is less than 25% [6]. HE contributes a significant burden on healthcare systems. In 2014, the estimated national economic burden of hospitalizations with HE reached $11.9 billion in the USA [7].
Potential pathogeneses of HE mainly include hyperammonemia [8, 9], increased synthesis of gamma-aminobutyric acid (GABA) and pseudo neurotransmitters [10, 11], as well as consequences of bacterial infection and inflammatory processes [12, 13]. As for the excess systemic ammonia hypothesis, the drugs for management of HE mainly include lactulose [14, 15], rifaximin [16], and probiotics [17], all of which reduce ammonia production and absorption, as well as L-ornithine-L-aspartate (LOLA) [18] which increases ammonia clearance. Among them, lactulose and rifaximin are approved as the first-line choice of treatment for HE by the American Food and Drug Administration as well as other national drug regulatory agencies [19]. As for the GABA and pseudo neurotransmitter hypothesis, the most widely studied drug for management of HE is flumazenil that can block the GABA neural pathway, thereby improving the inhibition of central nervous system [20]. As for the bacterial infection and inflammatory process hypothesis, the substances that can eliminate inflammatory mediators and suppress oxidative stress should be considered. Recently, it has been reported that albumin can improve systemic inflammatory responses [21], which, in theory, could potentially be an effective therapy for the management of HE. However, the role of albumin infusion in the management of HE remains controversial. Among the studies regarding preventive role of albumin infusion, Sola et al. found that albumin could not prevent from HE in liver cirrhosis [22], but several studies suggested that long-term infusion of albumin could decrease the risk of HE in decompensated cirrhosis [23, 24]. Among the studies investigating the therapeutic role of albumin infusion, Simon-Talero et al. reported a poor therapeutic effect of albumin infusion on HE (but with a significant improvement in 90 day survival) [25], but several studies suggested that albumin infusion could improve both HE and survival in patients with decompensated liver cirrhosis [26, 27]. Currently, the use of albumin infusion has not been recommended for management of HE by the AASLD-EASL practice guideline [1]. By comparison, the Italian Association for the Study of the Liver (AISF) suggested that albumin could decrease the incidence of grade III and IV type C overt HE in cirrhotic patients with ascites [28].
Our work included a retrospective observational study and a systematic review with meta-analysis to clarify the role of albumin infusion in prevention and treatment of overt HE in liver cirrhosis.
Results
Observational study
Patient selection
Between January 2010 and June 2014, a total of 2868 cirrhotic patients were included (Figure 1). In the prevention study, 2577 cirrhotic patients without overt HE at admission were included. There were 728 patients in the albumin infusion group and 1849 patients in the control group. In the treatment study, 468 cirrhotic patients with overt HE at or after admission were included. There were 213 patients in the albumin infusion group and 255 patients in the control group.
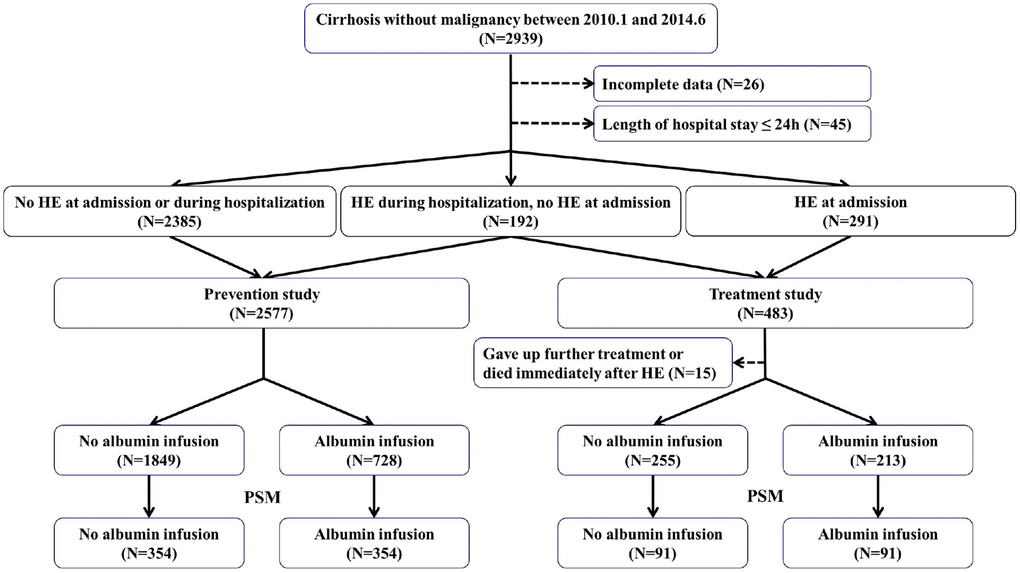
Figure 1. Flow chart of patient selection in our observational study.
Prevention study
After a 1:1 propensity score matching (PSM) analysis, a total of 708 patients were included. Three hundred and fifty-four patients were matched in each group (Figure 1). Baseline characteristics were described in Table 1. Median total dosage of albumin was 30g (range: 5–210g) in the albumin infusion group. Median Child-Pugh score was 8. Median MELD score was 7.30. The incidence of overt HE and the in-hospital mortality were 8.50% (60/708) and 3.50% (25/708), respectively (Table 2).
Table 1. Prevention study – Baseline characteristics in albumin and control groups after PSM.
| Variables | No. Pts | Overall | No. Pts | Albumin group | No. Pts | Control group | P value | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Age (years) | 708 | 56.80 (14.37-89.19) 57.82±12.54 | 354 | 57.63 (17.41-87.13) 58.12±12.57 | 354 | 56.45 (14.37-89.19) 57.52±12.52 | 0.454 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Sex (male) (%) | 708 | 440 (62.10%) | 354 | 226 (63.80%) | 354 | 214 (60.50%) | 0.352 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Etiology of Liver Diseases | 708 | 354 | 354 | 0.207 | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| HBV (%) | 192 (27.10%) | 102 (28.80%) | 90 (25.40%) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| HCV (%) | 43 (6.10%) | 22 (6.20%) | 21 (5.90%) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Alcohol Abuse (%) | 150 (21.20%) | 63 (17.80%) | 87 (24.60%) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| HBV+Alcohol Abuse (%) | 68 (9.60%) | 42 (11.90%) | 26 (7.30%) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| HCV+Alcohol Abuse (%) | 11 (1.60%) | 5 (1.40%) | 6 (1.70%) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Drug Related Liver Diseases (%) | 9 (1.30%) | 6 (1.70%) | 3 (0.80%) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Autoimmune Liver Diseases (%) | 46 (6.50%) | 22 (6.20%) | 24 (6.80%) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Other or Unknown Etiology (%) | 189 (26.70%) | 92 (26.00%) | 97 (27.40%) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Potential inducement of HE | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| AUGIB (%) | 708 | 196 (27.70%) | 354 | 88 (24.90%) | 354 | 108 (30.50%) | 0.093 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Infection (%) | 708 | 121 (17.10%) | 354 | 58 (16.40%) | 354 | 63 (17.80%) | 0.618 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Ascites (%) | 708 | 454 (64.10%) | 354 | 231 (65.30%) | 354 | 223 (63.00%) | 0.531 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Ascites (None/Mild/ Moderate+Severe) (%) | 708 | 254 (35.90%)/90 (12.70%)/364 (51.40%) | 354 | 123 (34.80%)/43 (12.10%)/188 (53.10%) | 354 | 131 (37.00%)/47 (13.30%)/176 (49.70%) | 0.662 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Abdominal Paracentesis (%) | 708 | 73 (10.30%) | 354 | 45 (12.70%) | 354 | 28 (7.90%) | 0.036 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Laboratory Tests | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| RBC (1012/L) | 706 | 2.98 (1.01-5.89) 3.00±0.78 | 353 | 3.05 (1.25-5.57) 3.05±0.73 | 353 | 2.87 (1.01-5.89) 2.94±0.83 | 0.024 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Hb (g/L) | 706 | 92.00 (27.00-176.00) 91.85±28.07 | 353 | 95.00 (29.00-169.00) 94.42±26.89 | 353 | 87.00 (27.00-176.00) 89.29±29.02 | 0.011 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| WBC (109/L) | 706 | 4.10 (0.80-33.00) 5.16±3.73 | 353 | 3.80 (0.80-26.00) 4.88±3.49 | 353 | 4.30 (1.00-33.00) 5.44±3.95 | 0.030 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| PLT (109/L) | 706 | 74.00 (3.00-467.00) 93.24±68.27 | 353 | 73.00 (17.00-394.00) 87.61±57.35 | 353 | 76.00 (3.00-467.00) 98.86±77.35 | 0.183 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| TBIL (μmol/L) | 708 | 23.30 (1.90-809.80) 44.20±70.97 | 354 | 24.30 (2.00-379.50) 38.44±47.17 | 354 | 22.40 (1.90-809.80) 49.96±88.30 | 0.737 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| DBIL (μmol/L) | 706 | 10.40 (0.30-562.80) 24.37±49.21 | 354 | 10.80 (0.30-276.20) 20.51±33.10 | 352 | 10.00 (0.40-562.80) 28.24±61.08 | 0.772 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| IBIL (μmol/L) | 706 | 13.05 (0.90-265.30) 19.91±25.55 | 354 | 13.35 (0.90-124.70) 17.93±16.99 | 352 | 12.45 (1.30-265.30) 21.90±31.85 | 0.801 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| ALB (g/L) | 708 | 30.15 (0.40-50.00) 30.20±6.28 | 354 | 29.70 (13.10-50.00) 30.06±6.42 | 354 | 30.60 (0.40-45.50) 30.34±6.14 | 0.191 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| ALT (U/L) | 708 | 25.00 (4.00-1460.00) 41.57±84.90 | 354 | 26.00 (4.00-495.00) 37.45±44.36 | 354 | 25.00 (5.00-1460.00) 45.69±111.51 | 0.985 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| AST (U/L) | 708 | 37.00 (7.00-1366.00) 58.32±80.67 | 354 | 37.00 (7.00-649.00) 56.51±58.18 | 354 | 36.00 (8.00-1366.00) 60.11±98.20 | 0.202 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| AKP (U/L) | 708 | 86.00 (17.00-969.00) 124.03±114.25 | 354 | 84.75 (26.00-739.70) 122.86±113.31 | 354 | 89.00 (17.00-969.00) 125.20±115.33 | 0.531 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| GGT(U/L) | 708 | 51.00 (6.00-2280.00) 119.25±193.61 | 354 | 48.00 (6.00-1221.00) 109.05±174.79 | 354 | 58.00 (8.00-2280.00) 129.45±210.51 | 0.117 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| BUN (mmol/L) | 708 | 6.08 (1.72-62.45) 7.80±6.45 | 354 | 6.18 (1.72-44.34) 7.69±5.81 | 354 | 6.00 (1.81-62.45) 7.91±7.03 | 0.307 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Scr (μmol/L) | 708 | 61.00 (23.00-933.90) 89.25±112.89 | 354 | 61.00 (27.40-702.00) 83.34±86.44 | 354 | 60.95 (23.00-933.90) 95.15±134.10 | 0.430 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| K (mmol/L) | 701 | 3.99 (2.13-8.28) 4.00±0.58 | 353 | 4.00 (2.68-8.28) 4.01±0.54 | 348 | 3.99 (2.13-7.24) 3.99±0.62 | 0.655 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Na (mmol/L) | 701 | 138.70 (118.90-157.80) 138.07±4.45 | 353 | 138.40 (124.60-157.80) 138.14±4.33 | 348 | 138.95 (118.90-152.40) 138.01±4.56 | 0.737 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Ammonia (μmol/L) | 343 | 36.00 (9.00-791.60) 47.27±58.18 | 164 | 35.00 (9.00-791.60) 45.79±71.75 | 179 | 36.00 (9.00-238.00) 48.62±42.26 | 0.228 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| PT (seconds) | 708 | 15.80 (10.50-42.50) 16.45±3.49 | 354 | 15.80 (11.00-33.70) 16.30±3.05 | 354 | 15.80 (10.50-42.50) 16.59±3.89 | 0.850 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| INR | 708 | 1.27 (0.76-4.75) 1.35±0.39 | 354 | 1.27 (0.79-3.28) 1.33±0.34 | 354 | 1.26 (0.76-4.75) 1.37±0.44 | 0.769 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| APTT (seconds) | 708 | 42.60 (27.30-472.40) 44.73±19.51 | 354 | 43.45 (28.80-83.30) 43.98±7.34 | 354 | 41.90 (27.30-472.40) 45.49±26.60 | 0.050 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Child-Pugh Score | 708 | 8 (5-13) 7.96±1.71 | 354 | 8 (5-13) 7.97±1.69 | 354 | 8 (5-13) 7.96±1.74 | 0.677 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Child-Pugh Class A/B/C (%) | 708 | 143 (20.20%)/444 (62.70%)/121 (17.10%) | 354 | 73 (20.60%)/224 (63.30%)/57 (16.10%) | 354 | 70 (19.80%)/220 (62.10%)/64 (18.10%) | 0.777 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| MELD Score | 708 | 7.30 (-5.64-38.80) 8.31±6.76 | 354 | 7.19 (-5.64-26.71) 8.10±6.03 | 354 | 7.33 (-5.08-38.80) 8.51±7.41 | 0.986 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Abbreviations: Pts: Patients; HBV: Hepatic B Virus; HCV: Hepatic C Virus; AUGIB: Acute Upper Gastrointestinal Bleeding, RBC: Red Blood Cell; Hb: Hemoglobin; WBC: White Blood Cell; PLT: Platelet Count; TBIL: Total Bilirubin; DBIL: Direct Bilirubin; IBIL: Indirect Bilirubin; ALB: Albumin; ALT: Alanine Aminotransferase; AST: Aspartate Aminotransferase; AKP: Alkaline Phosphatase; GGT: Gamma-Glutamyl Transpeptidase; BUN: Blood Urea Nitrogen; Scr: Serum Creatinine; K: Potassium; Na: Sodium; PT, Prothrombin Time; INR: International Standardization Ratio; APTT: Activated Partial Thromboplastin Time; MELD: Model for End-stage Liver Disease. | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Table 2. Prevention study - Interventions and outcomes of patients during hospitalizations in albumin and control groups after PSM.
| Variables | No. Pts | Overall | No. Pts | Albumin group | No. Pts | Control group | P value | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Frozen Plasma Infusion (%) | 708 | 136 (19.20%) | 354 | 61 (17.20%) | 354 | 75 (21.20%) | 0.182 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Lactulose (%) | 708 | 128 (18.10%) | 354 | 61 (17.20%) | 354 | 67 (18.90%) | 0.558 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| L-ornithine-L-aspartate (%) | 708 | 104 (14.70%) | 354 | 48 (13.60%) | 354 | 56 (15.80%) | 0.396 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Compound Amino Acid (6AA) (%) | 708 | 95 (13.40%) | 354 | 44 (12.40%) | 354 | 51 (14.40%) | 0.440 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Compound Amino Acid (15HBC) (%) | 708 | 268 (37.90%) | 354 | 126 (35.60%) | 354 | 142 (40.10%) | 0.215 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Compound Amino Acid (18AA) (%) | 708 | 98 (13.80%) | 354 | 42 (11.90%) | 354 | 56 (15.80%) | 0.128 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Arginine (%) | 708 | 73 (10.30%) | 354 | 32 (9.00%) | 354 | 41 (11.60%) | 0.266 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Alanylglutamine (%) | 708 | 121 (17.10%) | 354 | 55 (15.50%) | 354 | 66 (18.60%) | 0.272 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Antibiotic (%) | 708 | 376 (53.10%) | 354 | 175 (49.40%) | 354 | 201 (56.80%) | 0.050 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Dosage of Albumin Infused (g) | 354 | 30 (5-210) 42.75±35.47 | NA | 30 (5-210) 42.75±35.47 | 354 | NA | NA | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Incidence of Overt HE (%) | 708 | 60 (8.50%) | 354 | 15 (4.20%) | 354 | 45 (12.70%) | <0.001 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Time from Admission to HE (days) | 60 | 4.21 (0.24-84.79) 8.54±13.09 | 15 | 5.61 (1.62-47.99) 10.52±11.73 | 45 | 3.73 (0.24-84.79) 7.89±13.57 | 0.066 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| In-hospital Death (%) | 708 | 25 (3.50%) | 354 | 6 (1.70%) | 354 | 19 (5.40%) | 0.008 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Abbreviations: NA: Not Applicable; HE: Hepatic Encephalopathy. | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
The albumin infusion group had significantly higher red blood cell (P=0.024) and hemoglobin (P=0.011) and lower white blood cell (P=0.030) than the control group (Table 1). The albumin infusion group had a significantly higher proportion of abdominal paracentesis than the control group (12.70% versus 7.90%, P=0.036) (Table 2). The albumin infusion group had significantly lower incidence of overt HE (4.20% versus 12.70%, P<0.001) and in-hospital mortality (1.70% versus 5.40%, P=0.008) than the control group (Table 2).
Treatment study
After a 1:1 PSM analysis, a total of 182 patients were included. Ninety-one patients were matched in each group (Figure 1). Baseline characteristics were described in Table 3. Median total dosage of albumin was 40g (range: 10–250g) in the albumin infusion group. Median Child-Pugh score was 10. Median model for end-stage liver disease (MELD) score was 12.21. The rate of HE improvement and the in-hospital mortality were 76.40% (139/182) and 13.70% (25/182), respectively (Table 4).
Table 3. Treatment study - Baseline characteristics in albumin and control groups after PSM.
| Variables | No. Pts | Overall | No. Pts | Albumin group | No. Pts | Control group | P value | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Age (years) | 182 | 57.04 (30.78-84.77) 58.93±11.81 | 91 | 56.01 (38.06-84.74) 58.99±11.83 | 91 | 58.17 (30.78-84.77) 58.86±11.85 | 0.927 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Sex (male) (%) | 182 | 123 (67.60%) | 91 | 59 (64.80%) | 91 | 64 (70.30%) | 0.428 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Etiology of Liver Diseases | 182 | 91 | 91 | 0.069 | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| HBV (%) | 44 (24.20%) | 28 (30.80%) | 16 (17.60%) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| HCV (%) | 10 (5.50%) | 5 (5.50%) | 5 (5.50%) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Alcohol Abuse (%) | 49 (26.90%) | 18 (19.80%) | 31 (34.10%) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| HBV+Alcohol Abuse (%) | 22 (12.10%) | 12 (13.20%) | 10 (11.00%) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| HCV+Alcohol Abuse (%) | 2 (1.10%) | 1 (1.10%) | 1 (1.10%) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Drug Related Liver Diseases (%) | 2 (1.10%) | 0 (0.00%) | 2 (2.20%) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Autoimmune Liver Diseases (%) | 15 (8.20%) | 11 (12.10%) | 4 (4.40%) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Other or Unknown Etiology (%) | 38 (20.90%) | 16 (17.60%) | 22 (24.20%) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Potential inducement of HE | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| AUGIB (%) | 182 | 58 (31.90%) | 91 | 29 (31.90%) | 91 | 29 (31.90%) | 1.000 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Infection (%) | 182 | 47 (25.80%) | 91 | 21 (23.10%) | 91 | 26 (28.60%) | 0.397 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Ascites (%) | 182 | 136 (74.70%) | 91 | 67 (73.60%) | 91 | 69 (75.80%) | 0.733 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Ascites (None/Mild/ Moderate+Severe) (%) | 182 | 46 (25.30%)/22 (12.10%)/114 (62.60%) | 91 | 24 (26.40%)/10 (11.00%)/57 (62.60%) | 91 | 22 (24.20%)/12 (13.20%)/57 (62.60%) | 0.874 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Abdominal Paracentesis (%) | 182 | 28 (15.40%) | 91 | 15 (16.50%) | 91 | 13 (14.30%) | 0.681 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Overt HE | 182 | 91 | 91 | 1.000 | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Grade 1-2 (%) | 124 (68.10%) | 62 (68.10%) | 62 (68.10%) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Grade 3-4 (%) | 58 (31.90%) | 29 (31.90%) | 29 (31.90%) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Laboratory Tests | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| RBC (1012/L) | 181 | 2.69 (1.19-5.33) 2.76±0.72 | 90 | 2.61 (1.19-4.54) 2.70±0.72 | 91 | 2.80 (1.52-5.33) 2.82±0.73 | 0.241 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Hb (g/L) | 181 | 89.00 (42.00-157.00) 89.84±24.91 | 90 | 89.50 (42.00-144.00) 87.72±22.93 | 91 | 87.00 (43.00-157.00) 91.93±26.69 | 0.367 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| WBC (109/L) | 181 | 4.60 (1.10-31.40) 5.90±4.23 | 90 | 4.40 (1.10-31.40) 5.64±4.75 | 91 | 5.00 (1.30-21.00) 6.16±3.67 | 0.081 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| PLT (109/L) | 181 | 76.00 (13.00-314.00) 82.55±49.55 | 90 | 68.50 (13.00-282.00) 77.98±51.20 | 91 | 80.00 (17.00-314.00) 87.08±47.71 | 0.077 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| TBIL (μmol/L) | 182 | 38.95 (5.90-607.80) 62.40±76.80 | 91 | 37.10 (5.90-607.80) 61.37±85.35 | 91 | 39.30 (7.70-383.20) 63.43±67.64 | 0.437 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| DBIL (μmol/L) | 182 | 17.70 (0.70-331.70) 33.86±48.78 | 91 | 16.80 (0.70-331.70) 32.02±52.69 | 91 | 18.80 (3.60-242.50) 35.71±44.75 | 0.297 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| IBIL (μmol/L) | 182 | 19.10 (1.90-276.10) 28.54±31.10 | 91 | 18.50 (1.90-276.10) 29.36±35.71 | 91 | 19.70 (3.30-140.70) 27.72±25.84 | 0.842 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| ALB (g/L) | 182 | 27.10 (0.40-42.50) 26.79±6.05 | 91 | 26.50 (10.50-42.50) 26.55±6.13 | 91 | 27.30 (0.40-42.40) 27.03±5.99 | 0.465 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| ALT (U/L) | 182 | 26.00 (8.00-748.00) 41.63±70.97 | 91 | 25.00 (8.00-201.00) 35.88±33.10 | 91 | 27.00 (9.00-748.00) 47.38±74.70 | 0.467 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| AST (U/L) | 182 | 43.50 (11.00-1230.00) 66.79±108.64 | 91 | 42.00 (14.00-228.00) 54.42±40.39 | 91 | 44.00 (11.00-1230.00) 79.15±147.63 | 0.563 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| AKP (U/L) | 182 | 91.00 (17.00-470.00) 111.22±68.39 | 91 | 88.00 (25.00-402.00) 108.22±66.64 | 91 | 98.00 (17.00-470.00) 114.23±70.34 | 0.462 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| GGT (U/L) | 182 | 43.00 (8.00-1102.00) 84.43±124.90 | 91 | 41.00 (9.00-702.00) 79.67±107.84 | 91 | 46.00 (8.00-1102.00) 89.19±140.36 | 0.402 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| BUN (mmol/L) | 182 | 7.93 (1.58-62.45) 10.83±9.35 | 91 | 7.94 (1.72-46.02) 10.15±8.04 | 91 | 7.79 (1.58-62.45) 11.50±10.50 | 0.847 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Scr (μmol/L) | 182 | 69.50 (24.00-1069.00) 103.57±119.91 | 91 | 71.00 (25.00-533.60) 93.35±77.32 | 91 | 68.00 (24.00-1069.00) 113.79±150.75 | 0.830 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| K (mmol/L) | 182 | 4.10 (2.25-5.99) 4.15±0.67 | 91 | 4.10 (2.65-5.57) 4.17±0.59 | 91 | 4.10 (2.25-5.99) 4.12±0.75 | 0.694 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Na (mmol/L) | 182 | 137.70 (83.00-152.40) 136.42±6.63 | 91 | 138.00 (83.00-146.60) 136.60±7.47 | 91 | 137.10 (121.00-152.40) 136.23±5.71 | 0.287 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Ammonia (μmol/L) | 177 | 73.00 (5.30-415.00) 81.47±57.54 | 88 | 75.50 (5.30-325.00) 80.87±58.85 | 89 | 72.00 (9.00-415.00) 82.07±56.54 | 0.818 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| PT (seconds) | 182 | 18.20 (11.50-62.80) 19.50±6.11 | 91 | 18.30 (11.50-62.80) 19.87±7.36 | 91 | 18.00 (12.30-36.30) 19.14±4.55 | 0.821 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| INR | 182 | 1.55 (0.88-7.96) 1.70±0.80 | 91 | 1.55 (0.88-7.96) 1.75±0.97 | 91 | 1.52 (0.94-3.60) 1.66±0.52 | 0.954 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| APTT (seconds) | 182 | 45.95 (29.30-180.00) 48.98±14.89 | 91 | 47.00 (29.30-180.00) 49.75±17.18 | 91 | 44.80 (30.00-114.90) 48.22±12.22 | 0.495 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Child-Pugh Score | 182 | 10 (5-14) 9.95±2.01 | 91 | 10 (5-14) 9.92±1.90 | 91 | 10 (6-14) 9.98±2.13 | 0.895 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Child-Pugh Class A/B/C (%) | 182 | 4 (2.20%)/73 (40.10%)/105 (57.70%) | 91 | 2 (2.20%)/36 (39.60%)/53 (58.20%) | 91 | 2 (2.20%)/37 (40.70%)/52 (57.10%) | 0.988 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| MELD Score | 182 | 12.21 (0.13-42.68) 13.50±8.40 | 91 | 11.92 (0.79-42.68) 13.07±7.96 | 91 | 12.50 (0.13-38.80) 13.94±8.84 | 0.676 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Abbreviations: Pts: Patients; HBV: Hepatic B Virus; HCV: Hepatic C Virus; AUGIB: Acute Upper Gastrointestinal Bleeding; RBC: Red Blood Cell; Hb: Hemoglobin; WBC: White Blood Cell; PLT: Platelet Count; TBIL: Total Bilirubin; DBIL: Direct Bilirubin; IBIL: Indirect Bilirubin; ALB: Albumin; ALT: Alanine Aminotransferase; AST: Aspartate Aminotransferase; AKP: Alkaline Phosphatase; GGT: Gamma-Glutamyl Transpeptidase; BUN: Blood Urea Nitrogen; Scr: Serum Creatinine; K: Potassium; Na: Sodium; PT, Prothrombin Time; INR: International Standardization Ratio; APTT: Activated Partial Thromboplastin Time; MELD: Model for End-stage Liver Disease. | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Table 4. Treatment study- Interventions and outcomes of patients during hospitalizations in albumin and control groups after PSM.
| Variables | No. Pts | Overall | No. Pts | Albumin group | No. Pts | Control group | P value | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Frozen Plasma Infusion (%) | 182 | 54 (29.70%) | 91 | 29 (31.90%) | 91 | 25 (27.50%) | 0.516 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Lactulose (%) | 182 | 87 (47.80%) | 91 | 45 (45.50%) | 91 | 42 (46.20%) | 0.656 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| L-ornithine-L-aspartate (%) | 182 | 132 (72.50%) | 91 | 69 (75.80%) | 91 | 63 (69.20%) | 0.319 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Compound Amino Acid (6AA) (%) | 182 | 115 (63.20%) | 91 | 56 (61.50%) | 91 | 59 (64.80%) | 0.645 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Compound Amino Acid (15HBC) (%) | 182 | 41 (22.50%) | 91 | 19 (20.90%) | 91 | 22 (24.20%) | 0.595 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Compound Amino Acid (18AA) (%) | 182 | 14 (7.70%) | 91 | 6 (6.60%) | 91 | 8 (8.80%) | 0.578 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Arginine (%) | 182 | 105 (57.70%) | 91 | 51 (56.00%) | 91 | 54 (59.30%) | 0.653 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Alanylglutamine (%) | 182 | 20 (11.00%) | 91 | 12 (13.20%) | 91 | 8 (8.80%) | 0.343 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Antibiotics (%) | 182 | 101 (55.50%) | 91 | 48 (52.70%) | 91 | 53 (58.20%) | 0.456 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Dosage of Albumin Infused (g) | 91 | 40 (10-250) 46.48±37.16 | NA | 40 (10-250) 46.48±37.16 | 91 | NA | NA | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Improvement of Overt HE (%) | 182 | 139 (76.40%) | 91 | 77 (84.60%) | 91 | 62 (68.10%) | 0.009 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| In-hospital Death (%) | 182 | 25 (13.70%) | 91 | 7 (7.70%) | 91 | 18 (19.80%) | 0.018 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Abbreviations: NA: Not Applicable; HE: Hepatic Encephalopathy. | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
No significant difference in the baseline characteristics and interventions was observed between albumin infusion and control groups (P>0.05, in all comparisons) (Table 3 and Table 4). The albumin infusion group had a significantly higher rate of overt HE improvement (84.60% versus 68.10%, P=0.009) and a significantly lower in-hospital mortality (7.70% versus 19.80%, P=0.018) than the control group (Table 4).
Systematic review with meta-analysis
Study selection
A total of 3496 studies were identified in EMBASE, PubMed, and Cochrane Library databases. Finally, 9 studies were eligible, including 6 studies investigating the prevention of HE and 3 studies investigating the treatment of HE (Supplementary Figure 1). Characteristics of the studies were summarized in Table 5. Among all of these included studies, the severity of HE was assessed based on the West-Haven criteria [2]. Inclusion and exclusion criteria were summarized in Supplementary Table 1. Characteristics of patients were summarized in Supplementary Table 2. Biochemical variables for treatment studies were summarized in Supplementary Table 3.
Table 5. Characteristics of studies.
| First Author (year) | Country | Study Design | Enrollment Period | Number of Patients | Dosage of Albumin Infused | Outcomes | Main Findings | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Treatment study | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Jalan (2004) | UK | Cohort | NA | 15 | Albumin group: to administer 4.5% albumin intravenously until the central venous pressure was sustained at 7–10mmHg. Control group: none. | Improvement of HE during 3 days. | Severity of HE was significantly improved in the albumin group at both 24 and 72h (P<0.01), which was not observed in the control group (P=0.21). | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Simon-Talero (2013) | Spain | RCT | 2009- 2012 | 56 | Albumin group: day 1: albumin 1.5g/kg; day 3: albumin 1.0g/kg. Control group: none. | Presence of HE at day 4. | No difference in the proportion of patients without HE at day 4 between albumin and control groups (65.2% vs 57.1%, P=0.6). | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Sharma (2017) | India | RCT | 2015- 2016 | 120 | Albumin group: albumin 1.5g/kg/day. Control group: none. | Recovery of HE during 10 days. | Difference in the rate of complete reversal of HE within 10 days was significant between albumin and control groups (75% vs 53.3%, P=0.03). | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Prevention study | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Planas (1990) | Spain | RCT | NA | 88 | Albumin group: when 1L of ascites was removed, 8g albumin was infused. Control group: none. | Improvement of ascites. Incidence of HE. | Three patients developed HE during hospitalization in each group (albumin and control group). | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Riggio (2015) | Italy | Cohort | NA | 68 | Albumin group: day 1, 2: albumin 1.0g/kg/day; day 4, 7, 14, 21, 28: albumin 0.5g/kg/day. Control group: none. | Incidence of overt HE during first month. | No difference in the incidence of HE between albumin and control groups during the first month (34% vs 31%) or during the whole follow-up (39% vs 48%). | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Arora (2018) | India | RCT | NA | 59 | Albumin group: when 1L of ascites was removed, 8g albumin was infused. Control group: none. | Improvement of ascites. Incidence of HE. | No difference in the incidence of HE between albumin and control groups (6.7% vs 24%, P=0.06). | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Caraceni (2018) | Italy | RCT | 2011- 2015 | 431 | Albumin group: albumin 40g twice per week for two weeks, and then 40g albumin per week. Control group: no additional use of albumin, except for standard medical treatment. | Improvement of ascites. Incidence of HE. | Difference in the incidence of HE was significant between albumin and control groups (rate ratio=0.48, 95%CI=0.37 to 0.63, P<0.001). | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Sola (2018) | Spain | RCT | 2008- 2015 | 173 | Albumin group: albumin 40g per 15 days. Control group: none. | Incidence of complications of cirrhosis. Incidence of HE. | No difference in the incidence of HE between albumin and control groups (28% vs 24%, P=0.635). | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Di Pascoli (2019) | Italy | Cohort | 2012- 2016 | 70 | Albumin group: albumin 20g twice per week; when 1L of ascites was removed and 6-8g albumin was infused. Control group: no additional use of albumin, except for standard medical treatment. | 24-month mortality. Incidence of HE. | Difference in the incidence of HE was significant between albumin and control groups (26.9% vs 64.5%, P=0.016). | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Abbreviations: HE: Hepatic Encephalopathy; RCT: Randomized Controlled Trial; NA: Not Available. | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Prevention study
A total of 889 patients were included. The sample size ranged from 59 to 431 among studies. Four studies were randomized controlled trials (RCTs), and 2 studies were cohort studies. All studies were published between 1990 and 2019.
In terms of random sequence generation and blinding of participants and personnel, 3 RCTs had a low risk of bias; as for allocation concealment, 2 RCTs had a low risk of bias; as for blinding of outcome assessment, incomplete outcome data, and selective reporting, all RCTs had a low risk of bias; in terms of other bias, all RCTs had an unclear risk of bias (Supplementary Figure 2A). The Riggio’s [29] and Di Pascoli’s [24] study scored 8 and 7 points according to the Newcastle-Ottawa Scale, respectively.
The data regarding the development of overt HE was extracted in 6 studies including 889 patients [22–24, 29–31] (Supplementary Table 4). Albumin infusion might decrease the risk of overt HE in cirrhosis (OR=1.63, 95%CI=0.96 to 2.75, P=0.07), but the difference did not reach statistical significance (Figure 2A). There was a significant heterogeneity among studies (I2=47%, P=0.09). There was no significant publication bias (P=0.437) (Supplementary Figure 3).
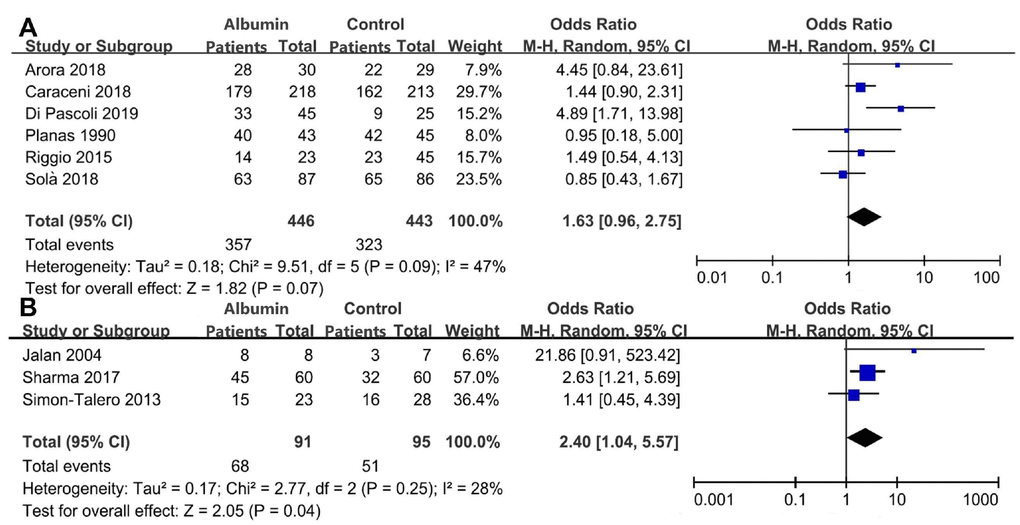
Figure 2. Meta-analyses regarding the prevention (A) and treatment (B) of overt HE.
Treatment study
A total of 191 patients were included. The sample size ranged from 15 to 120 among studies. Two studies were RCTs, and 1 study was a cohort study. All studies were published between 2004 and 2017.
In terms of random sequence generation, allocation concealment, and blinding of participants and personnel, 1 RCT had a low risk of bias; in terms of blinding of outcome assessment, incomplete outcome data, and selective reporting, all RCTs had a low risk of bias; as for other bias, all RCTs studies had an unclear risk of bias (Supplementary Figure 2B). The Jalan’s [27] study scored 5 points according to the Newcastle-Ottawa Scale.
The data regarding the improvement of overt HE was explored in 3 studies including 191 patients [25–27] (Supplementary Table 5). Albumin infusion might increase the improvement of overt HE (odds ratio [OR]=2.40, 95% confidence interval [CI]=1.04 to 5.57, P=0.04) (Figure 2B). There was no significant heterogeneity (I2=28%, P=0.25). There was no significant publication bias (P=0.623) (Supplementary Figure 4).
Plasma ammonia level was explored in 3 studies including 191 patients [25–27]. Albumin infusion did not significantly change the ammonia level (mean difference [MD]=0.28, 95%CI=-3.03 to 3.58, P=0.87) (Supplementary Figure 5A). There was no significant heterogeneity (I2=0%, P=0.86).
Interleukin (IL)-6 level was explored in 2 studies including 176 patients [25, 26]. Albumin infusion significantly decreased the IL-6 level (MD=-6.20, 95%CI=-8.66 to -3.75, P<0.00001) (Supplementary Figure 5B). There was no significant heterogeneity (I2=0%, P=0.77).
tumor necrosis factor (TNF)-α level was explored in 2 studies including 176 patients [25, 26]. Albumin infusion might decrease the TNF-α level (MD=-1.08, 95%CI=-22.94 to 20.77, P=0.92) (Supplementary Figure 5C), but the difference was not statistically significant. There was a significant heterogeneity (I2=64%, P=0.10).
Discussion
Based on a single-center retrospective study involving 2868 cirrhotic patients and a meta-analysis of 9 studies, the main findings were as follows. First, albumin infusion was associated with reduced incidence and improvement of overt HE. Based on the results of our meta-analysis, the number needed to treat was 14 (95%CI=8 to 46) and 5 (95%CI=4 to 6) for preventing the development of overt HE and improving the severity of overt HE, respectively. Second, albumin infusion might be associated with reduced in-hospital mortality in cirrhotic patients with or without overt HE.
Our study had several features. First, our findings were not only derived from a relatively large number of original data obtained at our hospital, but also further confirmed by meta-analyses. Second, a 1:1 PSM analysis was employed to adjust the factors that might influence the outcomes of overt HE, including severity of liver dysfunction, infection, paracentesis, gastrointestinal bleeding, and drugs for HE. Third, our original study focused on the in-hospital outcomes. Fourth, our study objectives included both prevention and treatment of overt HE.
Albumin, which not only expands intravascular volume and improves microcirculation but also binds numerous substances, such as bile acids, nitric oxide, and cytokines [32, 33], has been widely employed for management of cirrhosis and portal hypertension related complications in real-world clinical practice. An US-based AASLD survey on the use of albumin in cirrhosis suggested that albumin was mainly employed for preventing post-paracentesis circulatory dysfunction (PPCD) and hepatorenal syndrome (HRS) and treating spontaneous bacterial peritonitis (SBP), HRS, hypotension, refractory ascites, hyponatremia, edema, and hypoalbuminemia [34]. Notably, only a few physicians prescribed albumin for HE. A European survey on use of albumin in cirrhosis suggested that albumin was mainly employed for preventing PPCD and renal failure and treating type-1 HRS, ascites, non-SBP bacterial infections, severe hyponatremia (<125mmol/L), HE, and hypoalbuminemia [35]. Among them, only a few indications have been recommended by the evidence-based guidelines. For example, the AASLD guideline recommends that albumin should be employed for large-volume paracentesis and HRS [36]; similarly, the EASL guideline suggests that albumin should be employed for the prevention of PPCD, SBP, and HRS [37]. By comparison, other indications, such as HE, hyponatremia, hypoalbuminemia, edema, and non-SBP bacterial infections, were not sufficiently supported by the currently available evidence. In our study, human albumin was prescribed at the discretion of attending physicians, and the primary indications for the use of albumin infusion mainly included post-paracentesis, ascites, and hypoalbuminemia.
Inflammatory markers and serum endotoxin levels are significantly increased in decompensated cirrhotic patients [21, 38, 39]. These cytokines may affect the integrity of the blood-brain barrier, and allow a large number of plasma ammonia ions enter into the brain, thereby causing HE [39, 40]. Recently, it has been reported that anti-TNF-α treatment can improve cognitive impairment in rats caused by chronic hyperammonemia-induced peripheral and central nervous system inflammation that can lead to neurotransmission and cognitive impairment [41]. Albumin is a multi-domain protein stabilized by 17 disulfide bonds where 34 cysteine residues are involved [42]. Among them, a free cysteine (Cys-34) can regulate inflammation [43] by reversibly binding to many inflammation mediators and transporting them to specific tissues or organs [44]. Supplementation of albumin in patients with cirrhosis can bind to inflammatory cytokines and acts to protect the blood-brain barrier [21, 45]. Our meta-analysis also suggested that albumin infusion might decrease IL-6 level.
Oxidative stress may also have a potential role in the pathogenesis of HE [46–49]. Albumin has a powerful antioxidant capacity [50]. Such an effect can be achieved by the abilities of albumin in binding to and inactivating free metals, such as copper and iron, which can catalyze the formation of reactive oxygen [51, 52], and capturing free radicals, such as reactive oxygen and nitrogen [53–55], which can damage astrocytes in patients with HE [48, 49].
Serum sodium abnormalities may be a risk factor for HE in cirrhosis [56, 57]. In Caraceni’s study, albumin infusion significantly reduced the incidence of hyponatremia [23]. And, a recent large-scale study also found that albumin infusion could improve hyponatremia in patients with cirrhosis [58].
It has been proposed that the effect of albumin infusion for hyponatremia in cirrhosis may be attributed to the correction of an impaired Gibbs-Donnan equilibrium that results in the imbalance of charged particles near the semipermeable membrane can alter fluid dynamics [59]. At the Gibbs-Donnan equilibrium, the chemical gradient is equal in magnitude and opposite in direction to the electrical gradient as described by the following equation: FEm=-RT ln([Na+]1 ⁄[Na+]2), where F is Faraday’s constant; R is ideal gas constant; T is absolute temperature; [Na+]1 is the sodium concentration in the protein-containing compartment; and [Na+]2 is the sodium concentration in the non-protein-containing compartment [59].
Major limitations of our study are as follows. In our retrospective study, the potential for patient selection bias and misclassification were unavoidable; additionally, the standard dosage of albumin was lacking, but the dosage was often dependent upon the physicians’ considerations. In our meta-analysis, a relatively small number of studies were included, and the patient characteristics, duration and dosage of albumin, and use of other drugs for management of overt HE were heterogeneous among them. Additionally, we have to acknowledge that the absolute number of patients who developed HE events, but not the cumulative incidence of HE or number of HE events, was extracted from the original papers. This is because the data expression is often heterogeneous among studies. For example, in the ANSWER study, the data regarding the incidence of complications were reported by “per person/year”. It should also be considered that this study only reported the occurrence of grade III or IV HE and the duration of the follow-up of patients who only received standard medical treatment was significantly shorter with respect to those who also received albumin. This may have influenced the results of the present meta-analysis, as the incidence of HE episodes assessed by Kaplan-Meier estimation showed a significantly lower value in the group who received human albumin. Therefore, the role of albumin administration in the prevention of HE warrants investigation in future studies.
In conclusion, albumin infusion may be effective for preventing the development of overt HE and improving the severity of overt HE in patients with cirrhosis. In future studies, the hypothesis should be confirmed that the benefit of albumin in management of HE may be achieved by regulating inflammation and anti-oxidative stress and improving sodium concentration (Supplementary Figure 6). Considering a relatively high cost of human albumin, especially the need of a large dosage of albumin infused, the cost-effectiveness of albumin infusion in such patients should be further explored in the future. Additionally, albumin infusion may also decrease the in-hospital mortality of patients with cirrhosis regardless of overt HE. More prospective studies are needed to explore the role of albumin infusion for management of HE in cirrhotic patients.
Materials and Methods
Observational study
This observational study consisted of two parts: a prevention study that determined the role of albumin infusion in the prophylaxis of HE and a treatment study that determined the role of albumin infusion in the treatment of overt HE.
Ethics
This observational study was approved by the Medical Ethical Committee of the General Hospital of Northern Theater Command (formerly, the General Hospital of Shenyang Military Area). The ethical approval number is k (2018)18.
Patient selection
We reviewed the medical records of cirrhotic patients who were consecutively admitted to the General Hospital of Northern Theater Command from January 2010 to June 2014. Cirrhosis was diagnosed based on clinical grounds involving laboratory tests, endoscopic findings, ultrasonographic findings, and liver histology, if available. Other eligibility criteria were as follows: 1) age and gender were not limited; 2) patients had no malignancy; 3) electronic medical records were complete; and 4) length of hospital stay was more than 24 hours. This was primarily because the patients who had been hospitalized for less than 24 hours were unable to receive effective and sufficient therapy. In the prevention study, the exclusion criteria were as follows: 1) patients with a diagnosis of overt HE at admission; and 2) patients who underwent transjugular intrahepatic portosystemic shunt (TIPS) or surgical shunt. In the treatment study, the exclusion criteria were as follows: 1) patients without overt HE at or after admission; 2) patients’ relatives declined further treatment or patients died immediately after a diagnosis of overt HE; and 3) patients who underwent TIPS or surgical shunt.
Data collection
The primary data were collected as follows: age, gender, etiology of liver cirrhosis, ascites, acute upper gastrointestinal bleeding (AUGIB), infection, regular laboratory data, albumin infusion, albumin dosage, frozen plasma infusion, abdominal paracentesis, antibiotics, medications (i.e., lactulose, LOLA, compound amino acid, alanylglutamine, and arginine) for the prevention and treatment of overt HE, and in-hospital death. Child-Pugh [60] and MELD [61] scores were calculated. In the prevention study, we also recorded overt HE events during hospitalizations. In the treatment study, we also recorded the severity of overt HE at the time of diagnosis and the outcomes of overt HE after treatment during hospitalizations.
Groups
In the prevention study, the patients were classified into two groups: 1) the albumin group in which patients received albumin infusion during the entire hospitalization or before a diagnosis of overt HE; and 2) the control group in which patients did not receive any albumin infusion during the entire hospitalization or before a diagnosis of overt HE. In the treatment study, the patients were classified into two groups: 1) the albumin group in which patients received albumin infusion after a diagnosis of overt HE; and 2) the control group in which patients did not receive any albumin infusion after a diagnosis of overt HE.
Diagnosis and definitions
We reviewed the medical records to re-evaluate the diagnosis of overt HE according to the final report of 11th World Congresses of Gastroenterology [62]. The grade of HE was assessed based on the West-Haven criteria [2]. Improvement of HE was defined as the grade of HE was decreased to a lower grade according to the West-Haven criteria.
Outcomes
The outcomes of interest were the development and improvement of overt HE for the prevention and treatment studies, respectively. In-hospital mortality was also evaluated.
Statistical analysis
A 1:1 PSM analysis was performed. Matching factors included age, sex, severity of liver dysfunction (Child-Pugh and MELD scores), ascites, AUGIB, infection, serum albumin at baseline, frozen plasma infusion, abdominal paracentesis, antibiotics, and drugs (lactulose, LOLA, compound amino acid, alanylglutamine, and arginine) for the prevention and treatment of overt HE. Continuous variables were reported as mean ± standard deviation and median (range) and the differences between albumin and control groups were compared by the non-parametric Mann-Whitney U test. Categorical variables were reported as frequency (percentage) and the differences between albumin and control groups were compared by the chi-square test. A two-tailed P<0.05 was considered statistically significant. All statistical analyses were performed with IBM SPSS 20.0 (IBM Crop) statistical package and Stata/SE 12.0 (Stata Corp, College Station, TX) software.
Systematic review with meta-analysis
Registration
The registration number of PROSPERO was CRD42018085605.
Literature search
Three electronic databases (EMBASE, PubMed, and Cochrane Library) were searched from the earliest available publication until January 23, 2019. The following keywords were used: “albumin” and “hepatic encephalopathy”. No language restriction was applied. Only published data were considered. If some data was not available, we contacted with the corresponding authors to obtain the relevant data.
Study selection
All potentially eligible studies should compare the outcomes of cirrhotic patients treated with and without albumin. The exclusion criteria were as follows: 1) duplicate articles; 2) reviews or meta-analysis; 3) case reports; 4) experimental or animal studies; 5) comments or letters; 6) guidelines or consensus; and 7) irrelevant topics.
Data extraction
The following data were extracted: characteristics of included studies, baseline characteristics of patients, and outcome variables.
Groups
In the prevention study, the albumin group should be that patients received albumin infusion; the control group should be that patients received standard medical treatment without additional albumin infusion. In the treatment study, the albumin group should be that patients received albumin infusion after a diagnosis of HE; the control group should be that patients did not receive albumin infusion after a diagnosis of HE.
Outcomes
The primary outcomes were the development and improvement of overt HE for the prevention and treatment studies, respectively. The secondary outcomes were the changes of ammonia, IL-6, and TNF-α levels for the treatment studies.
Study quality assessment
For RCTs, the Cochrane Risk of Bias tool was applied to assess the risk of bias from random sequence generation (selection bias), allocation concealment (selection bias), blinding of participants and personnel (performance bias), blinding of outcome assessment (detection bias), incomplete outcome data (attrition bias), selective reporting (reporting bias), and other sources. For non-RCTs, the Newcastle-Ottawa quality assessment scale was applied to assess the study quality, which evaluated a total of 8 indicators with the highest score of 9 points.
Statistical analysis
The meta-analysis was performed using Review Manager (Version 5.2, Cochrane collaboration, The Nordic Cochrane Centre, Copenhagen) software and Stata/SE 12.0 (Stata Corp, College Station, TX) software. Dichotomous outcomes were expressed as OR with 95% CI; continuous outcomes were expressed as MD with 95% CI. Effect size estimates were analyzed using random-effect model. P<0.05 was considered statistically significant. Heterogeneity was assessed by the Cochrane Q test and the I2 statistics. P<0.1 or I2>50% was considered as a statistically significant heterogeneity. Publication bias was assessed by the Egger test. P<0.1 was considered as a statistically significant publication bias.
Author Contributions
Zhaohui Bai: reviewed and searched the literature, wrote the protocol, collected the data, performed the statistical analysis and quality assessment, interpreted the data, and drafted the manuscript; Mauro Bernardi, Eric M. Yoshida, Hongyu Li, Xiaozhong Guo, Nahum Méndez-Sánchez, Yingying Li, Ran Wang, and Jiao Deng: checked the data, discussed the findings, gave critical comments, and/or revised the manuscript; Xingshun Qi: conceived the work, reviewed and searched the literature, wrote the protocol, performed the statistical analysis, interpreted the data, and drafted and revised the manuscript; All authors have made an intellectual contribution to the manuscript and approved the submission.
Acknowledgments
We are indebted to our study team for establishing and updating our retrospective database, including Junna Dai, Cuihong Zhu, Yun Li, Ying Peng, Zheng Ning, Feifei Hou, Jiancheng Zhao, Han Deng, Ran Wang, Jing Li, Xintong Zhang, Dan Han, Tingxue Song, Zhong Peng, Wenchun Bao, and Yingying Li, of whom all had worked for our study group.
Conflicts of Interest
The authors declare that they have no competing interests.
References
- 1. American Association for the Study of Liver D, European Association for the Study of the L. Hepatic encephalopathy in chronic liver disease: 2014 practice guideline by the European Association for the Study of the Liver and the American Association for the Study of Liver Diseases. J Hepatol. 2014; 61:642–659. https://doi.org/10.1016/j.jhep.2014.05.042 [PubMed]
- 2. Blei AT, Cordoba J, Practice Parameters Committee of the American College of Gastroenterology. Hepatic Encephalopathy. Am J Gastroenterol. 2001; 96:1968–1976. [PubMed]
- 3. Romero-Gomez M, Boza F, Garcia-Valdecasas MS, Garcia E, Aguilar-Reina J. Subclinical hepatic encephalopathy predicts the development of overt hepatic encephalopathy. Am J Gastroenterol. 2001; 96:2718–2723. [PubMed]
- 4. Bismuth M, Funakoshi N, Cadranel JF, Blanc P. Hepatic encephalopathy: from pathophysiology to therapeutic management. Eur J Gastroenterol Hepatol. 2011; 23:8–22. https://doi.org/10.1097/MEG.0b013e3283417567 [PubMed]
- 5. Khungar V, Poordad F. Management of overt hepatic encephalopathy. Clin Liver Dis. 2012; 16:73–89. https://doi.org/10.1016/j.cld.2011.12.007 [PubMed]
- 6. Fichet J, Mercier E, Genee O, Garot D, Legras A, Dequin PF, Perrotin D. Prognosis and 1-year mortality of intensive care unit patients with severe hepatic encephalopathy. J Crit Care. 2009; 24:364–370. https://doi.org/10.1016/j.jcrc.2009.01.008 [PubMed]
- 7. Hirode G, Vittinghoff E, Wong RJ. Increasing Burden of Hepatic Encephalopathy Among Hospitalized Adults: An Analysis of the 2010-2014 National Inpatient Sample. Dig Dis Sci. 2019; 64:1448–1457. https://doi.org/10.1007/s10620-019-05576-9 [PubMed]
- 8. Brusilow SW, Koehler RC, Traystman RJ, Cooper AJ. Astrocyte glutamine synthetase: importance in hyperammonemic syndromes and potential target for therapy. Neurotherapeutics. 2010; 7:452–470. https://doi.org/10.1016/j.nurt.2010.05.015 [PubMed]
- 9. Gonzalez-Usano A, Cauli O, Agusti A, Felipo V. Hyperammonemia alters the modulation by different neurosteroids of the glutamate-nitric oxide-cyclic GMP pathway through NMDA- GABAA - or sigma receptors in cerebellum in vivo. J Neurochem. 2013; 125:133–143. https://doi.org/10.1111/jnc.12119 [PubMed]
- 10. Ahboucha S, Butterworth RF. The neurosteroid system: implication in the pathophysiology of hepatic encephalopathy. Neurochem Int. 2008; 52:575–587. https://doi.org/10.1016/j.neuint.2007.05.004 [PubMed]
- 11. Palomero-Gallagher N, Zilles K. Neurotransmitter receptor alterations in hepatic encephalopathy: a review. Arch Biochem Biophys. 2013; 536:109–121. https://doi.org/10.1016/j.abb.2013.02.010 [PubMed]
- 12. Seyan AS, Hughes RD, Shawcross DL. Changing face of hepatic encephalopathy: role of inflammation and oxidative stress. World J Gastroenterol. 2010; 16:3347–3357. [PubMed]
- 13. Shawcross D, Jalan R. The pathophysiologic basis of hepatic encephalopathy: central role for ammonia and inflammation. Cell Mol Life Sci. 2005; 62:2295–2304. https://doi.org/10.1007/s00018-005-5089-0 [PubMed]
- 14. de Lorenzo-Pinto A, Garcia-Sanchez R, Lorenzo-Salinas A. Lactulose enemas in the treatment of hepatic encephalopathy. Do we help or harm? Rev Esp Enferm Dig. 2017; 109:736–737. https://doi.org/10.17235/reed.2017.5106/2017 [PubMed]
- 15. Gluud LL, Vilstrup H, Morgan MY. Nonabsorbable disaccharides for hepatic encephalopathy: A systematic review and meta-analysis. Hepatology. 2016; 64:908–922. https://doi.org/10.1002/hep.28598 [PubMed]
- 16. Bass NM, Mullen KD, Sanyal A, Poordad F, Neff G, Leevy CB, Sigal S, Sheikh MY, Beavers K, Frederick T, et al. Rifaximin treatment in hepatic encephalopathy. N Engl J Med. 2010; 362:1071–1081. https://doi.org/10.1056/NEJMoa0907893 [PubMed]
- 17. Cao Q, Yu CB, Yang SG, Cao HC, Chen P, Deng M, Li LJ. Effect of probiotic treatment on cirrhotic patients with minimal hepatic encephalopathy: A meta-analysis. Hepatobiliary Pancreat Dis Int. 2018; 17:9–16. https://doi.org/10.1016/j.hbpd.2018.01.005 [PubMed]
- 18. Kircheis G, Nilius R, Held C, Berndt H, Buchner M, Gortelmeyer R, Hendricks R, Kruger B, Kuklinski B, Meister H, et al. Therapeutic efficacy of L-ornithine-L-aspartate infusions in patients with cirrhosis and hepatic encephalopathy: results of a placebo-controlled, double-blind study. Hepatology. 1997; 25:1351–1360. https://doi.org/10.1002/hep.510250609 [PubMed]
- 19. Prakash R, Mullen KD. Mechanisms, diagnosis and management of hepatic encephalopathy. Nat Rev Gastroenterol Hepatol. 2010; 7:515–525. https://doi.org/10.1038/nrgastro.2010.116 [PubMed]
- 20. Goh ET, Andersen ML, Morgan MY, Gluud LL. Flumazenil versus placebo or no intervention for people with cirrhosis and hepatic encephalopathy. Cochrane Database Syst Rev. 2017; 8:CD002798. https://doi.org/10.1002/14651858.CD002798.pub4 [PubMed]
- 21. Artigas A, Wernerman J, Arroyo V, Vincent JL, Levy M. Role of albumin in diseases associated with severe systemic inflammation: Pathophysiologic and clinical evidence in sepsis and in decompensated cirrhosis. J Crit Care. 2016; 33:62–70. https://doi.org/10.1016/j.jcrc.2015.12.019 [PubMed]
- 22. Sola E, Sole C, Simon-Talero M, Martin-Llahi M, Castellote J, Garcia-Martinez R, Moreira R, Torrens M, Marquez F, Fabrellas N, et al. Midodrine and albumin for prevention of complications in patients with cirrhosis awaiting liver transplantation. A randomized placebo-controlled trial. J Hepatol. 2018; 69:1250–1259. https://doi.org/10.1016/j.jhep.2018.08.006 [PubMed]
- 23. Caraceni P, Riggio O, Angeli P, Alessandria C, Neri S, Foschi FG, Levantesi F, Airoldi A, Boccia S, Svegliati-Baroni G, et al. Long-term albumin administration in decompensated cirrhosis (ANSWER): an open-label randomised trial. The Lancet. 2018; 391:2417–2429. https://doi.org/10.1016/s0140-6736(18)30840-7 [PubMed]
- 24. Di Pascoli M, Fasolato S, Piano S, Bolognesi M, Angeli P. Long-term administration of human albumin improves survival in patients with cirrhosis and refractory ascites. Liver Int. 2019; 39:98–105. https://doi.org/10.1111/liv.13968 [PubMed]
- 25. Simon-Talero M, Garcia-Martinez R, Torrens M, Augustin S, Gomez S, Pereira G, Guevara M, Gines P, Soriano G, Roman E, et al. Effects of intravenous albumin in patients with cirrhosis and episodic hepatic encephalopathy: a randomized double-blind study. J Hepatol. 2013; 59:1184–1192. https://doi.org/10.1016/j.jhep.2013.07.020 [PubMed]
- 26. Sharma BC, Singh J, Srivastava S, Sangam A, Mantri AK, Trehanpati N, Sarin SK. Randomized controlled trial comparing lactulose plus albumin versus lactulose alone for treatment of hepatic encephalopathy. J Gastroenterol Hepatol. 2017; 32:1234–1239. https://doi.org/10.1111/jgh.13666 [PubMed]
- 27. Jalan R, Kapoor D. Reversal of diuretic-induced hepatic encephalopathy with infusion of albumin but not colloid. Clin Sci (Lond). 2004; 106:467–474. https://doi.org/10.1042/CS20030357 [PubMed]
- 28. Montagnese S, Russo FP, Amodio P, Burra P, Gasbarrini A, Loguercio C, Marchesini G, Merli M, Ponziani FR, Riggio O, et al. Hepatic encephalopathy 2018: A clinical practice guideline by the Italian Association for the Study of the Liver (AISF). Dig Liver Dis. 2019; 51:190–205. https://doi.org/10.1016/j.dld.2018.11.035 [PubMed]
- 29. Riggio O, Nardelli S, Pasquale C, Pentassuglio I, Gioia S, Onori E, Frieri C, Salvatori FM, Merli M. No effect of albumin infusion on the prevention of hepatic encephalopathy after transjugular intrahepatic portosystemic shunt. Metab Brain Dis. 2016; 31:1275–1281. https://doi.org/10.1007/s11011-015-9713-x [PubMed]
- 30. Planas R, Gines P, Arroyo V, Llach J, Panes J, Vargas V, Salmeron JM, Gines A, Toledo C, Rimola A, et al. Dextran-70 versus albumin as plasma expanders in cirrhotic patients with tense ascites treated with total paracentesis. Results of a randomized study. Gastroenterology. 1990; 99:1736–1744. https://doi.org/10.1016/0016-5085(90)90481-f [PubMed]
- 31. Arora V, Maiwall R, Thomas SS, Rajan V, Ali R, Kumar G, Jain P, Sarin SK. Albumin decreases the incidence of paracentesis induced circulatory dysfunction with less than 5 litres of ascitic tap in acute on chronic liver failure (ACLF) patients: Randomized controlled trial (NCT02467348). Journal of Hepatology. 2018; 68:S42–S43. https://doi.org/10.1016/s0168-8278(18)30303-9
- 32. Wilkinson P, Sherlock S. The effect of repeated albumin infusions in patients with cirrhosis. Lancet. 1962; 2:1125–1129.
- 33. Arroyo V. Review article: albumin in the treatment of liver diseases—new features of a classical treatment. Aliment Pharmacol Ther. 2002; 16 Suppl 5:1–5. https://doi.org/10.1046/j.1365-2036.16.s5.1.x [PubMed]
- 34. Bajaj JS, O'Leary JG, Wong F, Kamath PS. Variations in albumin use in patients with cirrhosis: An AASLD members survey. Hepatology. 2015; 62:1923–1924. https://doi.org/10.1002/hep.27789 [PubMed]
- 35. Caraceni P, Pavesi M, Baldassarre M, Bernardi M, Arroyo V. The use of human albumin in patients with cirrhosis: a European survey. Expert Rev Gastroenterol Hepatol. 2018; 12:625–632. https://doi.org/10.1080/17474124.2018.1460203 [PubMed]
- 36. Runyon BA, AASLD. Introduction to the revised American Association for the Study of Liver Diseases Practice Guideline management of adult patients with ascites due to cirrhosis 2012. Hepatology. 2013; 57:1651–1653. https://doi.org/10.1002/hep.26359 [PubMed]
- 37. European Association for the Study of the L. EASL clinical practice guidelines on the management of ascites, spontaneous bacterial peritonitis, and hepatorenal syndrome in cirrhosis. J Hepatol. 2010; 53:397–417. https://doi.org/10.1016/j.jhep.2010.05.004 [PubMed]
- 38. Jain L, Sharma BC, Sharma P, Srivastava S, Agrawal A, Sarin SK. Serum endotoxin and inflammatory mediators in patients with cirrhosis and hepatic encephalopathy. Dig Liver Dis. 2012; 44:1027–1031. https://doi.org/10.1016/j.dld.2012.07.002 [PubMed]
- 39. Odeh M. Pathogenesis of hepatic encephalopathy: the tumour necrosis factor-alpha theory. Eur J Clin Invest. 2007; 37:291–304. https://doi.org/10.1111/j.1365-2362.2007.01778.x [PubMed]
- 40. Duchini A, Govindarajan S, Santucci M, Zampi G, Hofman FM. Effects of tumor necrosis factor-alpha and interleukin-6 on fluid-phase permeability and ammonia diffusion in CNS-derived endothelial cells. J Investig Med. 1996; 44:474–482. [PubMed]
- 41. Balzano T, Dadsetan S, Forteza J, Cabrera-Pastor A, Taoro-Gonzalez L, Malaguarnera M, Gil-Perotin S, Cubas-Nunez L, Casanova B, Castro-Quintas A, et al. Chronic hyperammonemia induces peripheral inflammation that leads to cognitive impairment in rats: reversal by anti-tnfa treatment. J Hepatol. 2019. [Epub ahead of print]. https://doi.org/10.1016/j.jhep.2019.01.008 [PubMed]
- 42. He XM, Carter DC. Atomic structure and chemistry of human serum albumin. Nature. 1992; 358:209–215. https://doi.org/10.1038/358209a0 [PubMed]
- 43. Oettl K, Birner-Gruenberger R, Spindelboeck W, Stueger HP, Dorn L, Stadlbauer V, Putz-Bankuti C, Krisper P, Graziadei I, Vogel W, et al. Oxidative albumin damage in chronic liver failure: relation to albumin binding capacity, liver dysfunction and survival. J Hepatol. 2013; 59:978–983. https://doi.org/10.1016/j.jhep.2013.06.013 [PubMed]
- 44. Arroyo V, Garcia-Martinez R, Salvatella X. Human serum albumin, systemic inflammation, and cirrhosis. J Hepatol. 2014; 61:396–407. https://doi.org/10.1016/j.jhep.2014.04.012 [PubMed]
- 45. Dziarski R. Cell-bound albumin is the 70-kDa peptidoglycan-, lipopolysaccharide-, and lipoteichoic acid-binding protein on lymphocytes and macrophages. J Biol Chem. 1994; 269:20431–20436. [PubMed]
- 46. Jiang W, Desjardins P, Butterworth RF. Hypothermia attenuates oxidative/nitrosative stress, encephalopathy and brain edema in acute (ischemic) liver failure. Neurochem Int. 2009; 55:124–128. https://doi.org/10.1016/j.neuint.2009.02.007 [PubMed]
- 47. Montoliu C, Cauli O, Urios A, ElMlili N, Serra MA, Giner-Duran R, Gonzalez-Lopez O, Del Olmo JA, Wassel A, Rodrigo JM, et al. 3-nitro-tyrosine as a peripheral biomarker of minimal hepatic encephalopathy in patients with liver cirrhosis. Am J Gastroenterol. 2011; 106:1629–1637. https://doi.org/10.1038/ajg.2011.123 [PubMed]
- 48. Bosoi CR, Rose CF. Oxidative stress: a systemic factor implicated in the pathogenesis of hepatic encephalopathy. Metab Brain Dis. 2013; 28:175–178. https://doi.org/10.1007/s11011-012-9351-5 [PubMed]
- 49. Garcia-Martinez R, Cordoba J. Acute-on-chronic liver failure: the brain. Curr Opin Crit Care. 2011; 17:177–183. https://doi.org/10.1097/MCC.0b013e328344b37e [PubMed]
- 50. Roche M, Rondeau P, Singh NR, Tarnus E, Bourdon E. The antioxidant properties of serum albumin. FEBS Lett. 2008; 582:1783–1787. https://doi.org/10.1016/j.febslet.2008.04.057 [PubMed]
- 51. Bal W, Sokolowska M, Kurowska E, Faller P. Binding of transition metal ions to albumin: sites, affinities and rates. Biochim Biophys Acta. 2013; 1830:5444–5455. https://doi.org/10.1016/j.bbagen.2013.06.018 [PubMed]
- 52. Stohs SJ, Bagchi D. Oxidative mechanisms in the toxicity of metal ions. Free Radic Biol Med. 1995; 18:321–336. https://doi.org/10.1016/0891-5849(94)00159-h [PubMed]
- 53. Bruschi M, Candiano G, Santucci L, Ghiggeri GM. Oxidized albumin. The long way of a protein of uncertain function. Biochim Biophys Acta. 2013; 1830:5473–5479. https://doi.org/10.1016/j.bbagen.2013.04.017 [PubMed]
- 54. Carter DC, He XM, Munson SH, Twigg PD, Gernert KM, Broom MB, Miller TY. Three-dimensional structure of human serum albumin. Science. 1989; 244:1195–1198. https://doi.org/10.1126/science.2727704 [PubMed]
- 55. Evans TW. Review article: albumin as a drug—biological effects of albumin unrelated to oncotic pressure. Aliment Pharmacol Ther. 2002; 16 Suppl 5:6–11. https://doi.org/10.1046/j.1365-2036.16.s5.2.x [PubMed]
- 56. Guevara M, Baccaro ME, Torre A, Gomez-Anson B, Rios J, Torres F, Rami L, Monte-Rubio GC, Martin-Llahi M, Arroyo V, et al. Hyponatremia is a risk factor of hepatic encephalopathy in patients with cirrhosis: a prospective study with time-dependent analysis. Am J Gastroenterol. 2009; 104:1382–1389. [PubMed]
- 57. Bossen L, Gines P, Vilstrup H, Watson H, Jepsen P. Serum sodium as a risk factor for hepatic encephalopathy in patients with cirrhosis and ascites. J Gastroenterol Hepatol. 2019; 34:914. https://doi.org/10.1111/jgh.14558 [PubMed]
- 58. Bajaj JS, Tandon P, O'Leary JG, Biggins SW, Wong F, Kamath PS, Garcia-Tsao G, Maliakkal B, Lai JC, Fallon M, et al. The Impact of Albumin Use on Resolution of Hyponatremia in Hospitalized Patients With Cirrhosis. Am J Gastroenterol. 2018; 113:1339. https://doi.org/10.1038/s41395-018-0119-3 [PubMed]
- 59. Nguyen MK, Ornekian V, Kao L, Butch AW, Kurtz I. Defining the role of albumin infusion in cirrhosis-associated hyponatremia. Am J Physiol Gastrointest Liver Physiol. 2014; 307:G229–232. https://doi.org/10.1152/ajpgi.00424.2013 [PubMed]
- 60. Pugh RN, Murray-Lyon IM, Dawson JL, Pietroni MC, Williams R. Transection of the oesophagus for bleeding oesophageal varices. Br J Surg. 1973; 60:646–649. https://doi.org/10.1002/bjs.1800600817 [PubMed]
- 61. Kamath PS, Kim WR, Advanced Liver Disease Study G. The model for end-stage liver disease (MELD). Hepatology. 2007; 45:797–805. https://doi.org/10.1002/hep.21563 [PubMed]
- 62. Ferenci P, Lockwood A, Mullen K, Tarter R, Weissenborn K, Blei AT. Hepatic encephalopathy—definition, nomenclature, diagnosis, and quantification: final report of the working party at the 11th World Congresses of Gastroenterology, Vienna, 1998. Hepatology. 2002; 35:716–721. https://doi.org/10.1053/jhep.2002.31250 [PubMed]


