Introduction
COVID-19 is a serious global public-health concern that has had a startling medical, economic, educational, political, and cultural impact in a number of countries [1–4]. As of 10:00 am Central European Summer Time, 1 August 2020, there have been 17,396,943 confirmed cases of COVID-19, including 675,060 deaths, reported to the WHO (https://covid19.who.int/) [5]. Among them, the Americas, Europe, South-East Asia, Eastern Mediterranean, Africa, and Western Pacific have reported 9,320,330, 3,357,465, 2,072,194, 1,544,994, 788,448, and 312,771 cases, respectively (Figure 1A) [5]. The overall worldwide crude death rate among infected persons is about 3.88%, of which the crude death rates in Europe, Americas, Western Pacific, Eastern Mediterranean, South-East Asia, and Africa are about 6.34%, 3.81%, 2.68%, 2.6%, 2.17%, and 1.72%, respectively (Figure 1B) [5]. With the rapid increase in the number of COVID-19 patients, those with a history of cerebrovascular disease have gradually attracted the attention of clinicians and pathologists. Meta-analyses by Aggarwal et al. [6] and Wang et al. [7] showed that underlying cerebrovascular disease is related to increased disease severity in COVID-19 patients. It is therefore important to identify a history of cerebrovascular disease in COVID-19 patients, which will help to predict their prognosis and support more effective allocation of limited medical resources. Many studies have reported the incidences of cerebrovascular disease as a comorbidity in patients with COVID-19 [8–54]. However, there are moderate differences among these studies. In addition, some are single-center studies and have an insufficient sample size, low population representativeness, and limited universality of conclusions. For those reasons, this meta-analysis was performed to estimate the incidence of a history of cerebrovascular disease among patients with COVID-19.
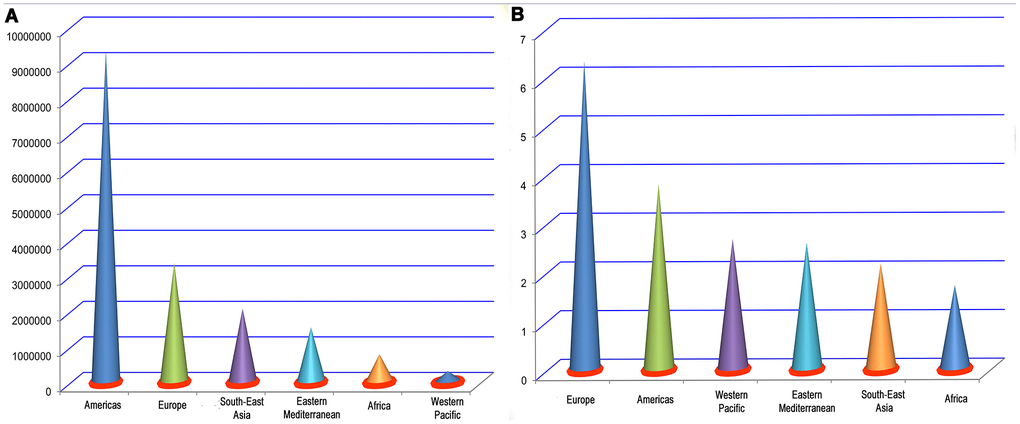
Figure 1. Number of infections (A) and crude death rate (%) (B) by region.
Results
Search and quality assessment results
Using the retrieval strategy summarized in the Methods, a total of 7,190 related studies were evaluated, and 1825 papers remained after 5365 duplicate articles were excluded. After reading the titles and abstracts, 1744 studies that did not meet the inclusion criteria were excluded. After evaluating of the remaining 81 articles applicability by reading the full text, an additional 34 were ruled out based on the exclusion criteria. Ultimately, 47 studies [8–54], including 19 Chinese [8–26] and 28 English language [27–54] studies were included. The PRISMA flow diagram of the literature screening is shown in Figure 2. In addition, the quality assessment and baseline characteristics of the included articles are depicted in Table 1. The studies mainly reported the clinical characteristics of patients with COVID-19, incidences of underlying diseases, and prognoses. The participants in these studies mainly came from China, the United States, the United Kingdom, and Italy. The sample size distribution among these studies was roughly 21 to 5,700. Moreover, there were 3, 14, 10, 7, 7, and 5 studies with quality scores of 3, 4, 5, 6, 7, and 8, respectively. Thus, the literature included in our meta-analysis was of relatively high quality.
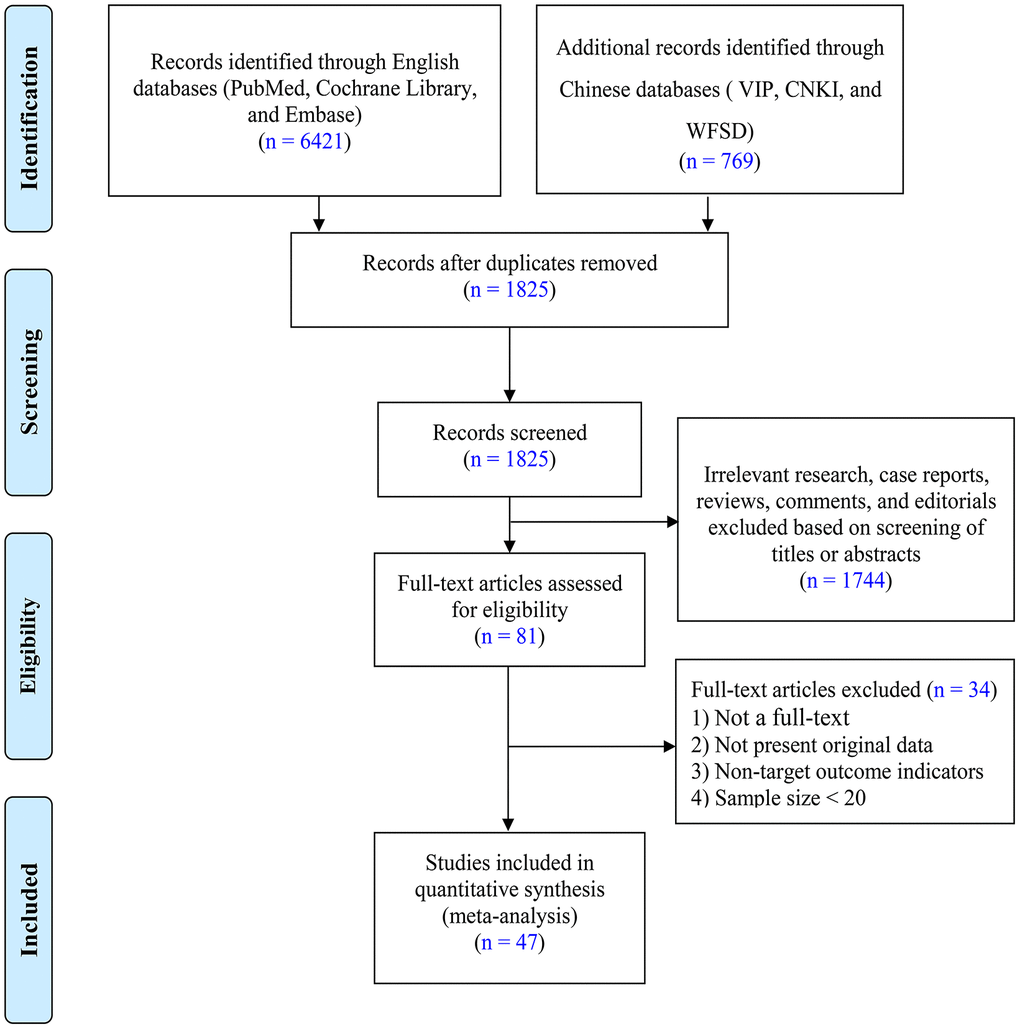
Figure 2. PRISMA flow diagram showing selection of the literature for this meta-analysis.
Table 1. Quality assessment and baseline characteristics of the included studies.
| Study and year | Quality assessment | Country | Publishing language | Sample size | Males/Females | Age | Cerebrovascular disease, (%) | Hypertension, (%) | Dizziness or headache, (%) |
| Li,2020[8] | ★★★★★★ | China | Chinese | 80 | 40/40 | 3-90 | — | 14, (17.5) | 12, (15.0) |
| Yuan,2020[9] | ★★★★★ | China | Chinese | 223 | 106/117 | 46.5±16.1 | — | 25, (11.2) | 11, (4.9) |
| Wang,2020a[10] | ★★★★ | China | Chinese | 32 | 16/16 | — | — | 5, (15.6) | 1, (3.1) |
| Zhang,2020a[11] | ★★★★ | China | Chinese | 61 | 36/25 | 3-85 | — | 15, (24.6) | 9, (14.8) |
| Zuo,2020[12] | ★★★★★ | China | Chinese | 50 | 18/32 | 48.2±15.3 | 2, (4.0) | 9, (18.0) | 3, (6.0) |
| Wang,2020b[13] | ★★★★ | China | Chinese | 96 | 46/50 | — | 3, (3.1) | 50, (52.1) | 2, (2.1) |
| Lei,2020[14] | ★★★★ | China | Chinese | 51 | 25/16 | 26-82 | 1, (1.96) | 9, (17.6) | 1, (1.96) |
| Dong,2020[15] | ★★★★★★ | China | Chinese | 27 | 13/14 | 23-68 | — | 4, (14.8) | 4, (14.8) |
| Zhao,2020[16] | ★★★★ | China | Chinese | 21 | 14/7 | 4-72 | — | 4, (19.0) | 4, (19.0) |
| Tong,2020[17] | ★★★ | China | Chinese | 258 | 133/125 | 46.97±17.8 | 1, (0.39) | 32, (12.4) | — |
| Suo,2020[18] | ★★★★★ | China | Chinese | 171 | 67/104 | 49±20 | — | 24, (14) | 16, (9.4) |
| Zhong,2020[19] | ★★★★ | China | Chinese | 62 | 40/22 | 28-77 | — | — | 2, (3.2) |
| Xu,2020a[20] | ★★★★★ | China | Chinese | 155 | 87/68 | 41.99±15.40 | — | — | 5, (3.2) |
| Gong,2020[21] | ★★★★★★ | China | Chinese | 80 | 45/35 | 18-82 | — | 8, (10.0) | 10, (8.0) |
| Chen,2020a[22] | ★★★★★ | China | Chinese | 67 | 20/47 | 11-85 | — | 12, (17.9) | — |
| Lu,2020[23] | ★★★★★ | China | Chinese | 50 | 28/22 | 50.4±16.8 | — | 8, (16) | — |
| Huang,2020a[24] | ★★★★ | China | Chinese | 35 | 19/16 | 12-74 | — | 1, (2.9) | 3, (8.6) |
| Liang,2020a[25] | ★★★ | China | Chinese | 28 | 16/12 | 24-87 | 1, (3.6) | 9, (32.1) | — |
| Zhuang,2020[26] | ★★★★ | China | Chinese | 26 | 18/8 | 3-79 | — | 4, (15.4) | 6, (23.1) |
| Yang,2020[27] | ★★★★★★ | China | English | 149 | 81/68 | 45.11±13.35 | 0, (0) | — | 13, (8.7) |
| Chen,2020b[28] | ★★★★★★ | China | English | 249 | 126/123 | 51±20.74 | — | — | 28, (11.2) |
| Liu,2020a[29] | ★★★★★ | China | English | 56 | 31/25 | — | — | 10, (17.9) | — |
| Lovell,2020[30] | ★★★★★★★ | British | English | 101 | 64/37 | 82.0±12.6 | 12, (11.9) | 54, (53.5) | — |
| Huang,2020b[31] | ★★★★★★★ | China | English | 41 | 30/11 | 49.0±12.6 | — | 6, (14.6) | 3, (7.9) |
| Chen,2020c[32] | ★★★★★★★ | China | English | 99 | 67/32 | 55.5±13.1 | 1, (1.0) | — | 8, (8.1) |
| Zhou,2020a[33] | ★★★★★★★★ | China | English | 191 | 119/72 | 56.0±15.6 | — | 58, (30.3) | — |
| Goyal,2020[34] | ★★★★ | America | English | 393 | 238/155 | 62.2±18.6 | — | 197, (50.1) | — |
| Guan,2020[35] | ★★★★★★★★ | China | English | 1099 | 640/459 | 47.0±17.0 | 15, (1.4) | 165, (15.0) | 150, (13.6) |
| Chen,2020d[36] | ★★★★★★ | China | English | 203 | 108/95 | 20-91 | 43, (21.2) | 9, (4.4) | 14, (6.9) |
| Qian,2020[37] | ★★★★ | China | English | 91 | 37/54 | 5-96 | — | 15, (16.5) | 7, (7.7) |
| Liu,2020b[38] | ★★★★★★★ | China | English | 137 | 61/76 | 20-83 | — | 13, (9.5) | 13, (9.5) |
| Zhang,2020b[39] | ★★★★★ | China | English | 140 | 71/69 | 25-87 | 3, (2.1) | 42, (30) | — |
| Zhou,2020b[40] | ★★★★★★ | China | English | 21 | 13/8 | 66.1±13.9 | 3, (14.3) | 10, (47.6) | 0, (0) |
| Xu,2020b[41] | ★★★★★★★ | China | English | 62 | 35/27 | 41.0±15.6 | 1, (1.6) | 5, (8.1) | 21, (33.9) |
| Chen,2020e[42] | ★★★★★★ | China | English | 274 | 171/103 | 62.0±19.3 | 4, (1.5) | 93, (33.9) | 52, (19.0) |
| Zheng,2020a[43] | ★★★★★ | China | English | 96 | 58/38 | 55.0±15.2 | — | 35,(36.5) | 11, (11.5) |
| Liang,2020b[44] | ★★★★★★★ | China | English | 1590 | 904/674 | 48.9±16.3 | 30, (1.9) | 269, (16.9) | 205, (15.4) |
| Wang,2020c[45] | ★★★★★★★ | China | English | 138 | 75/63 | 56.0±19.3 | 7, (5.1) | 43, (31.2) | 21, (15.2) |
| Zheng,2020b[46] | ★★★ | China | English | 161 | 80/81 | 45±17.4 | 4, (2.5) | 22, (13.7) | 12, (7.5) |
| Wu,2020[47] | ★★★★★★ | China | English | 80 | 39/41 | 46.1±15.4 | 1, (1.3) | — | 13, (16.3) |
| Wang,2020d[48] | ★★★★ | China | English | 26 | 11/15 | 42.0±14.7 | — | 5, (19.2) | 1, (3.9) |
| Grasselli,2020[49] | ★★★★★★★★ | Italy | English | 1591 | 1304/287 | 63.0±10.4 | — | 509, (48.8) | — |
| Richardson,2020[50] | ★★★★★★★★ | America | English | 5700 | 3437/2263 | 0-107 | — | 3026, (53.1) | — |
| Wan,2020[51] | ★★★★★ | China | English | 135 | 72/63 | 47±14.1 | — | 13, (9.6) | 34, (25.2) |
| Xu,2020c[52] | ★★★★ | China | English | 90 | 39/51 | 18-86 | — | 17, (18.9) | 4, (4.4) |
| Wang,2020e[53] | ★★★★★ | China | English | 1012 | 524/488 | 16-89 | — | 46, (45.4) | 152, (15) |
| Zhang,2020c[54] | ★★★★ | China | English | 645 | 328/326 | 46.65±13.82 | — | 100, (15.5) | 67, (10.4) |
Meta-analysis findings
Primary outcome
Incidence of cerebrovascular disease as a comorbidity in patients with COVID-19
There were 18 studies [12–14, 17, 25, 27, 30, 32, 35, 36, 39–42, 44–47] reporting incidences of a history of cerebrovascular diseases among patients with COVID-19. We used a ratio difference (RD) as the effect size, and then applied generic inverse variance to calculate the pooled effect size. The pooled findings are shown in Figure 3. The heterogeneity test demonstrated moderate to significant heterogeneity among the studies (Chi2=76.06, I2=79%, P<0.00001), so the random-effects model was applied. The pooled incidence was 3.0% (95%CI=2.0%-4.0%, P<0.00001). The pooled finding indicated that 3.0% of COVID-19 patients had underlying cerebrovascular disease.
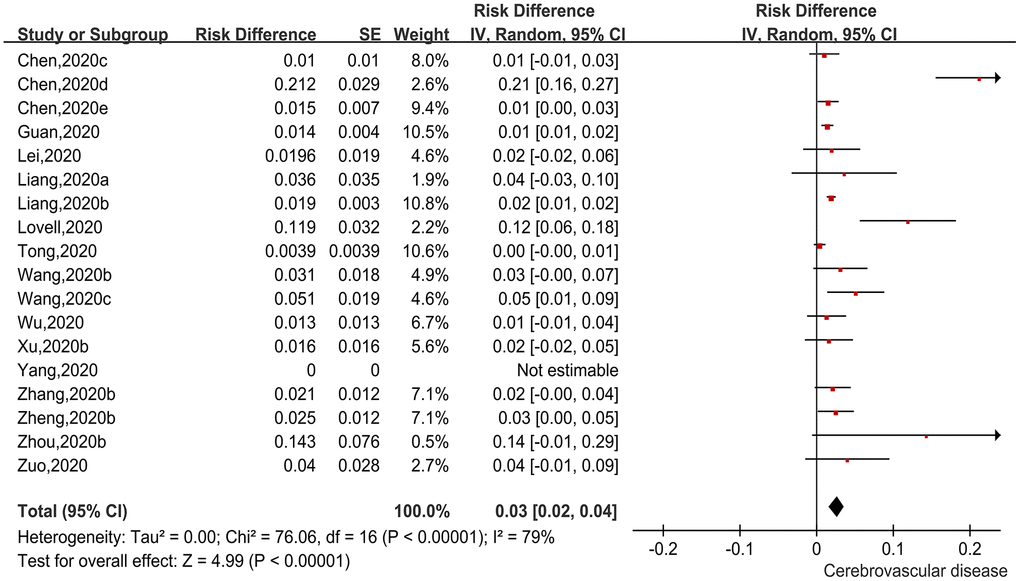
Figure 3. Forest plot showing the incidence of cerebrovascular disease as a comorbidity in patients with COVID-19.
Secondary outcomes
Incidence of hypertension as a comorbidity in patients with COVID-19
Forty one [8–18, 21–26, 29–31, 33–46, 48–54] articles presented incidences of a history of hypertension in patients with COVID-19. Using RD as the effect size, we applied generic inverse variance to calculate the pooled effect size (Figure 4). We found that there was significant heterogeneity among the studies (Chi2=3682.38, I2=99%, P<0.00001), so the random-effects model was used. The pooled incidence was 23.0% (95%CI=16.0%-29.0%, P<0.00001), suggesting 23.0% of COVID-19 patients had a history of hypertension.
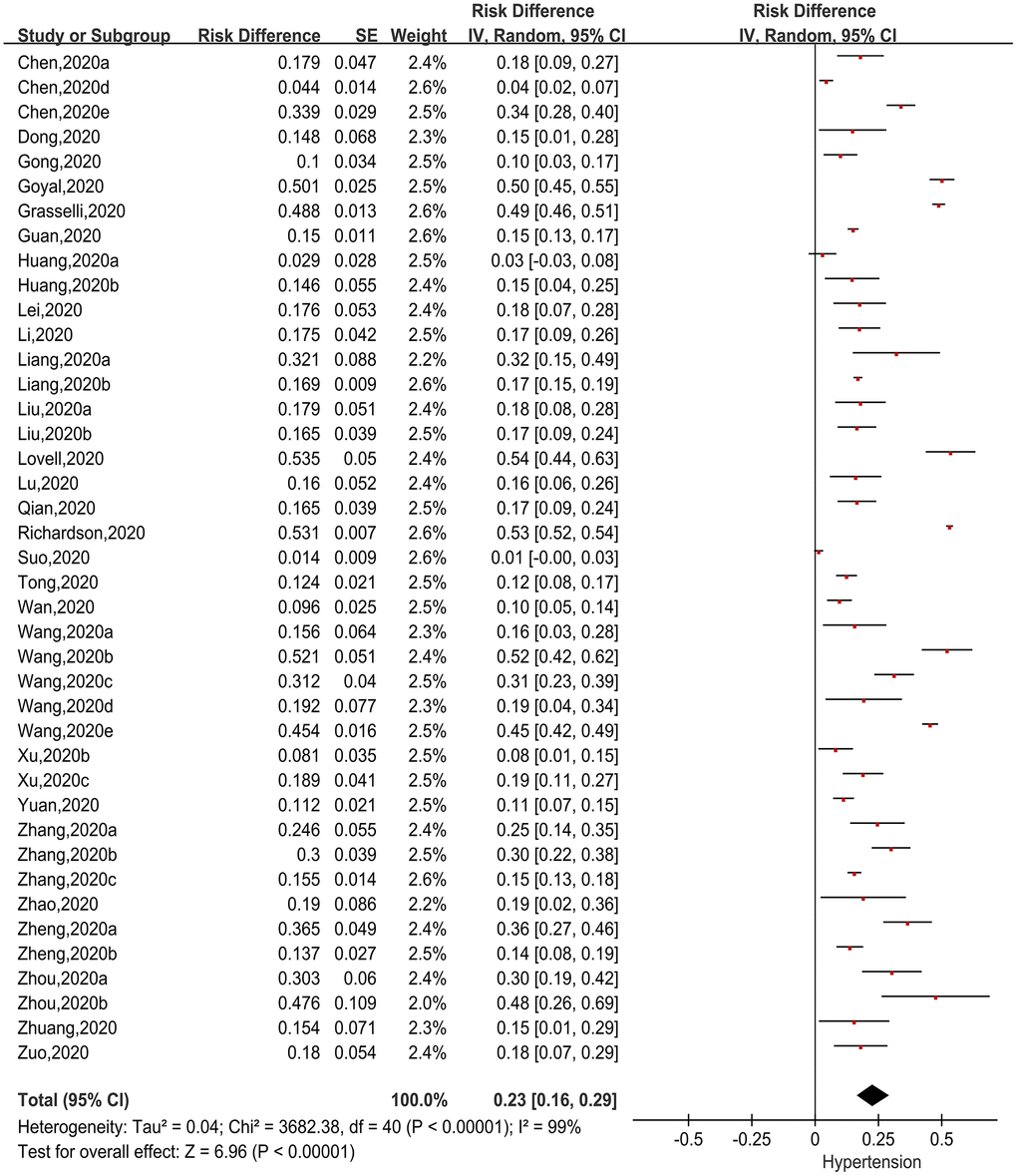
Figure 4. Forest plot showing the incidence of hypertension as a comorbidity in patients with COVID-19.
Incidence of dizziness or headache in patients with COVID-19
There were 36 papers [8–16, 18–21, 24, 26–28, 31, 32, 35–38, 40, 48, 51–54] reporting incidences of dizziness or headache (first symptom) in patients with COVID-19. Again using the RD as the effect size, generic inverse variance was applied to calculate the pooled effect size (Figure 5). The heterogeneity test indicated obvious heterogeneity among the studies (Chi2=2467.9, I2=99%, P<0.00001), so the random-effects model was applied. The pooled incidence was 14.0% (95%CI=8.0%-20.0%, P<0.00001). Thus, 14.0% of COVID-19 patients presented with dizziness or headache as their first symptom.
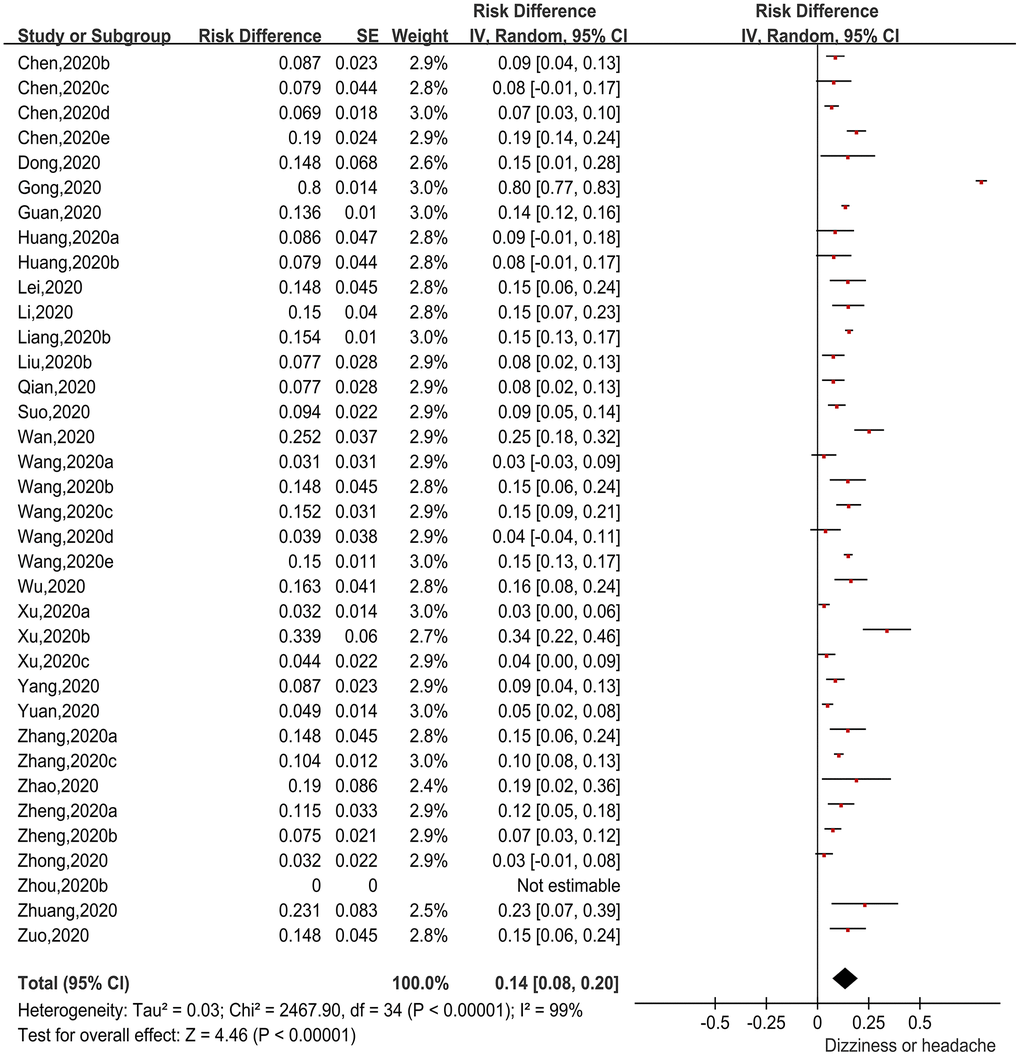
Figure 5. Forest plot showing the proportion of patients with dizziness or headache.
Subgroup analysis
Subgroup analysis was applied to investigate the potential impact on constituent ratios of cerebrovascular disease, hypertension, and dizziness or headache of country (China and other countries), sex ratio (males/females <1 and ≥1), and sample size (<100 and >100). Results of the subgroup analyses are shown in Table 2. The findings suggest that country, sex ratio, and sample size are all potential influencing factors and heterogeneity sources for the constituent ratios for cerebrovascular disease, hypertension, and dizziness or headache.
Table 2. Subgroup analysis of the impact of country, sex ratio, and sample size on the pooled findings.
| Terms | Subgroups | Number | Ratio, (%) | 95%CI | I2, (%) | P | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| CVD | Country | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| China | 17 | 0.02 | 0.01-0.03 | 77 | <0.00001 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| British | 1 | 0.12 | 0.06-0.18 | — | 0.0002 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Sex ratio (Males/Females) | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| <1 | 4 | 0.02 | 0.01-0.04 | 0 | 0.002 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| ≥1 | 14 | 0.03 | 0.02-0.04 | 84 | <0.00001 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Sample size | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| <100 | 8 | 0.02 | 0.01-0.03 | 0 | 0.003 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| >100 | 10 | 0.03 | 0.02-0.05 | 89 | <0.0001 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| HTN | Country | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| China | 37 | 0.19 | 0.15-0.23 | 96 | <0.00001 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Other countries | 4 | 0.51 | 0.48-0.54 | 67 | <0.00001 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Sex ratio (Males/Females) | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| <1 | 11 | 0.18 | 0.10-0.25 | 94 | <0.00001 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| ≥1 | 30 | 0.25 | 0.17-0.32 | 99 | <0.00001 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Sample size | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| <100 | 22 | 0.20 | 0.15-0.25 | 81 | <0.00001 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| >100 | 19 | 0.26 | 0.16-0.36 | 99 | <0.00001 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| D or H | Country | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| China | 36 | 0.14 | 0.08-0.20 | 99 | <0.00001 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Other countries | — | — | — | — | — | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Sex ratio (Males/Females) | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| <1 | 11 | 0.08 | 0.06-0.10 | 45 | <0.00001 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| ≥1 | 25 | 0.16 | 0.08-0.24 | 99 | 0.0001 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Sample size | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| <100 | 21 | 0.16 | 0.01-0.31 | 99 | 0.04 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| >100 | 15 | 0.11 | 0.09-0.14 | 89 | <0.00001 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| (CVD: cerebrovascular disease; HTN: hypertension; D or H: dizziness or headache). | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Sensitivity analysis and publication bias
We evaluated the effect of each study on the pooled constituent ratio value by sequentially removing single studies. The results revealed no obvious change in stability, which validated the rationality and reliability of our meta-analysis. The funnel plot is depicted in Figure 6. Publication bias was rated as slight to moderate based on visualization of the funnel plot. We therefore cautiously suggest that the results of this study are relatively stable and reliable.
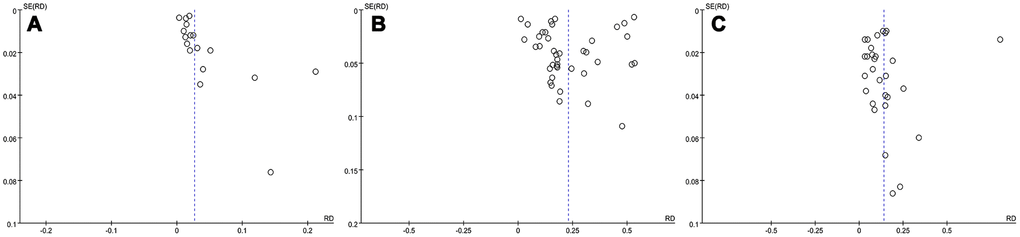
Figure 6. Funnel plot for cerebrovascular disease (A), hypertension (B), and dizziness or headache (C).
Discussion
This meta-analysis of pooling findings demonstrated that 3% of COVID-19 patients have a history of cerebrovascular disease and 23.0% have a history of hypertension. It is also worth noting that 14.0% of patients have neurological symptoms (dizziness or headache) as the first symptom of COVID-19.
A meta-analysis by Zhu et al. [55], involving 3,062 patients with COVID-19, showed that fever, fatigue, cough and expectoration are the most common clinical symptoms. Like us, however, they reported that dizziness or headache symptoms also occur (Zhu et al. 15.4% vs. the present meta-analysis: 14.0%). To effectively allocate medical resources, we need to attach great importance to early neurological symptoms (dizziness, headache, seizures etc.) in COVID-19 patients because they may not be purely related to COVID-19, but may be early signs of cerebrovascular disease. Moreover, our results indicate that about 3% COVID-19 patients had a history of cerebrovascular disease. It is therefore necessary to record early neurological symptoms and signs in COVID-19 patients. This may involve not only patient shunting and altered medical resource allocation, but also adjustment of the treatment protocol.
Angiotensin-converting enzyme 2 (ACE2) receptors are reported to be a key gateway through which viruses invade human organs or tissues [56]. This makes organs and tissues enriched in ACE2 receptors susceptible to attack by viruses. Although the lungs are ground zero, SARS-CoV-2, the virus causing COVID-19, can also infect other organs, including the brain, blood vessels, heart, testicles, kidneys, and gut [56]. When SARS-CoV-2 invades the body, its spike glycoprotein receptor-binding domain binds to ACE2 receptors, which may cause down-regulation of ACE2 expression [57]. The accompanying vasoconstriction (increased blood pressure) may become a risk factor for cerebrovascular disease. An observational study (single center and retrospective) by Li et al. [58] found that among 211 COVID-19 patients, 6% developed cerebrovascular disease.
As far as we know, the incidence of cerebrovascular disease in COVID-19 patients with underlying hypertension has not yet been reported (about 23% hypertension patients need to be closely watched). It was recently reported, however, that blood pressure variability or threshold hypertension was associated with a poor prognosis in patients with cerebrovascular disease [59]. This prompted us to ask the question, do COVID-19 patients with cerebrovascular disease comorbidity have a poorer prognosis than those without it? To answer that question, we systematically searched the PubMed database and found that a meta-analysis demonstrated that patients with a history of cerebrovascular disease have a 2.5-fold greater likelihood of severe COVID-19 illness [6]. On the other hand, the relationship between blood pressure variability and the prognosis of comorbid patients (cerebrovascular disease and COVID-19) remains unclear.
Subgroup analyses demonstrated that country (China and other countries), sex ratio (males/females <1 and ≥1), and sample size (<100 and >100) are potential influencing factors and heterogeneity sources affecting constituent ratios for cerebrovascular disease, hypertension, and dizziness or headache. It is particularly noteworthy that the constituent ratios for cerebrovascular disease and hypertension may differ among COVID-19 patients from different race groups. In addition, subgroup analysis of sex ratios suggests that men are more likely to have comorbidities (cerebrovascular disease and hypertension) and neurological symptoms (dizziness or headache). This implies that men may be more susceptible to SARS-CoV-2 infection and suggests investigation of possible detrimental effects of androgen and/or beneficial effects of estrogen may be warranted. Subgroup analysis of sample size may be less helpful in explaining the composition ratio and or rate, but it may be the source of heterogeneity between studies.
This study has several limitations. First, although 47 studies were included, the heterogeneity among studies was obvious, which may make the statistical efficiency insufficient. Second, the patients included in the analysis are mainly Chinese, which may bring challenges to the conclusions drawn. Third, several included studies did not clearly state their inclusion and exclusion criteria, disease course, or disease severity (lower quality assessment results). Fourth, due to the inclusion of data limitations, subgroup analysis was not comprehensive with regard to age, race, disease severity, and disease stage.
Conclusions
Despite the limitations of this study, which may have influenced the results, the authors conclude that cerebrovascular disease and hypertension are comorbidities among patients with COVID-19. In addition, patients reporting dizziness and headache as the first symptoms of COVID-19 should be administered neurological examinations. The difference in the degree to which men and women tolerate SARS-CoV-2 may provide a clue to the prevention and treatment of COVID-19.
Materials and Methods
This meta-analysis follows the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines [60].
Search strategy
To identify eligible studies, the main search was conducted in the PubMed, Cochrane Library, Embase, CNKI, WFSD, and VIP electronic databases for studies published between December 1, 2019 and April 26, 2020. The keywords used were 2019-nCoV/Coronavirus/COVID-19/SARS CoV-2/2019 novel coronavirus infection/coronavirus disease 2019/2019 novel coronavirus disease/coronavirus 2019/COVID-2019 and features/characteristics. Specific retrieval strategies were adjusted to accommodate the different databases. The procedure was concluded by: 1) the perusal of the reference sections of all relevant studies; 2) a manual search of key journals and abstracts from the major databases in the field of COVID-19; and 3) contacting experts to try to acquire unpublished data. The main search was completed independently by investigators. Any discrepancy was solved by consultation with an investigator not involved in the initial procedure.
Inclusion criteria
1) Participants: COVID-19 patients of all ages (diagnostic criteria comply with WHO interim guidance [61]); 2) Outcomes: incidence of a history of cerebrovascular disease and (or) hypertension in patients with COVID-19, and (or) incidence of dizziness/headache as first symptoms; 3) Study design: published case series studies and observational studies.
Exclusion criteria
1) Absence of original data; 2) sample size < 20; 3) repeated publication of a study in different languages; 4) presence of selection bias, such as only including dead patients or critically ill patients etc.
Quality assessment
Using an assessment tool, two independent reviewers assessed the quality of the selected studies according to the recommendations of the United Kingdom National Institute for Health and Care Excellence (NICE) [62]. We analyzed the following eight domains: 1) cases are preferably come from medical institutions of different levels and perform multi-center research; 2) There are clear research hypothesis or purposes; 3) There are clear inclusion and exclusion criteria; 4) There are clear outcome indicators; 5) The data collected reach the expected goal; 6) patients are recruited continuously; 7) The authors clearly describe the study’s primary findings; and 8) subgroup analysis and reporting of outcome indicators are performed. Studies are assigned one point for each criterion met, making the maximum score 8 points. Studies receiving ≥ 4 points were considered to be of high methodological quality [62]. Any disagreement was resolved through discussion by the entire review team.
Data extraction
Two reviewers extracted data independently using a predefined data extraction form. Disagreements were resolved by discussion or consensus with a third reviewer. The data extracted included the first author; study characteristics (i.e., year and publishing language); participant characteristics (i.e., age, country, sample size); and outcomes (i.e., incidence of cerebrovascular diseases or hypertension as comorbidity or dizziness/headache as the first symptom in patients with COVID-19). Cerebrovascular diseases (ischemic and hemorrhagic cerebrovascular diseases) refers to transient or permanent neurological dysfunction caused by one or more cerebrovascular diseases arising for various reasons [63]. In addition, diagnoses of hypertension complied with the Japanese Society of Hypertension Guidelines [64]. For studies with insufficient information, the reviewers contacted the primary authors, when possible, to acquire and verify the data.
Statistical analysis
Constituent ratios were pooled using the mean and standard error (SE) values and were weighted using the inverse variance method [65]. We calculated 95% confidence intervals (CIs) using the Mantel-Haenszel statistical method. I-square (I2) statistics and Q tests were performed to assess the impact of study heterogeneity on the results of the meta-analysis. According to the Cochrane review guidelines [66], if severe heterogeneity was present (P<0.1 or I2>50%), randomized effect models were chosen, otherwise fixed effect models were used. Subgroup analyses were performed based on the country, sex ratio, and sample size. To evaluate the quality and consistency of the results, a sensitivity analysis was conducted by removing individual studies. When the number of relevant studies was ≥10, the publication bias test tool included with the RevMan 5.3 software package was applied, and the funnel plot was visually inspected to assess publication bias.
Author Contributions
Jun Zhang, Haili Wang, Min Wei, and Hengzhu Zhang: gathered data, making of charts and figure, writing of the manuscript. Lun Dong, and Yuping Li: revising the manuscript, acquisition of data, accepts responsibility for conduct of research and final approval. All authors contributed to the interpretation of the data and to writing of the paper. All authors read and approved the final manuscript.
Conflicts of Interest
The authors report no conflicts of interest in this work.
Funding
This study was supported by the Jiangsu Province Key Experiments of Basic and Clinical Translation of Non-coding RNA (201902); Jiangsu Province Natural Science Foundation (BK20190241); and Jiangsu Provincial Key Medical Talents Program (QNRC2016326).
References
- 1. Zhang J, Wang H, Dong L. Letter to the editor: family member visits to critically ill patients during COVID-19: a new pathway. Telemed J E Health. 2020; 26:853–54. https://doi.org/10.1089/tmj.2020.0097 [PubMed]
- 2. World Health Organization. Corona-virus disease (COVID-19) outbreak. https://www.who.int.
- 3. Wang H, Tang X, Fan H, Luo Y, Song Y, Xu Y, Chen Y. Potential mechanisms of hemorrhagic stroke in elderly COVID-19 patients. Aging (Albany NY). 2020; 12:10022–34. https://doi.org/10.18632/aging.103335 [PubMed]
- 4. Zhang J, Wang H, Li Y, Dong L. Letter to the editor “the battle of humans and COVID-19: a war without smoke”. World Neurosurg. 2020; 139:714. https://doi.org/10.1016/j.wneu.2020.04.101 [PubMed]
- 5. World Health Organization. Coronavirus disease 2019 (COVID-19) situation report-194. https://www.who.int/.
- 6. Aggarwal G, Lippi G, Michael Henry B. Cerebrovascular disease is associated with an increased disease severity in patients with Coronavirus Disease 2019 (COVID-19): A pooled analysis of published literature. Int J Stroke. 2020; 15:385–389. https://doi.org/10.1177/1747493020921664 [PubMed]
- 7. Wang B, Li R, Lu Z, Huang Y. Does comorbidity increase the risk of patients with COVID-19: evidence from meta-analysis. Aging (Albany NY). 2020; 12:6049–57. https://doi.org/10.18632/aging.103000 [PubMed]
- 8. Li D, Long YZ, Huang P, Guo WL, Wu SH, Zhou Q, Fu JL. [Clinical characteristics of 80 patients with COVID-19 in Zhuzhou City]. Chin J Infect Control. 2020; 19:227–233. https://doi.org/10.12138/j.issn.1671-9638.20206514
- 9. Yuan Q, Sun YY, Zuo YJ, Chen TY, Cao Q, Yuan GD, Yang M, Zhang W, Peng AZ, Chen YK. [Analysis 223 patients with COVID-19 of clinical characteristics in Chongqing]. J of Southwest Univ (Natural Science). 2020; 42:17–24. https://doi.org/10.13718/j.cnki.xdzk.2020.03.003
- 10. Wang K, Kang SR, Tian RH, Wang Y, Zhang XZ, Li HM. [CT characteristic appearances of patients with novel coronavirus pneumonia]. Chinese Journal of Clinical Medicine. 2020; 27:27–31. https://doi.org/10.12025/j.issn.1008-6358.2020.20200169
- 11. Zhang YM, Zhang X, Wu D, Chen X, Zhang L, Zhang DW. [Clinical characteristics of COVID-19 and related nursing care]. Acad J Chin PLA Med Sch. 2020; 41:212–216. http://kns.cnki.net/kcms/detail/10.1117.r.20200421.1845.011.html.
- 12. Zuo FT, Li LC, Dong ZG, Chang XH, Jia MY, Wei CM, Zheng XS. [Analysis of thecorrelation between clinical characteristics and disease severity in patients with novel coronavirus pneumonia]. Tianjin Med J. 2020; 48:455–460. http://kns.cnki.net/kcms/detail/12.1116.r.20200413.1014.006.html.
- 13. Wang R, Xie LL, Du P, Fan HQ, Song MY. [Clinical characteristics of 96 hospitalized patients with coronavirus disease 2019]. Chinese Journal of Respiratory and Critical Care Medicine. 2020; 19:144–147. https://doi.org/10.7507/1671-6205.202002066
- 14. Lei Y, Lu J, Gu JY, Zhou DF, Li YY, Lu QF. [Clinical features of 51 patients with corona virus disease 2019 in Wuhan City]. Journal of Shandong University (Health Sciences). 2020; 58:1–6. http://kns.cnki.net/kcms/detail/37.1390.R.20200414.1315.006.html.
- 15. Dong L, Yang SJ, Zhang LS, Zhang ZH, Wang RQ, Xu K, Liu JL. [A preliminary study on clinical characteristics and pathological characteristics of 27 cases of COVID-19 patients in Sichuan]. Pharmacology and Clinics of Chinese Materia Medica. 2020; 2:50–53. https://doi.org/10.13412/j.cnki.zyyl.20200420.002.
- 16. Zhao L, Xue J, Wang YL, Dai EH, Xu ZG, Li YN, Dun ZQ, Gao HX, Rong YY, Chen C. [The clinical feature and imaging analysis of patients with new coronavirus infection in Shijiazhuang]. Tianjin Med J. 2020; 48:513–517. http://kns.cnki.net/kcms/detail/12.1116.r.20200417.1147.002.html.
- 17. Tong GD, Xia Z, Wang YX, Chen S, Wu ZM, Zeng ZY, Deng X. [The clinical features of 258 cases of new coronavirus pneumonia in Shenzhen City]. Journal of Traditional Chinese Medicine. 2020. [Epub ahead of print]. http://kns.cnki.net/kcms/detail/11.2166.R.20200413.1552.006.html.
- 18. Suo T, Wang YN, Zhao KC, Chen GZ. Clinical characteristics and outcome analysis of COVID-19 patients with chronic underlying diseases. Medical Journal of Wuhan University. 2020. [Epub ahead of print]. https://doi.org/10.14188/j.1671-8852.2020.0233.
- 19. Zhong SH, Lin F, Shi L. [The clinical characteristics and outcome of 62 patients with COVID-19]. Medical Journal of Chinese People’s Liberation Army. 2020. [Epub ahead of print]. http://kns.cnki.net/kcms/detail/11.1056.R.20200326.1308.002.html.
- 20. Xu J, Han MF, Zhao FD, Zhang T, Ma L. [Clinical manifestation sandsero-immunological characteristics of 155 patients with COVID-19]. Chin J Nosocomio. 2020; 30:961–965. https://doi.org/10.11816/cn.ni.2020-200577
- 21. Gong XY, Wei DR, Gong X, Xiong Y, Wang T, Mou FZ. [Analysis on TCM Clinical Characteristics and Syndromes of 80 Patients with Novel Coronavirus Pneumonia]. Chinese Journal of Information on TCM. 2020; 27:1–6. http://kns.cnki.net/kcms/detail/11.3519.r.20200330.1553.002.html.
- 22. Chen L, Yang XP, Zhen NH, Cai T, Hu YR, Gu JN, Zhao WH. [Clinical characteristics of 67 discharged cases of Corona Virus Disease 2019]. Chin J Nosocomiol. 2020; 30:801–805. https://doi.org/10.11816/cn.ni.2020-200526
- 23. Lu YF, Yang ZG, Wang M, Shi J, Wang ZW, Lv Y, Tang BZ, Ye C, Xu QN, Yin KS, Chen XR. [Analysis on Chinese medical clinical characteristics of 50 patients with novel coronavirus-infected pneumonia]. Academic Journal of Shanghai University of Traditional Chinese Medicine. 2020; 34:17–21. https://doi.org/10.16306/j.1008-861x.2020.02.003
- 24. Huang XQ, Nie LH, Li FM, Wang C, Chen G, Cai KK, Yu CY, Li C. [Analysis of Chinese Medical Characteristics of 35 Patients with Novel Coronavirus Pneumonia]. JETCM. 2020; 29:381–383. https://doi.org/10.3969/j.issn.1004-745X.2020.03.002
- 25. Liang YL, Yue F, Song L. [Epidemiological and Clinical Characteristics of 28 Confirmed Cases of Novel Coronavirus Pneumonia]. Clinical Research. 2020; 28:1–3. http://www.wanfangdata.com.cn/details/detail.do?_type=perio&id=yyybj202004001.
- 26. Zhuang YJ, Chen Z, Li J, Yang XL, Li J, Yuan Y, Guan Q, Jia HJ, Ma QY, Wu D, Ma HB, Tang ZR. [Clinical and epidemiological characteristics of 26 patients diagnosed with COVID-19]. Chin J Nosocomiol. 2020; 30:826–829. https://doi.org/10.11816/cn.ni.2020-200207
- 27. Yang W, Cao Q, Qin L, Wang X, Cheng Z, Pan A, Dai J, Sun Q, Zhao F, Qu J, Yan F. Clinical characteristics and imaging manifestations of the 2019 novel coronavirus disease (COVID-19):A multi-center study in Wenzhou city, Zhejiang, China. J Infect. 2020; 80:388–93. https://doi.org/10.1016/j.jinf.2020.02.016 [PubMed]
- 28. Chen J, Qi T, Liu L, Ling Y, Qian Z, Li T, Li F, Xu Q, Zhang Y, Xu S, Song Z, Zeng Y, Shen Y, et al. Clinical progression of patients with COVID-19 in Shanghai, China. J Infect. 2020; 80:e1–e6. https://doi.org/10.1016/j.jinf.2020.03.004 [PubMed]
- 29. Liu K, Chen Y, Lin R, Han K. Clinical features of COVID-19 in elderly patients: a comparison with young and middle-aged patients. J Infect. 2020; 80:e14–18. https://doi.org/10.1016/j.jinf.2020.03.005 [PubMed]
- 30. Lovell N, Maddocks M, Etkind SN, Taylor K, Carey I, Vora V, Marsh L, Higginson IJ, Prentice W, Edmonds P, Sleeman KE. Characteristics, symptom management, and outcomes of 101 patients with COVID-19 referred for hospital palliative care. J Pain Symptom Manage. 2020; 60:e77–81. https://doi.org/10.1016/j.jpainsymman.2020.04.015 [PubMed]
- 31. Huang C, Wang Y, Li X, Ren L, Zhao J, Hu Y, Zhang L, Fan G, Xu J, Gu X, Cheng Z, Yu T, Xia J, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet. 2020; 395:497–506. https://doi.org/10.1016/S0140-6736(20)30183-5 [PubMed]
- 32. Chen N, Zhou M, Dong X, Qu J, Gong F, Han Y, Qiu Y, Wang J, Liu Y, Wei Y, Xia J, Yu T, Zhang X, Zhang L. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. Lancet. 2020; 395:507–13. https://doi.org/10.1016/S0140-6736(20)30211-7 [PubMed]
- 33. Zhou F, Yu T, Du R, Fan G, Liu Y, Liu Z, Xiang J, Wang Y, Song B, Gu X, Guan L, Wei Y, Li H, et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet. 2020; 395:1054–1062. https://doi.org/10.1016/S0140-6736(20)30566-3 [PubMed]
- 34. Goyal P, Choi JJ, Pinheiro LC, Schenck EJ, Chen R, Jabri A, Satlin MJ, Campion TR
Jr , Nahid M, Ringel JB, Hoffman KL, Alshak MN, Li HA, et al. Clinical characteristics of covid-19 in New York city. N Engl J Med. 2020; 382:2372–74. https://doi.org/10.1056/NEJMc2010419 [PubMed] - 35. Guan WJ, Ni ZY, Hu Y, Liang WH, Ou CQ, He JX, Liu L, Shan H, Lei CL, Hui DS, Du B, Li LJ, Zeng G, et al, and China Medical Treatment Expert Group for Covid-19. Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med. 2020; 382:1708–20. https://doi.org/10.1056/NEJMoa2002032 [PubMed]
- 36. Chen T, Dai Z, Mo P, Li X, Ma Z, Song S, Chen X, Luo M, Liang K, Gao S, Zhang Y, Deng L, Xiong Y. Clinical characteristics and outcomes of older patients with coronavirus disease 2019 (COVID-19) in Wuhan, China: a single-centered, retrospective study. J Gerontol A Biol Sci Med Sci. 2020; 75:1788–95. https://doi.org/10.1093/gerona/glaa089 [PubMed]
- 37. Qian GQ, Yang NB, Ding F, Ma AH, Wang ZY, Shen YF, Shi CW, Lian X, Chu JG, Chen L, Wang ZY, Ren DW, Li GX, et al. Epidemiologic and clinical characteristics of 91 hospitalized patients with COVID-19 in Zhejiang, China: a retrospective, multi-centre case series. QJM. 2020; 113:474–81. https://doi.org/10.1093/qjmed/hcaa089 [PubMed]
- 38. Liu K, Fang YY, Deng Y, Liu W, Wang MF, Ma JP, Xiao W, Wang YN, Zhong MH, Li CH, Li GC, Liu HG. Clinical characteristics of novel coronavirus cases in tertiary hospitals in Hubei Province. Chin Med J (Engl). 2020; 133:1025–31. https://doi.org/10.1097/CM9.0000000000000744 [PubMed]
- 39. Zhang JJ, Dong X, Cao YY, Yuan YD, Yang YB, Yan YQ, Akdis CA, Gao YD. Clinical characteristics of 140 patients infected with SARS-CoV-2 in Wuhan, China. Allergy. 2020; 75:1730–41. https://doi.org/10.1111/all.14238 [PubMed]
- 40. Zhou Y, Han T, Chen J, Hou C, Hua L, He S, Guo Y, Zhang S, Wang Y, Yuan J, Zhao C, Zhang J, Jia Q, et al. Clinical and autoimmune characteristics of severe and critical cases of COVID-19. Clin Transl Sci. 2020; 10:1111. https://doi.org/10.1111/cts.12805 [PubMed]
- 41. Xu XW, Wu XX, Jiang XG, Xu KJ, Ying LJ, Ma CL, Li SB, Wang HY, Zhang S, Gao HN, Sheng JF, Cai HL, Qiu YQ, Li LJ. Clinical findings in a group of patients infected with the 2019 novel coronavirus (SARS-cov-2) outside of Wuhan, China: retrospective case series. BMJ. 2020; 368:m606. https://doi.org/10.1136/bmj.m606 [PubMed]
- 42. Chen T, Wu D, Chen H, Yan W, Yang D, Chen G, Ma K, Xu D, Yu H, Wang H, Wang T, Guo W, Chen J, et al. Clinical characteristics of 113 deceased patients with coronavirus disease 2019: retrospective study. BMJ. 2020; 368:m1091. https://doi.org/10.1136/bmj.m1091 [PubMed]
- 43. Zheng S, Fan J, Yu F, Feng B, Lou B, Zou Q, Xie G, Lin S, Wang R, Yang X, Chen W, Wang Q, Zhang D, et al. Viral load dynamics and disease severity in patients infected with SARS-CoV-2 in Zhejiang Province, China, January-March 2020: retrospective cohort study. BMJ. 2020; 369:m1443. https://doi.org/10.1136/bmj.m1443 [PubMed]
- 44. Liang WH, Guan WJ, Li CC, Li YM, Liang HR, Zhao Y, Liu XQ, Sang L, Chen RC, Tang CL, Wang T, Wang W, He QH, et al. Clinical characteristics and outcomes of hospitalised patients with COVID-19 treated in Hubei (epicentre) and outside Hubei (non-epicentre): a nationwide analysis of China. Eur Respir J. 2020; 55:2000562. https://doi.org/10.1183/13993003.00562-2020 [PubMed]
- 45. Wang D, Hu B, Hu C, Zhu F, Liu X, Zhang J, Wang B, Xiang H, Cheng Z, Xiong Y, Zhao Y, Li Y, Wang X, Peng Z. Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China. JAMA. 2020; 323:1061–69. https://doi.org/10.1001/jama.2020.1585 [PubMed]
- 46. Zheng F, Tang W, Li H, Huang YX, Xie YL, Zhou ZG. Clinical characteristics of 161 cases of corona virus disease 2019 (COVID-19) in Changsha. Eur Rev Med Pharmacol Sci. 2020; 24:3404–10. https://doi.org/10.26355/eurrev_202003_20711 [PubMed]
- 47. Wu J, Liu J, Zhao X, Liu C, Wang W, Wang D, Xu W, Zhang C, Yu J, Jiang B, Cao H, Li L. Clinical characteristics of imported cases of coronavirus disease 2019 (COVID-19) in Jiangsu Province: a multicenter descriptive study. Clin Infect Dis. 2020; 71:706–12. https://doi.org/10.1093/cid/ciaa199 [PubMed]
- 48. Wang L, Duan Y, Zhang W, Liang J, Xu J, Zhang Y, Wu C, Xu Y, Li H. Epidemiologic and clinical characteristics of 26 cases of COVID-19 arising from patient-to-patient transmission in Liaocheng, China. Clin Epidemiol. 2020; 12:387–91. https://doi.org/10.2147/CLEP.S249903 [PubMed]
- 49. Grasselli G, Zangrillo A, Zanella A, Antonelli M, Cabrini L, Castelli A, Cereda D, Coluccello A, Foti G, Fumagalli R, Iotti G, Latronico N, Lorini L, et al, and COVID-19 Lombardy ICU Network. Baseline characteristics and outcomes of 1591 patients infected with SARS-CoV-2 admitted to ICUs of the Lombardy region, Italy. JAMA. 2020; 323:1574–81. https://doi.org/10.1001/jama.2020.5394 [PubMed]
- 50. Richardson S, Hirsch JS, Narasimhan M, Crawford JM, McGinn T, Davidson KW, Barnaby DP, Becker LB, Chelico JD, Cohen SL, Cookingham J, Coppa K, Diefenbach MA, et al, and the Northwell COVID-19 Research Consortium. Presenting characteristics, comorbidities, and outcomes among 5700 patients hospitalized with COVID-19 in the New York city area. JAMA. 2020; 323:2052–59. https://doi.org/10.1001/jama.2020.6775 [PubMed]
- 51. Wan S, Xiang Y, Fang W, Zheng Y, Li B, Hu Y, Lang C, Huang D, Sun Q, Xiong Y, Huang X, Lv J, Luo Y, et al. Clinical features and treatment of COVID-19 patients in northeast Chongqing. J Med Virol. 2020; 92:797–806. https://doi.org/10.1002/jmv.25783 [PubMed]
- 52. Xu X, Yu C, Qu J, Zhang L, Jiang S, Huang D, Chen B, Zhang Z, Guan W, Ling Z, Jiang R, Hu T, Ding Y, et al. Imaging and clinical features of patients with 2019 novel coronavirus SARS-CoV-2. Eur J Nucl Med Mol Imaging. 2020; 47:1275–80. https://doi.org/10.1007/s00259-020-04735-9 [PubMed]
- 53. Wang X, Fang J, Zhu Y, Chen L, Ding F, Zhou R, Ge L, Wang F, Chen Q, Zhang Y, Zhao Q. Clinical characteristics of non-critically ill patients with novel coronavirus infection (COVID-19) in a Fangcang Hospital. Clin Microbiol Infect. 2020; 26:1063–68. https://doi.org/10.1016/j.cmi.2020.03.032 [PubMed]
- 54. Zhang X, Cai H, Hu J, Lian J, Gu J, Zhang S, Ye C, Lu Y, Jin C, Yu G, Jia H, Zhang Y, Sheng J, et al. Epidemiological, clinical characteristics of cases of SARS-CoV-2 infection with abnormal imaging findings. Int J Infect Dis. 2020; 94:81–87. https://doi.org/10.1016/j.ijid.2020.03.040 [PubMed]
- 55. Zhu J, Ji P, Pang J, Zhong Z, Li H, He C, Zhang J, Zhao C. Clinical characteristics of 3062 COVID-19 patients: a meta-analysis. J Med Virol. 2020; 10:1002. https://doi.org/10.1002/jmv.25884 [PubMed]
- 56. Meredith W, Jennifer CF, Jocelyn K, Catherine M. How does coronavirus kill? Clinicians trace a ferocious rampage through the body, from brain to toes. Science. 2020. https://doi.org/10.1126/science.abc3208
- 57. Lambert DW, Clarke NE, Turner AJ. Not just angiotensinases: new roles for the angiotensin-converting enzymes. Cell Mol Life Sci. 2010; 67:89–98. https://doi.org/10.1007/s00018-009-0152-x [PubMed]
- 58. Li Y, Li M, Wang M, Zhou Y, Chang J, Xian Y, Wang D, Mao L, Jin H, Hu B. Acute cerebrovascular disease following COVID-19: a single center, retrospective, observational study. Stroke Vasc Neurol. 2020. [Epub ahead of print]. https://doi.org/10.1136/svn-2020-000431 [PubMed]
- 59. Divani AA, Liu X, Di Napoli M, Lattanzi S, Ziai W, James ML, Jafarli A, Jafari M, Saver JL, Hemphill JC, Vespa PM, Mayer SA, Petersen A. Blood Pressure Variability Predicts Poor In-Hospital Outcome in Spontaneous Intracerebral Hemorrhage. Stroke. 2019; 50:2023–2029. https://doi.org/10.1161/STROKEAHA.119.025514 [PubMed]
- 60. Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JP, Clarke M, Devereaux PJ, Kleijnen J, Moher D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. J Clin Epidemiol. 2009; 62:e1–34. https://doi.org/10.1016/j.jclinepi.2009.06.006 [PubMed]
- 61. World Health Organization. Clinical management of severe acute respiratory infection when novel coronavirus (2019-nCoV) infection is suspected: interim guidance. 2020. https://apps.who.int/iris/bitstream/handle/10665/330374/WHO-2019-nCoV-laboratory-2020.1-eng.pdf.
- 62. NICE. Appendix 4 Quality of case series form [EB/OL] (2015-07-08) [2020-04-29]. http://www.nice.org.uk/guidance/index.
- 63. Chen Y, Hu FY, Wu B. Interpretation of "Chinese classification of cerebrovascular diseases (2015)". Chin J Contemp Neurol Neurosurg. 2017; 17:865–868. https://doi.org/10.3969/j.issn.1672-6731.2017.12.002
- 64. Umemura S, Arima H, Arima S, Asayama K, Dohi Y, Hirooka Y, Horio T, Hoshide S, Ikeda S, Ishimitsu T, Ito M, Ito S, Iwashima Y, et al. The Japanese society of hypertension guidelines for the management of hypertension (JSH 2019). Hypertens Res. 2019; 42:1235–481. https://doi.org/10.1038/s41440-019-0284-9 [PubMed]
- 65. Zhou XH, Obuchowski NA, McClish DK. Statistical methods in diagnostic medicine. New York. Wiley; 2002. https://doi.org/10.1002/9780470317082
- 66. Higgins JPT, Green S. Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 [updated March 2011]. The Cochrane Collaboration 2011. http://training.cochrane.org/handbook.


