Introduction
Skin photoaging is a complex process, which has many pathological similarities with skin injury. Histopathologically, it is mainly manifested by the decrease of collagen and the change of elastic fiber degeneration and deposition. External aging is regulated by complex environmental factors, including smoking, chemical exposure, and ultraviolet exposure [1, 2]. Ultraviolet irradiation reduces type I collagen through two mutually regulated pathways that stimulate collagen degradation and inhibit procollagen synthesis [3]. The decrease of type I procollagen synthesis induced by ultraviolet radiation is an important factor in the pathophysiology of skin photoaging [4]. Collagen remodeling is the most important process of skin regeneration in light injury; fibroblasts are the most important collagen-producing cells in collagen remodeling [1]. The UV radiation-induced photo-oxidation is the main damaging factor for the connective tissue of the skin. Yet, there is evidence that intrinsic and extrinsic aging processes have, at least in part, common biological, biochemical, and molecular mechanisms [5].
Cell therapy and laser therapy have been widely used in the treatment of photoaging skin. Fractional lasers, both ablative and non-ablative, are effective and safe, and have been used in a complementary manner for treating photoaged skin [6]. Conventional carbon dioxide (CO2) lattice laser is recognized as a “golden standard” measure to treat facial skin photoaging. It improves skin photoaging through the principle of focal photothermal action [7]. Fractional CO2 laser resurfacing has been used in the treatment of photoaging Asian population with a continued efficacy for up to 5 years [8].
Adult skin is composed of type I and III collagen; the type I collagen accounts for about 80% of skin collagen [9]. In dermis, type I collagen gathers into thick fibrous bundles parallel to the skin surface, interweaves into nets, and has a high mechanical stability. Type I collagen is an important component for maintaining skin tension, plumpness, and fullness [9]. Sunlight can affect type I collagen production, resulting in the reduction of mature collagen bundles, skin relaxation, and wrinkles. Other components in the matrix, such as aminopolysaccharides and proteoglycans, are also associated with photoaging [10].
The signaling protein SMAD3 promotes fibroblast proliferation, and induces synthesis and secretion of extracellular matrix proteins including collagen I. SMAD3 is down-regulated in photoaging cells, and is involved in skin photoaging [11]. In this study, we used primary human fibroblasts and a rat animal model to investigate the effect of CO2 lattice laser on skin photoaging.
Results
CO2 lattice laser promotes fibroblast proliferation
Using different doses of laser irradiation, MTT results showed that CO2 lattice laser could promote fibroblast proliferation, and the proliferation was enhanced with increasing laser dosage (Figure 1A). However, there was no significant difference in the proliferation ability between 3.75 mJ/cm2 irradiation group and 6.25 mJ/cm2 irradiation group. CO2 lattice laser also inhibited cell senescence by down-regulating production of reactive oxygen species (ROS) and malondialdehyde (MDA), and up-regulating expression of superoxide dismutase (SOD) (Figure 1B–1D). In addition, CO2 lattice laser increased gene and protein expression of SMAD3 (Figure 1E, 1F).
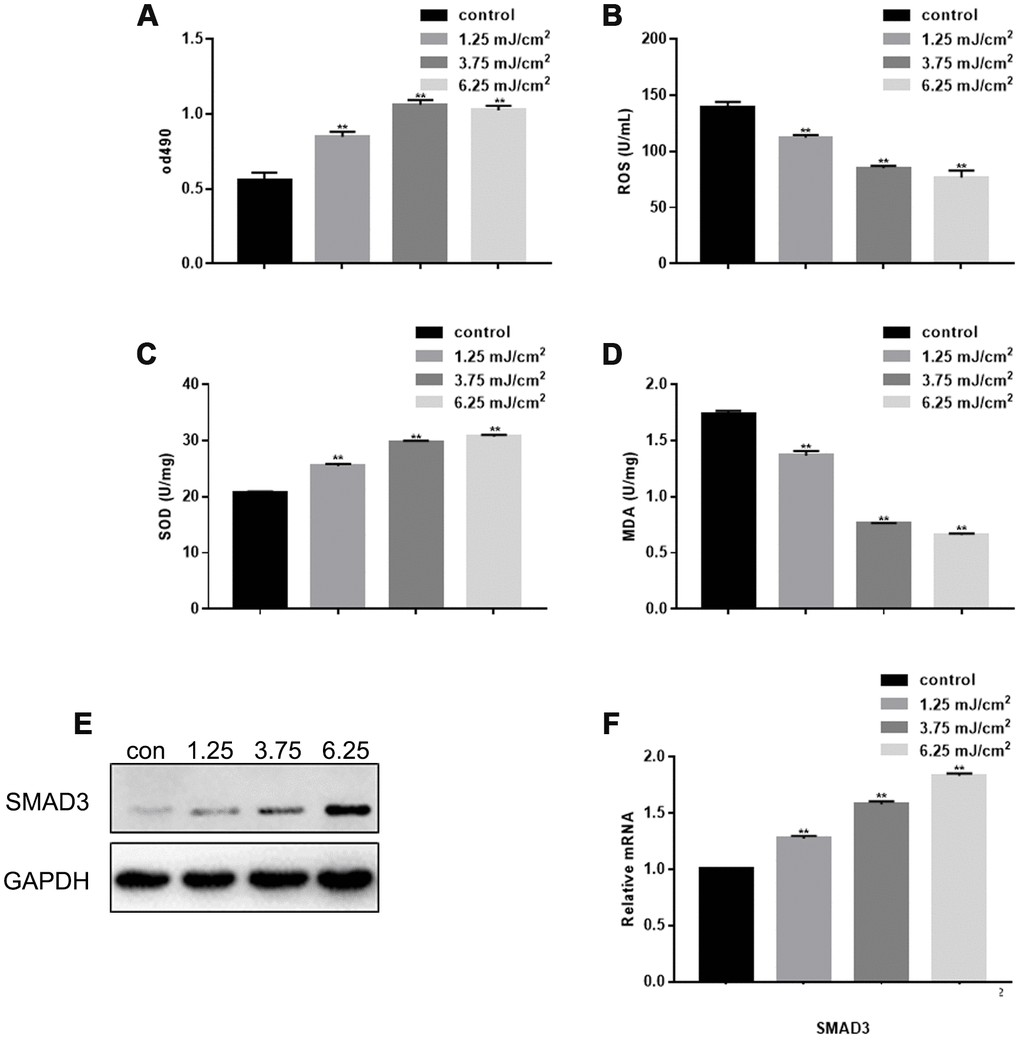
Figure 1. Effect of CO2 Lattice Laser on Fibroblasts. (A) Cell proliferation analyzed by MTT assay after treatment with 0, 1.25, 3.75 and 6.25 mJ/cm2 CO2 Lattice Laser. Data are shown as mean ± SEM.** P< 0.05 vs. 0 mJ/cm2 (B) ROS analyzed by ELISA in cells irradiated by CO2 lattice. Data are shown as mean ± SEM.** P< 0.05 vs. 0 mJ/cm2 (C) SOD expression analyzed by ELISA in cells irradiated by CO2 lattice laser. Data are shown as mean ± SEM.** P< 0.05 vs. 0 mJ/cm2 (D) MDA expression analyzed by ELISA in cells irradiated by CO2 lattice laser. Data are shown as mean ± SEM.** P< 0.05 vs. 0 mJ/cm2 (E, F) Western blotting and RT-PCR of SMAD3 in cells treated with 0, 1.25, 3.75 and 6.25 mJ/cm2 CO2 Lattice Laser; ** P< 0.05 vs. 0 mJ/cm2.
CO2 lattice laser suppresses cell senescence induced by UVB
As shown previously, UVB irradiation inhibited fibroblast proliferation, promoted expression of ROS and MDA, and inhibited expression of SOD (Figure 2A–2D). The inhibition of fibroblast proliferation and SOD expression, and the up-regulation of ROS and MDA induced by UVB irradiation were restored by CO2 lattice laser irradiation (Figure 2A–2D). In addition, UVB irradiation induced cell cycle arrest in G1 phase, and increased fibroblast apoptosis. However, the cell cycle arrest and apoptosis were reversed after CO2 lattice laser treatment (Figure 2E, 2F). Furthermore, CO2 lattice laser up-regulated gene and protein expression of SMAD3, CDK4, Bcl-2, and collagen 1 (COL1), which were down-regulated by UVB irradiation (Figure 2G, 2H).
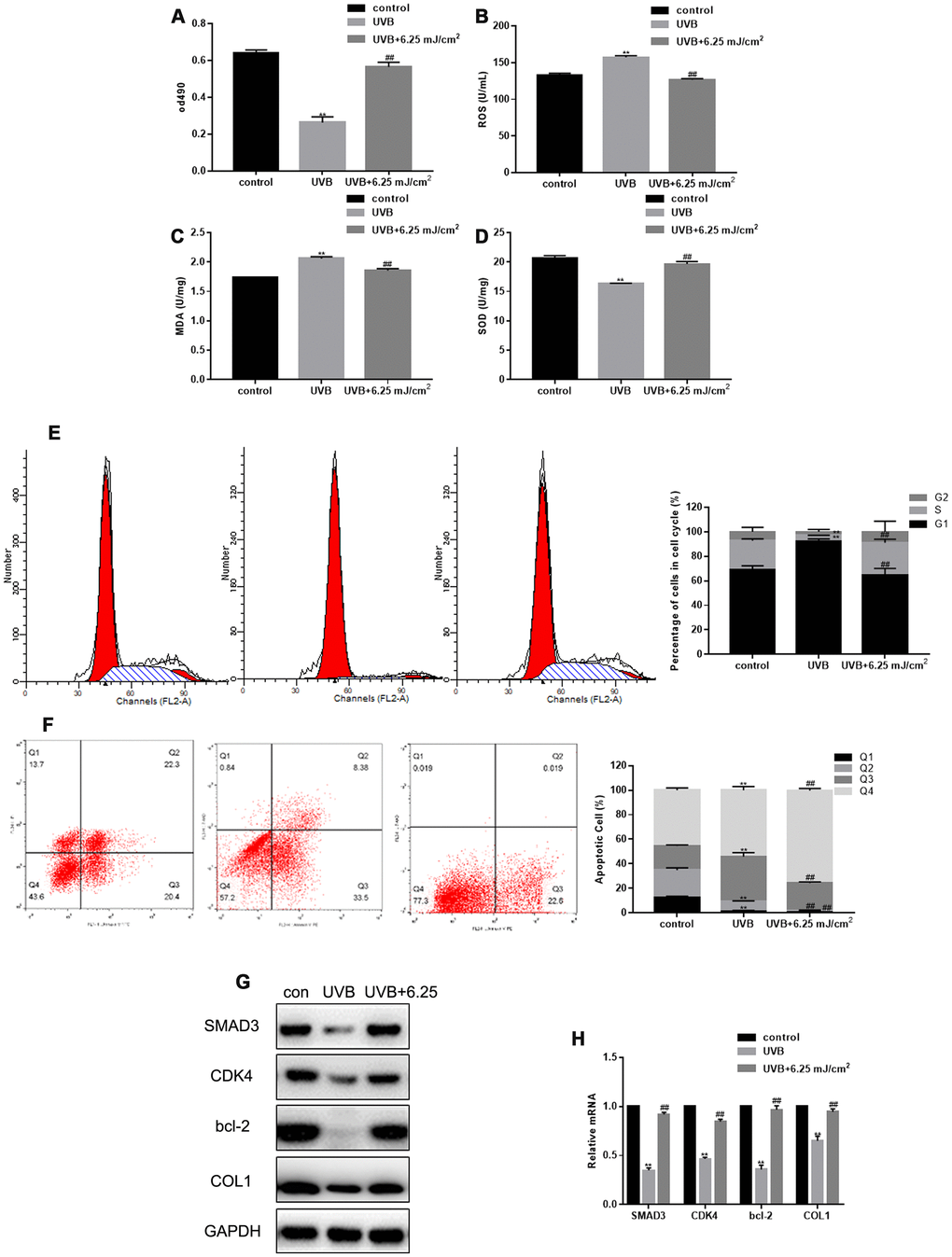
Figure 2. CO2 lattice laser suppresses cell senescence induced by UVB. (A) Proliferation of fibroblasts treated with control, UVB, or UVB and 6.25 mJ/cm2 CO2 Lattice Laser. Data are shown as mean ± SEM;** P< 0.05 vs. control, ## P< 0.05 vs. UVB. (B) ELISA of ROS production in cells irradiated by control, UVB, or UVB and 6.25 mJ/cm2 CO2 Lattice Laser. Data are shown as mean ± SEM;** P< 0.05 vs. control, ## P< 0.05 vs. UVB. (C) ELISA of SOD in cells irradiated by control, UVB or UVB and 6.25 mJ/cm2 CO2 Lattice Laser. Data are shown as mean ± SEM;** P< 0.05 vs. control, ## P< 0.05 vs. UVB. (D) ELISA of MDA in cells irradiated by control, UVB or UVB and 6.25 mJ/cm2 CO2 Lattice Laser. Data are shown as mean ± SEM;** P< 0.05 vs. control, ## P< 0.05 vs. UVB (E) Cell cycle analyzed by flow cytometry after treatment with control, UVB or UVB and 6.25 mJ/cm2 CO2 Lattice Laser. Data are shown as mean ± SEM.** P< 0.05 vs. control, ## P< 0.05 vs. UVB. (F) Apoptosis was detected by Annexin V-PI after treatment with control, UVB or UVB and 6.25 mJ/cm2 CO2 Lattice Laser. Data are shown as mean ± SEM.** P< 0.05 vs. control, ## P< 0.05 vs. UVB. (G, H) Expression of SMAD3, CDK4, Bcl-2, and COL1 analyzed by western blotting and RT-PCR. Data are shown as mean ± SEM;** P< 0.05 vs. control, ## P< 0.05 vs. UVB.
CO2 lattice laser reduces cell senescence through SMAD3
SMAD3 silencing inhibited fibroblast proliferation, but the proliferation was restored after CO2 laser irradiation (Figure 3A). SMAD3 silencing also increased the levels of ROS, up-regulated the expression of MDA, and down-regulated the expression of SOD; however, this effect was alleviated by CO2 lattice laser irradiation (Figure 3B–3D). In addition, CO2 lattice laser increased the expression of CDK4, Bcl-2, and COL1 induced by silencing SMAD3 (Figure 3E, 3F).
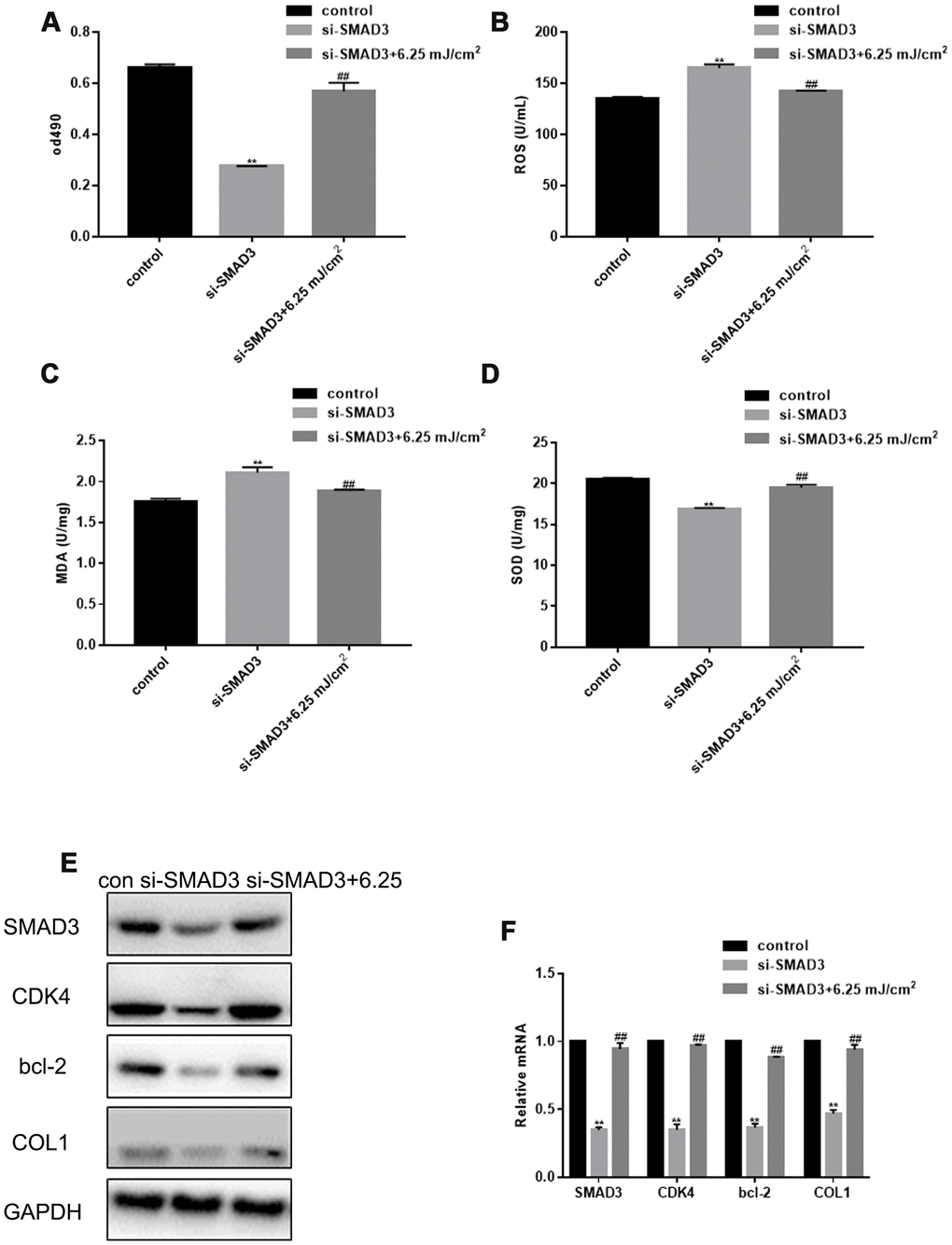
Figure 3. CO2 Lattice Laser Reduces Cell Senescence through SMAD3. (A) Proliferation of fibroblasts treated with control, si-SMAD3 or si-SMAD3 and 6.25 mJ/cm2 CO2 Lattice Laser. Data are shown as mean ± SEM.** P< 0.05 vs. control, ## P< 0.05 vs. si-SMAD3. (B) ROS production in cells irradiated by control, si-SMAD3 or si-SMAD3 and 6.25 mJ/cm2 CO2 Lattice Laser. Data are shown as mean ± SEM.** P< 0.05 vs. control, ## P< 0.05 vs. si-SMAD3. (C) MDA expression in cells irradiated by control, si-SMAD3 or si-SMAD3 and 6.25 mJ/cm2 CO2 Lattice Laser. Data are shown as mean ± SEM.** P< 0.05 vs. control, ## P< 0.05 vs. si-SMAD3. (D) SOD expression in cells irradiated by control, si-SMAD3 or si-SMAD3 and 6.25 mJ/cm2 CO2 Lattice Laser. Data are shown as mean ± SEM.** P< 0.05 vs. control, ## P< 0.05 vs. si-SMAD3. (E, F) Expression of SMAD3, CDK4, Bcl-2, and COL1 analyzed by western blotting and RT-PCR in cells treated with control, si-SMAD3 or si-SMAD3 and 6.25 mJ/cm2 CO2 Lattice Laser. Data are shown as mean ± SEM;** P< 0.05 vs. control, ## P< 0.05 vs. si-SMAD3.
Therapeutic effect of CO2 lattice laser on photoaging of rat skin
After UVB irradiation of rat skin, the dermis became thinner and the skin structure was disordered. In the control group, the structure of the epidermis was complete, the cell layers were clear, the thickness of the dermis was normal, the wavy fibrous tissues could be seen clearly, and the distribution was uniform and dense. However, after UVB irradiation, the epidermis was thickened with hyperkeratosis, had an unclear cell stratification, uneven distribution and disordered arrangement of cortical fibers, the diameter of collagen fibers increased, and inflammatory cells infiltrated the cross section. Importantly, in the treatment group, the thickness of skin and dermis significantly increased, and new, dense, and fine collagen fibers appeared in the superficial dermis, while some denatured and curly fibers were metabolized (Figure 4A, 4B). CO2 lattice laser treatment down-regulated the expression of ROS and MDA induced by UVB irradiation (Figure 4C, 4D). In addition, CO2 lattice laser treatment up-regulated the SOD expression reduced by UVB irradiation (Figure 4E). After CO2 lattice laser irradiation, the tissue expression of SMAD3, CDK4, Bcl-2, and COL1 significantly increased compared with the UVB irradiation group (Figure 4F, 4G).
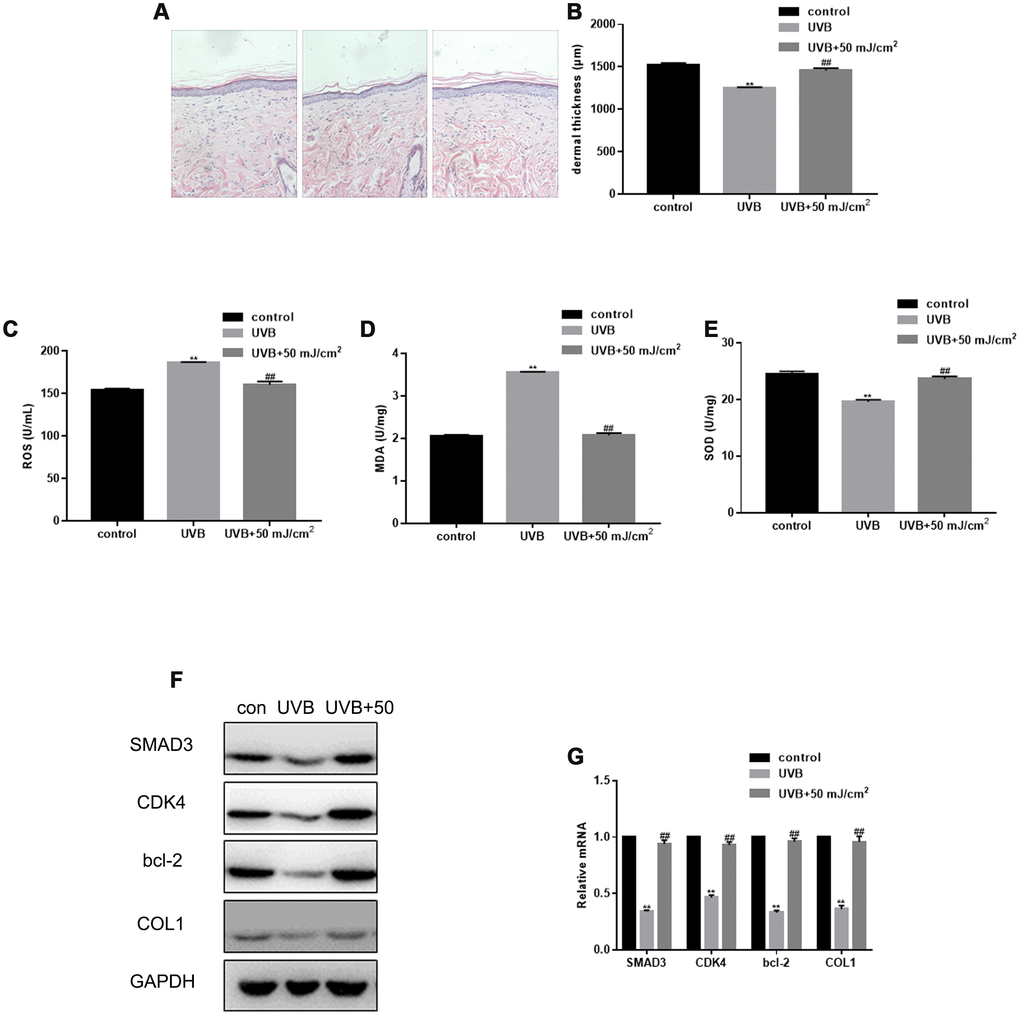
Figure 4. Therapeutic effect of CO2 lattice laser on photoaging of rat skin. (A) HE staining of skin structures in control, UVB irradiation, and CO2 lattice laser treatment groups. (B) Dermal thickness in control, UVB irradiation, and CO2 lattice laser treatment groups. Data are shown as mean ± SEM;** P< 0.05 vs. control, ## P< 0.05 vs. UVB. (C) ROS production analyzed by ELISA in cells irradiated by control, UVB, or UVB and 50 mJ/cm2 CO2 Lattice Laser. Data are shown as mean ± SEM.** P< 0.05 vs. control, ## P< 0.05 vs. UVB. (D) ELISA of MDA in cells irradiated by control, UVB or UVB and 50 mJ/cm2 CO2 Lattice Laser. Data are shown as mean ± SEM.** P< 0.05 vs. control, ## P< 0.05 vs. UVB. (E) ELISA of SOD in cells irradiated by control, UVB or UVB and 50 mJ/cm2 CO2 Lattice Laser. Data are shown as mean ± SEM.** P< 0.05 vs. control, ## P< 0.05 vs. UVB. (F, G) Expression of SMAD3, CDK4, Bcl-2, and COL1 analyzed by western blotting and RT-PCR in control, si-SMAD3 or si-SMAD3 and 6.25 mJ/cm2 CO2 Lattice Laser groups. Data are shown as mean ± SEM.** P< 0.05 vs. control, ## P< 0.05 vs. UVB.
Discussion
Photoaging refers to the aging process of skin caused by long-term exposure to ultraviolet light. Among the ultraviolet rays which cause photoaging, medium-wave ultraviolet light is especially damaging because of its high energy and strong penetration ability [14]. It can damage DNA, and induce expression of DNA damage repair factors and cell cycle regulatory proteins, resulting in a decreased fibroblast proliferation [15]. Exposure to UVA radiation can damage DNA and induce oxidative stress by generating ROS and MDA. SOD is a major antioxidant enzyme that provides a defense against the cell damage induced by oxidative stress [16]. UV can induce high concentration of ROS in the skin, resulting in photoaging [17]. In addition, MDA, a lipid peroxidation product, accumulates in the skin during aging, and mediates photoaging [18]. In contrast, SOD has an anti-aging effect [19]. In this study, we have evaluated the effect of UVB and CO2 laser on ROS, MDA, and SOD levels in skin cells during photoaging.
Previous studies have used cultured human primary fibroblasts to study the effect of UVB exposure on photoaging [20–22]. However, a single dose of UVB irradiation is difficult to control, and the effect greatly depends on the cell state. When the dosage is too high, cells undergo apoptosis; however, when the dosage is too low, cells can restore their normal functions through repair mechanisms [23]. Using a stable model of photoaging, our results show that UVB irradiation reduces fibroblast proliferation, blocks cell cycle in G1 phase, and increases apoptosis.
CO2 lattice laser is effective in repairing wrinkles and photoaging skin [24]. The combination of CO2 laser and RF(radio frequency) can be used to treat acne scars and various skin aging diseases [25–27]. It can promote epidermal reconstruction, dermal repair, and wound healing [28, 29]. Several recent studies have explored the therapeutic effect of laser on photoaging, but the mechanisms of its action are unknown [30]. CO2 and erbium: yttriumaluminum-garnet lasers, which can remove the stratum corneum, have been regarded as the gold standard for skin laser resurfacing. Fractional lasers combined with intense pulsed light therapy are expected to produce better efficacy with fewer side-effects for the treatment of photoaging skin [7]. A recent report has described the utility of a combined approach of fractional ablative CO2 with full-field erbium ablation for full face rejuvenation [31]. Rejuvenation with the fractional ablative carbon dioxide laser decreases the symptoms of facial aging in more than half of the patients [32]. Although many studies investigated the effect of CO2 laser on photoaging, most of them were clinical studies, and few of them analyzed the underlying mechanisms. In this study, we found that different doses of low concentration CO2 lattice laser irradiation could promote fibroblast proliferation.
Activation of SMAD3 promotes cell division and proliferation of fibroblasts, monocytes, and lymphocytes. SMAD3 induces collagen I synthesis, inhibits activation of matrix metalloproteinase, enhances expression of fibronectin, and reduces degradation of collagen fibers and extracellular matrix in fibroblasts [33]. In addition, it can stimulate fibroblast proliferation and inhibit fibroblast apoptosis by activating the MAPK pathway, thereby increasing the synthesis of collagen and elastic fibers [34]. This is the first study that focuses on the regulation of Smad3 by CO2 laser and UVB irradiation, and demonstrates that CO2 lattice laser irradiation promotes proliferation of human primary fibroblasts, down-regulates the levels of ROS and MDA, and induces the expression of SOD and SMAD3. In addition, our results show that CO2 lattice laser can up-regulate the expression of SMAD3, CDK4, Bcl-2, and COL1 down-regulated by UVB irradiation. CO2 lattice laser can reverse the aging of fibroblasts caused by UVB. Furthermore, CO2 lattice laser can reverse the cell senescence induced by SMAD3 silencing, indicating that the therapeutic effect of CO2 lattice laser is mediated by SMAD3.
The anti-aging effect of laser treatment can be achieved through epidermal reconstruction, dermal extracellular matrix regeneration, and remodeling [35]. This study shows that CO2 lattice laser can activate dermal fibroblasts, reduce UVB-induced cell cycle arrest and apoptosis, and stimulate collagen synthesis. Our HE staining results show that after the CO2 lattice laser treatment, the collagen expression increased, epidermis became thinner, dermis thickness increased, and inflammatory cell infiltration improved, demonstrating that the CO2 lattice laser treatment can have profound therapeutic effects on photoaging skin. In summary, our in vitro and in vivo data show that the CO2 lattice laser can reverse the skin aging caused by UVB, and indicate that this effect is mediated through SMAD3.
Materials and Methods
Cells
Healthy skin tissues were obtained from 6 patients who underwent skin flap surgery in our hospital from May 2013 to May 2014. All patients signed the informed consent, and all procedures were approved by the Ethics Committee of the General Hospital of Northern Theater Command. The obtained healthy skin tissues were cut into fragments under aseptic conditions, and the epidermis and dermis were separated to obtain skin primary fibroblasts. Tissues were digested with type I collagenase and cultured in Dulbecco modified Eagle medium (DMEM, Hyclone, China) containing 10% fetal bovine serum (FBS, Hyclone, China), at 37 °C under 5 % CO2. The study was conducted using 2-5 generations of fibroblasts [12].
Ultraviolet B (UVB) irradiation cell model
Primary fibroblasts with good cell viability and rapid proliferation were selected for the experiment. When the confluence was about 50%, the culture dish or six-well plate were taken out, the culture medium was discarded, cells were covered with PBS, and irradiated under UVB lamp tube at doses of 60 mJ/cm2. After each irradiation, DMEM medium was added. The interval time of irradiation was 12 h, 4 times in total.
CO2 lattice laser therapy
Cells were treated with CO2 lattice laser (wavelength 10600 nm, spot size 9 mm * 9 mm, spot 0.125 mm, energy 0, 1.25, 3.75 and 6.25 mJ/cm2, frequency 5 Hz, repetition delay time 0.5 s). The experiment was carried out 24 h after irradiation.
MTT assay
Cell proliferation was analyzed by the MTT tetrazolium assay. Cells were incubated with MTT solution for 4 h, and absorbance was measured at 490 nm.
Reactive oxygen species (ROS), superoxide dismutase (SOD), and malondialdehyde (MDA) assays
ROS were determined by ROS kit, SOD was determined by SOD kit, and MDA was determined by MDA kit, according to the manufacturer’s instructions (Shanghai Renjie Biotechnology Co., Ltd., China, Shanghai).
RNA isolation and real time PCR (RT-PCR)
RNA was extracted with Trizol, and converted to DNA using a reverse transcription kit (Roche, China, Beijing). SYBR kit (Roche Company, China, Beijing) was used for RT-PCR; a total of 35 cycles were carried out [13]. Primer sequences were as follows.
| Name | Forward primer (5'->3') | Reverse primer (5'->3') |
| SMAD3 | CGGGACCTCACCGACTACCT | GGGCCGTGATCTCCTTCTG |
| CDK4 | CATGTAGACCAGGACCTAAGG | GGAGGTCGGTACCAGAGTG |
| bcl-2 | TCGCCCTGTGGATGACTG | GCTTGGCAATTAGTGGTC |
| COL1 | GATGCCAATGTGGTTCGTG | TTCTTGCGGCTGCCCTCT |
| GAPDH | TGCGTGACATTAAGGAGAAG | CTGCATCCTGTCGGCAATG |
Western blotting
Proteins were extracted, separated by 10% polyacrylamide gel electrophoresis, and transferred to nitrocellulose membranes. After transfer, the membranes were blocked in 5% bovine serum albumin for 2 h at room temperature, and incubated overnight at 4°C with primary antibodies (SMAD3, CDK4, bcl-2, COL1 and GAPDH) (Santa Cruz, USA), followed by 1 h incubation with a secondary antibody (Santa Cruz, USA). Proteins were quantified by densitometry, and normalized to GAPDH.
Cell cycle and apoptosis assays
For cell cycle analysis, cells were washed with PBS, fixed in ethanol, suspended in PI/RNase staining solution (Shanghai Biyuntian Biotechnology Co., Ltd., Shanghai, China), and analyzed by flow cytometry (FC).
For apoptosis assay, cells were washed with PBS, fixed in ethanol, suspended in Annexin V-PI staining solution (Shanghai Biyuntian Biotechnology Co., Ltd., Shanghai, China), and analyzed by FC.
Animal model
Eighteen SD rats were randomly divided into a control group (6 rats), experimental group (6 rats), and treatment group (6 rats). The experimental and treatment groups were irradiated with UVB ultraviolet lamp (2 h/day, 60 days continuously). After 60 days, the animals in the treatment group were treated with a low energy CO2 lattice laser (wavelength 10600 nm, spot size 9 mm X 9 mm, spot 0.125 mm, energy 50 mJ/cm2, frequency 5 Hz, repetition delay time 0.5 s, coverage rate 10%) for two weeks. All groups were analyzed at the time of treatment completion in the treatment group.
Hematoxylin-eosin (HE) staining
Tissues were fixed in formalin, embedded in paraffin, sliced, and stained with hematoxylin. After washing, the tissues were stained with eosin, and observed under a microscope (200-fold magnification).
Statistical analysis
The data were analyzed by SPSS19.0 statistical analysis software. T test was used to evaluate the differences between the groups; P < 0.05 was considered significant.
Conflicts of Interest
The authors declare no conflicts of interest.
References
- 1. Lin P, Hwang E, Ngo HT, Seo SA, Yi TH. Sambucus nigra L. ameliorates UVB-induced photoaging and inflammatory response in human skin keratinocytes. Cytotechnology. 2019; 71:1003–17. https://doi.org/10.1007/s10616-019-00342-1 [PubMed]
- 2. Xiao Z, Liang P, Chen J, Chen MF, Gong F, Li C, Zhou C, Hong P, Yang P, Qian ZJ. A Peptide YGDEY from Tilapia Gelatin Hydrolysates Inhibits UVB-mediated Skin Photoaging by Regulating MMP-1 and MMP-9 Expression in HaCaT Cells. Photochem Photobiol. 2019; 95:1424–32. https://doi.org/10.1111/php.13135 [PubMed]
- 3. Duan X, Wu T, Liu T, Yang H, Ding X, Chen Y, Mu Y. Vicenin-2 ameliorates oxidative damage and photoaging via modulation of MAPKs and MMPs signaling in UVB radiation exposed human skin cells. J Photochem Photobiol B. 2019; 190:76–85. https://doi.org/10.1016/j.jphotobiol.2018.11.018 [PubMed]
- 4. Yang JE, Ngo HT, Hwang E, Seo SA, Park SW, Yi TH. Dietary enzyme-treated Hibiscus syriacus L. protects skin against chronic UVB-induced photoaging via enhancement of skin hydration and collagen synthesis. Arch Biochem Biophys. 2019; 662:190–200. https://doi.org/10.1016/j.abb.2018.12.020 [PubMed]
- 5. Borges J, Manela-Azulay M, Cuzzi T. Photoaging and the clinical utility of fractional laser. Clin Cosmet Investig Dermatol. 2016; 9:107–14. https://doi.org/10.2147/CCID.S77996 [PubMed]
- 6. Moon HR, Yun WJ, Lee YJ, Lee MW, Chang S. A prospective, randomized, double-blind comparison of an ablative fractional 2940-nm erbium-doped yttrium aluminum garnet laser with a nonablative fractional 1550-nm erbium-doped glass laser for the treatment of photoaged Asian skin. J Dermatolog Treat. 2015; 26:551–57. https://doi.org/10.3109/09546634.2014.999020 [PubMed]
- 7. Mei XL, Wang L. Ablative fractional carbon dioxide laser combined with intense pulsed light for the treatment of photoaging skin in Chinese population: A split-face study. Medicine (Baltimore). 2018; 97:e9494. https://doi.org/10.1097/MD.0000000000009494 [PubMed]
- 8. Tan J, Lei Y, Ouyang HW, Gold MH. The use of the fractional CO2 laser resurfacing in the treatment of photoaging in Asians: five years long-term results. Lasers Surg Med. 2014; 46:750–56. https://doi.org/10.1002/lsm.22304 [PubMed]
- 9. Liu S, You L, Zhao Y, Chang X. Hawthorn Polyphenol Extract Inhibits UVB-Induced Skin Photoaging by Regulating MMP Expression and Type I Procollagen Production in Mice. J Agric Food Chem. 2018; 66:8537–46. https://doi.org/10.1021/acs.jafc.8b02785 [PubMed]
- 10. Sun Z, Du J, Hwang E, Yi TH. Paeonol extracted from Paeonia suffruticosa Andr. ameliorated UVB-induced skin photoaging via DLD/Nrf2/ARE and MAPK/AP-1 pathway. Phytother Res. 2018; 32:1741–49. https://doi.org/10.1002/ptr.6100 [PubMed]
- 11. Liu Z, Li Y, Song H, He J, Li G, Zheng Y, Li B. Collagen peptides promote photoaging skin cell repair by activating the TGF-β/Smad pathway and depressing collagen degradation. Food Funct. 2019; 10:6121–34. https://doi.org/10.1039/C9FO00610A [PubMed]
- 12. Gras C, Ratuszny D, Hadamitzky C, Zhang H, Blasczyk R, Figueiredo C. miR-145 Contributes to Hypertrophic Scarring of the Skin by Inducing Myofibroblast Activity. Mol Med. 2015; 21:296–304. https://doi.org/10.2119/molmed.2014.00172 [PubMed]
- 13. Pfaffl MW. A new mathematical model for relative quantification in real-time RT-PCR. Nucleic Acids Res. 2001; 29:e45. https://doi.org/10.1093/nar/29.9.e45 [PubMed]
- 14. Song D, Park H, Lee SH, Kim MJ, Kim EJ, Lim KM. PAL-12, a new anti-aging hexa-peptoid, inhibits UVB-induced photoaging in human dermal fibroblasts and 3D reconstructed human full skin model, Keraskin-FT™. Arch Dermatol Res. 2017; 309:697–707. https://doi.org/10.1007/s00403-017-1768-6 [PubMed]
- 15. Bravo K, Duque L, Ferreres F, Moreno DA, Osorio E. Passiflora tarminiana fruits reduce UVB-induced photoaging in human skin fibroblasts. J Photochem Photobiol B. 2017; 168:78–88. https://doi.org/10.1016/j.jphotobiol.2017.01.023 [PubMed]
- 16. Li H, Gao A, Jiang N, Liu Q, Liang B, Li R, Zhang E, Li Z, Zhu H. Protective Effect of Curcumin Against Acute Ultraviolet B Irradiation-induced Photo-damage. Photochem Photobiol. 2016; 92:808–15. https://doi.org/10.1111/php.12628 [PubMed]
- 17. Cavinato M, Jansen-Dürr P. Molecular mechanisms of UVB-induced senescence of dermal fibroblasts and its relevance for photoaging of the human skin. Exp Gerontol. 2017; 94:78–82. https://doi.org/10.1016/j.exger.2017.01.009 [PubMed]
- 18. Chen BY, Lin DP, Wu CY, Teng MC, Sun CY, Tsai YT, Su KC, Wang SR, Chang HH. Dietary zerumbone prevents mouse cornea from UVB-induced photokeratitis through inhibition of NF-κB, iNOS, and TNF-α expression and reduction of MDA accumulation. Mol Vis. 2011; 17:854–63. [PubMed]
- 19. Sasaki H, Itoh T, Akamatsu H, Okamoto H, Horio T. Effects of calcium concentration on the SOD activity and UVB-induced cytotoxicity in cultured human keratinocytes. Photodermatol Photoimmunol Photomed. 2005; 21:9–14. https://doi.org/10.1111/j.1600-0781.2005.00117.x [PubMed]
- 20. Lee JJ, An S, Kim KB, Heo J, Cho DH, Oh HM, Kim HS, Bae S. Erratum to: Extract of Ettlia sp. YC001 Exerts Photoprotective Effects against UVB Irradiation in Normal Human Dermal Fibroblast. J Microbiol Biotechnol. 2016; 26:1162. https://doi.org/10.4014/jmb.2016.2606.1162 [PubMed]
- 21. Karthikeyan R, Kanimozhi G, Prasad NR, Agilan B, Ganesan M, Mohana S, Srithar G. 7-Hydroxycoumarin prevents UVB-induced activation of NF-κB and subsequent overexpression of matrix metalloproteinases and inflammatory markers in human dermal fibroblast cells. J Photochem Photobiol B. 2016; 161:170–76. https://doi.org/10.1016/j.jphotobiol.2016.04.027 [PubMed]
- 22. Park MJ, Bae YS. Fermented Acanthopanax koreanum Root Extract Reduces UVB- and H2O2-Induced Senescence in Human Skin Fibroblast Cells. J Microbiol Biotechnol. 2016; 26:1224–33. https://doi.org/10.4014/jmb.1602.02049 [PubMed]
- 23. Chung KW, Choi YJ, Park MH, Jang EJ, Kim DH, Park BH, Yu BP, Chung HY. Molecular Insights into SIRT1 Protection Against UVB-Induced Skin Fibroblast Senescence by Suppression of Oxidative Stress and p53 Acetylation. J Gerontol A Biol Sci Med Sci. 2015; 70:959–68. https://doi.org/10.1093/gerona/glu137 [PubMed]
- 24. Won KH, Lee SH, Lee MH, Rhee DY, Yeo UC, Chang SE. A prospective, split-face, double-blinded, randomized study of the efficacy and safety of a fractional 1064-nm Q-switched Nd:YAG laser for photoaging-associated mottled pigmentation in Asian skin. J Cosmet Laser Ther. 2016; 18:381–86. https://doi.org/10.1080/14764172.2016.1191645 [PubMed]
- 25. Cameli N, Mariano M, Serio M, Ardigò M. Preliminary comparison of fractional laser with fractional laser plus radiofrequency for the treatment of acne scars and photoaging. Dermatol Surg. 2014; 40:553–61. https://doi.org/10.1111/dsu.12470 [PubMed]
- 26. Hwang YJ, Lee YN, Lee YW, Choe YB, Ahn KJ. Treatment of acne scars and wrinkles in asian patients using carbon-dioxide fractional laser resurfacing: its effects on skin biophysical profiles. Ann Dermatol. 2013; 25:445–53. https://doi.org/10.5021/ad.2013.25.4.445 [PubMed]
- 27. Alexiades-Armenakas MR, Dover JS, Arndt KA. Fractional laser skin resurfacing. J Drugs Dermatol. 2012; 11:1274–87. [PubMed]
- 28. Lee HM, Haw S, Kim JK, Chang SE, Lee MW. Split-face study using a 1,927-nm thulium fiber fractional laser to treat photoaging and melasma in Asian skin. Dermatol Surg. 2013; 39:879–88. https://doi.org/10.1111/dsu.12176 [PubMed]
- 29. Sugata K, Osanai O, Sano T, Takema Y. Evaluation of photoaging in facial skin by multiphoton laser scanning microscopy. Skin Res Technol. 2011; 17:1–3. https://doi.org/10.1111/j.1600-0846.2010.00475.x [PubMed]
- 30. Polder KD. Commentary: A split-face study using the 1,927-nm thulium fiber fractional laser for photoaging and melasma in Asian skin. Dermatol Surg. 2013; 39:889–90. https://doi.org/10.1111/dsu.12195 [PubMed]
- 31. Worley B, Cohen JL. Combination Ablative Approach to Laser Therapy in Advanced Aging of the Face. J Drugs Dermatol. 2018; 17:796–99. [PubMed]
- 32. Yalici-Armagan B, Elcin G. Fractional carbon dioxide laser for facial rejuvenation: A prospective study to evaluate the efficacy and the safety. J Cosmet Laser Ther. 2018; 20:2–8. https://doi.org/10.1080/14764172.2017.1358453 [PubMed]
- 33. Chen B, Li R, Yan N, Chen G, Qian W, Jiang HL, Ji C, Bi ZG. Astragaloside IV controls collagen reduction in photoaging skin by improving transforming growth factor-β/Smad signaling suppression and inhibiting matrix metalloproteinase-1. Mol Med Rep. 2015; 11:3344–48. https://doi.org/10.3892/mmr.2015.3212 [PubMed]
- 34. Tanaka H, Yamaba H, Kosugi N, Mizutani H, Nakata S. Fermentable metabolite of Zymomonas mobilis controls collagen reduction in photoaging skin by improving TGF-beta/Smad signaling suppression. Arch Dermatol Res. 2008 (Suppl 1); 300:S57–64. https://doi.org/10.1007/s00403-007-0805-2 [PubMed]
- 35. Jeon Y, Jung Y, Youm JK, Kang KS, Kim YK, Kim SN. Abietic acid inhibits UVB-induced MMP-1 expression in human dermal fibroblast cells through PPARα/γ dual activation. Exp Dermatol. 2015; 24:140–45. https://doi.org/10.1111/exd.12616 [PubMed]


