Introduction
Aging can be characterized by the progressive loss of physiological integrity, resulting in impaired functions and susceptibility for diseases and death. This biological deterioration is considered a major risk factor for cancer, cardiovascular diseases, diabetes and Alzheimer’s disease among others. At the cellular level, there are two key hallmarks of the aging process: shortening of telomere length and cellular senescence [1].
Telomeres are tandem nucleotide repeats located at the end of the chromosomes which maintain genomic stability. Telomeres shorten during replication (mitosis) due to the inherent inability to fully replicate the end part of the lagging DNA strand [2]. Telomere length (TL), measuring between 4 to 15 kilobases, gradually shorten by ~20-40 bases per year and is associated with different diseases, low physical performance and cortical thinning of the brain [3–5]. When TL reaches a critical length, cells cannot replicate and progress to senescence or programmed cell death [6]. Goglin et al. demonstrated that adults with shorter TLs have increased mortality rates [7]. Shortened TLs can be a direct inherited trait, but several environmental factors have also been associated with shortening TL including stress, lack of physical endurance activity, excess body mass index, smoking, chronic inflammation, vitamins deficiency and oxidative stress [2, 8, 9].
Cellular senescence is an arrest of the cell cycle which can be caused by telomere shortening [10], as well as other aging associated stimuli independent of TL such as non-telomeric DNA damage [1]. The primary purpose of senescence is to prevent propagation of damaged cells by triggering their elimination via the immune system. The accumulation of senescent cells with aging reflects either an increase in the generation of these cells and/or a decrease in their clearance, which in turn aggravates the damage and contributes to aging [1].
A growing body of research has found several pharmacological agents that can reduce the telomere shortening rate [11, 12]. Several lifestyle interventions including endurance training, diets and supplements targeting cell metabolism and oxidative stress have reported relatively small effects (2-5%) on TL3, [2, 8, 9].
Hyperbaric oxygen therapy (HBOT) utilizes 100% oxygen in an environmental pressure higher than one absolute atmospheres (ATA) to enhance the amount of oxygen dissolved in body’s tissues. Repeated intermittent hyperoxic exposures, using certain HBOT protocols, can induce physiological effects which normally occur during hypoxia in a hyperoxic environment, the so called hyperoxic-hypoxic paradox [13–16]. In addition, it was recently demonstrated that HBOT can induce cognitive enhancements in healthy aging adults via mechanisms involving regional changes in cerebral blood flow [17]. On the cellular level, it was demonstrated that HBOT can induce the expression of hypoxia induced factor (HIF), vascular endothelial growth factor (VEGF) and sirtuin (SIRT), stem cell proliferation, mitochondrial biogenesis, angiogenesis and neurogenesis [18]. However, no study to date has examined HBOT’s effects on TL and senescent cell accumulation.
The aim of the current study was to evaluate whether HBOT affects TL and senescence-like T-cells population in aging adults.
Results
Thirty-five individuals were assigned to HBOT. Five patients did not complete baseline assessments and were excluded. All 30 patients who completed baseline evaluations completed the interventions. Due to the low quality of blood samples (low number of cells or technician error), four patients were excluded from the telomere analysis and 10 patients from senescent cell analysis (Figure 1). The baseline characteristics and comparison of the cohorts following exclusion of the patients are provided in Table 1. There were no significant differences between the three groups (Table 1).
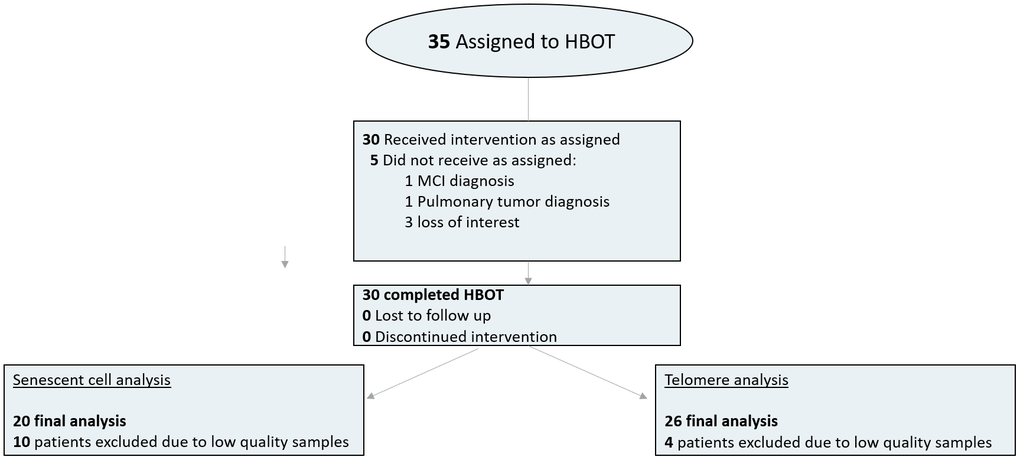
Figure 1. Patient flowchart.
Table 1. Baseline characteristics.
| HBOT | Telomere analysis | Senescent analysis | P-value | ||
| N | 30 | 25 (83.3%) | 20 (66.6%) | ||
| Age (years) | 68.41±13.2 | 67.56±14.35 | 66.70±16.00 | 0.917 | |
| BMI | 26.77±3.20 | 26.89±3.34 | 27.14±3.81 | 0.946 | |
| Males | 16 (53.3%) | 13 (52.0%) | 10 (50.0%) | 0.987 | |
| Females | 14 (47.7%) | 12 (48.0%) | 10 (50.0%) | 0.987 | |
| Complete blood count | |||||
| Hemoglobin | 6.33±1.25 | 6.57±1.15 | 6.58±1.29 | 0.707 | |
| White blood cells | 14.02±1.40 | 13.92±1.35 | 13.97±1.49 | 0.969 | |
| %PBMC | 39.96±6.75 | 39.25±6.64 | 38.59±6.63 | 0.774 | |
| Platelets | 239.87±1.39 | 244.08±43.0 | 254.05±41.4 | 0.559 | |
| Chronic medical conditions | |||||
| Atrial fibrillation | 4 (13.3%) | 4 (16.0%) | 2 (10.0%) | 0.841 | |
| Hypothyroidism | 4 (13.3%) | 4 (16.0%) | 3 (15.8%) | 0.956 | |
| Obstructive sleep apnea | 4 (13.3%) | 4 (16.0%) | 3 (15.0%) | 0.961 | |
| Asthma | 1 (3.3%) | 1 (4.0%) | 0 | 0.680 | |
| BPH | 7 (23.3%) | 5 (20.0%) | 6 (30.0%) | 0.733 | |
| GERD | 3 (10%) | 2 (8.0%) | 2 (10.0%) | 0.961 | |
| Osteoporosis | 5 (16.7%) | 5 (20.0%) | 4 (20.0%) | 0.936 | |
| Rheumatic arthritis | 1 (3.3%) | 0 | 1 (5.0%) | 0.561 | |
| Osteoarthritis | 7 (23.3%) | 4 (16.0%) | 5 (25.0%) | 0.755 | |
| Diabetes mellitus | 3 (10%) | 3 (12.0%) | 2 (10.0%) | 0.966 | |
| Hypertension | 7 (23.3%) | 5 (20.0%) | 5 (25.0%) | 0.918 | |
| Dyslipidemia | 16 (53.3%) | 14 (56.0%) | 12 (60.0%) | 0.897 | |
| Ischemic heart disease | 2 (6.7%) | 1 (4.0%) | 2 (10.0%) | 0.725 | |
| History of smoking | 10 (33.3%) | 8 (32.0%) | 7 (35.0%) | 0.978 | |
| Chronic medications | |||||
| Anti-aggregation | 8 (26.7%) | 6 (24.0%) | 5 (25.0%) | 0.974 | |
| ACE-Inhibitors/ARB blockers | 6 (20%) | 6 (24.0%) | 6 (30.0%) | 0.720 | |
| Beta blockers | 5 (16.7%) | 5 (20.0%) | 3 (15.0%) | 0.901 | |
| Calcium blockers | 3 (10%) | 3 (12.0%) | 2 (10.0%) | 0.966 | |
| Alpha blockers | 7 (23.3%) | 5 (20.0%) | 6 (30.0%) | 0.733 | |
| Diuretics | 2 (6.7%) | 1 (4.0%) | 1 (5.0%) | 0.906 | |
| Statins | 10 (33.3%) | 9 (36.0%) | 7 (35.0%) | 0.978 | |
| Oral hypoglycemic | 1 (3.3%) | 1 (4.0%) | 1 (5.0%) | 0.958 | |
| Bisphosphonates | 1 (3.3%) | 1 (4.0%) | 1 (5.0%) | 0.958 | |
| Proton pump inhibitors | 3 (10%) | 3 (12.0%) | 3 (15.0%) | 0.726 | |
| Hormones | 3 (10%) | 3 (12.0%) | 2 (10.0%) | 0.966 | |
| Benzodiazepines | 3 (10%) | 2 (8.0%) | 1 (5.0%) | 0.816 | |
| SSRI | 5 (16.7%) | 5 (20.0%) | 3 (15.0%) | 0.990 |
Telomere length
Compared to the baseline, the T-helper telomere lengths were significantly increased at the 30th session and post-HBOT by 21.70±40.05 (p=0.042), 23.69%±39.54 (p=0.012) and 29.30±38.51 (p=0.005), respectively (Figure 2). However, repeated measures analysis shows a non-significant trend (F=4.663, p=0.06, Table 2 and Figure 2).
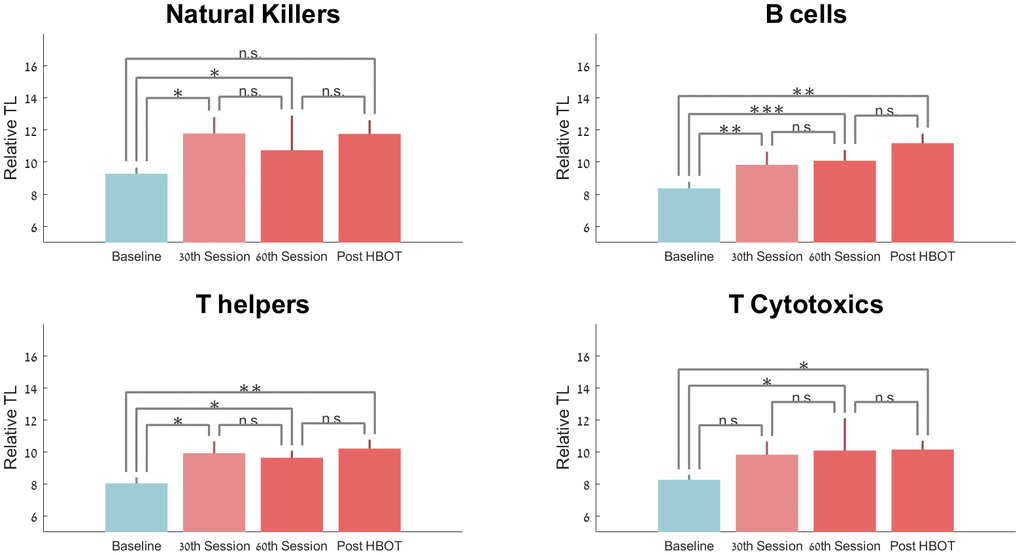
Figure 2. Telomere length changes with HBOT. Mean+SEM *p<0.05, **p<0.01, ***p<0.001.
Table 2. Telomere length and senescent cell changes post-HBOT.
| Absolute changes | Relative changes (%) | Repeated measures F (p) | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| PBMC | Baseline | 30th Session | 60th Session | Post HBOT | 30th session | 60th session | Post-HBOT | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| PBMC ((N=25) | 2.55±0.53 | -0.15±0.40 | -4.91±16.70 | 1.987 (t) 0.09 | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| PBMC (N=20) | 2.50±0.53 | -0.13±0.31 | -4.21±11.99 | 1.810 (t) 0.07 | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Relative telomeres length (N=25) | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Natural killer | 9.27±1.91 | 11.77±5.14 (0.045) | 10.73±2.73 (0.013) | 11.75±4.22 (0.06) | 25.02±51.42 | 20.56±33.35 | 22.16±44.81 | 0.812 (0.391) | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| B-cells | 8.36±2.02 | 10.22±3.04 (0.007) | 11.23±3.58 (0.0001) | 11.17±2.98 (0.007) | 25.68±40.42 | 29.39±23.39 | 37.63±52.73 | 7.390 (0.017) | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| T Helper | 8.04±1.82 | 9.92±3.68 (0.042) | 9.63±2.17 (0.012) | 10.20±2.77 (0.005) | 21.70±40.05 | 23.69±39.54 | 29.30±38.51 | 4.663 (0.063) | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| T Cytotoxic | 8.26±1.54 | 9.83±4.08 (0.11) | 10.08±3.33 (0.019) | 10.15±2.74 (0.023) | 18.29±45.62 | 24.13±40.88 | 19.59±33.98 | 1.159 (0.310) | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Senescent cells (% of T cells) (N=20) | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| T Helper | 10.29±5.42 | 7.84±7.09 (0.09) | 8.51±7.45 (0.20) | 6.22±4.88 (<0.0001) | -19.66±80.03 | -11.67±94.30 | -37.30±33.04 | 8.548 (0.01) | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| T Cytotoxic | 52.19±21.07 | 45.53±19.91 (<0.0001) | 45.45±18.81 (0.002) | 46.59±21.91 (0.0004) | -12.21±8.74 | -9.81±9.50 | -10.96±12.59 | 6.916 (0.018) | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| P-values shown in () compared to baseline. | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| P-values in bold <0.05. | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Compared to baseline, telomere lengths of B cells increased significantly at the 30th session, 60th session and post-HBOT by 25.68%±40.42 (p=0.007), 29.39%±23.39 (p=0.0001) and 37.63%±52.73 (p=0.007), respectively (Figure 2). Repeated measures analysis shows a significant within-group effect (F=0.390, p=0.017, Table 2 and Figure 2).
Compared to baseline, natural killer cells telomer lengths significantly increased at the 30th session (p=0.045) and at the 60th session by 20.56% ±33.35 (p=0.013). Post-HBOT, telomere lengths increased by 22.16%±44.81 post-HBOT (p=0.06, Table 2 and Figure 2). Repeated measures analysis indicates that there was no additional significant effect after the 30th session (F=0.812, p=0.391).
Compared to baseline, cytotoxic T-cells had a non-significant increase at the 30th session by 18.29%±45.62 (p=0.11), followed by a significant increase of 24.13%±40.88 at the 60th session (p=0.0019) and 19.59%±33.98 post-HBOT (p=0.023). Repeated measures analysis indicates that there was no additional significant effect after the 30th session (F=1.159, p=0.310, Table 2 and Figure 2).
Senescent cells
There was a non-significant decrease in the number of senescent T-helpers at the 30th session and 60th session by -19.66%±80.03 (p=0.09) and -11.67%±94.30 (p=0.20) respectively. However, there was a significant drop in the number of senescent T helpers by -37.30%±33.04 post-HBOT (P<0.0001, Figure 3). Repeated measures analysis showed a significant continuous effect even after the 30th session, with a within-group effect (F=8.547, p=0.01, Table 2 and Figure 3).
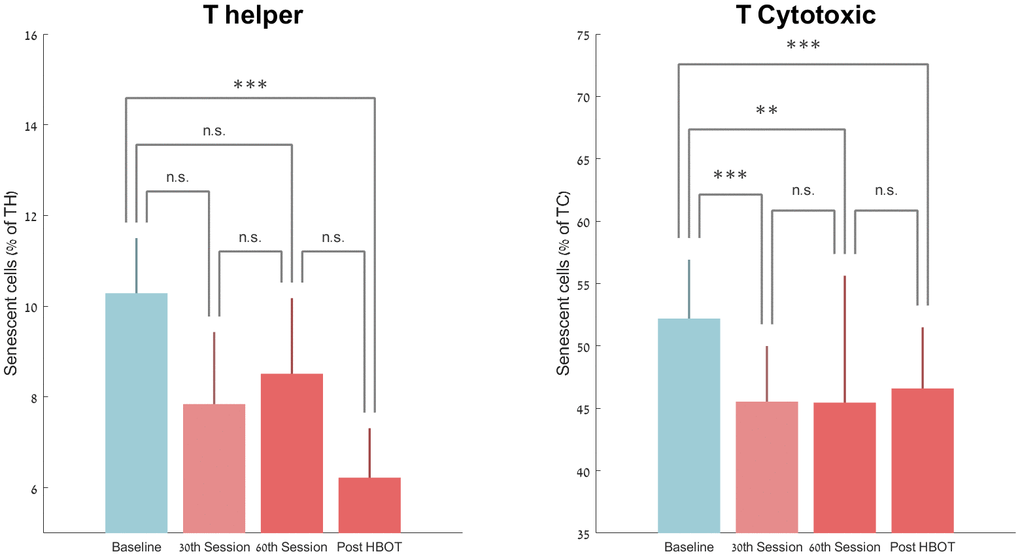
Figure 3. Senescent cell changes with HBOT. Mean+SEM *p<0.05, **p<0.01, ***p<0.001.
T-cytotoxic senescent cell percentages decreased significantly by -12.21%±8.74 (P<0.0001) at the 30th HBOT session, -9.81%±9.50 at the 60th HBOT session (0.002) and -10.96%±12.59 (p=0.0004) post-HBOT (Table 2 and Figure 3). Repeated measures analysis shows a significant continuous effect even after the 30th session, with a within-group effect (F=6.916, p=0.018, Table 2).
HIF-1alpha
HIF-1alpha levels were increased from 10.54±3.39 to 19.71±3.39 at the 60th session (p=0.006) where 2 weeks post HBOT levels of 16.81±7.65 were not significantly different from baseline (p=0.16).
Discussion
In this study, for the first time in humans, it was found that repeated daily HBOT sessions can increase PBMC telomere length by more than 20% in an aging population, with B cells having the most striking change. In addition, HBOT decreased the number of senescent cells by 10-37%, with T helper senescent cells being the most effected.
A substantial number of associations between telomere length and lifestyle modifications have been observed. This has led to several interventional studies which included diet, supplements (such as omega-3, and walnuts among others), physical activity, stress management and social support. A two year trial conducted on cognitively healthy elderly adults, using a diet rich in walnuts, showed a non-significant trend to preserve telomere length when compared to a control diet [19]. In another study which evaluated the effect of a twelve week low frequency explosive-type resistance training in elderly people, telomere length was better preserved in the intervention group without a significant increase [20]. A recent study found that aerobic endurance training or high intensity interval training for six month increased telomere length up to 5% [21]. Additional weight loss, yoga and stress management techniques failed to show significant telomere length changes [22–25]. However, most of these studies have shown significant correlations between antioxidant activity and telomerase activity [22–25].
While many genetic and environmental factors are associated with telomere shortening, the most common suggest mechanism is oxidative stress. Oxidative stress can occur from imbalances between the production of reactive oxygen species (ROS) and cellular scavengers. Telomeres are highly sensitive to oxidative DNA damage, which can induce telomere shortening and dysfunction [26]. The association between oxygen and/or oxidative stress and telomere length has been debated for the past several decades. Human cell culture studies consistently show that mild oxidative stress accelerates telomere shortening, whereas antioxidants and free radical scavengers decrease shortening rates and increase the cellular proliferative lifespan [27]. Several clinical studies on pathological conditions (such as diabetes, inflammatory diseases, Parkinson’s disease) have shown correlations between oxidative stress markers, reactive oxygen species scavengers levels and telomere length [28]. However, healthy individuals did not show similar results [29].
Exposing cell cultures to a hyperbaric environment has been previously suggested to induce significant oxidative stress and premature cells senescence [30]. However, this was based on isolated cells grown in a hyperbaric incubator and not on the complex biological system of humans as in this study. Similar to the current study, a previous prospective one-year observational study in divers exposed to intense hyperbaric oxygen, showed significant telomere elongation in leukocytes [31]. As used in the current study, the HBOT protocol utilizes the effects induced by repeated intermittent hyperoxic exposures, the so called hyperoxic hypoxic paradox [13, 18]. These intermittent hyperoxic exposures induce an adaptive response which includes increased upregulation of antioxidants genes [32] and production of antioxidants/scavengers that adjust to the increased ROS generation causing the ROS/scavenger ratio to gradually becomes similar to the ratio under a normal oxygen environment. However, because the scavenger elimination half-life (T1/2) is significantly longer than the T1/2 of ROS, upon return to normoxia, following repeated hyperoxic exposures, there are significantly higher levels of scavengers and increased antioxidant activity [13, 18]. Thus, similar to physical exercise and caloric restriction, a daily repeated HBOT protocol can induce the hormesis phenomenon. Single exposures increase ROS generation acutely, triggering the antioxidant response, and with repeated exposures, the response becomes protective [13, 18].
Additionally, intermittent hyperoxic exposures induce many of the physiological responses that occur during hypoxia [13]. HBOT induces the release of transcription factors called hypoxic induced factors (HIF) and increase their stability and activity [14]. In turn, HIF induces a cellular cascade including vascular endothelial growth factor and angiogenesis induction, mitochondria biogenesis, stem cells mobilization and SIRT1 increased activity [18]. Our study confirms increased HIF expression is induced by repetitive HBOT exposures, which gradually decreases towards normalization of HIF levels at nonmonic environment.
Currently, many interventions that genetically or pharmacologically (senolytic drugs) remove senescent cells have been developed in animal models and are waiting for safety and efficacy evaluations in humans [33]. The current study suggests a non-pharmacological method, clinically available with well-established safety profile, for senescent cells populations decrease. Our protocol included 60 sessions of 100% oxygen at 2 ATA including three air breaks during each session to utilize the hyperoxic hypoxic paradox and minimize the risk of oxygen toxicity. Interestingly, both TL and senescent cell reduction peaked at the 30th session. However, the dose response curve related to the applied pressure, time and number of HBOT exposures and its relation to HIF expression and its related regenerative effects are still not fully understood and further studies are needed to find the optimal HBOT protocols.
Hyperbaric oxygen therapy is a well-established treatment modality for non-healing wounds, radiation injuries as well as different hypoxic or ischemic events (such as carbon monoxide toxicity, infections, etc). In recent years, a growing evidence from pre-clinical as well as clinical trials demonstrate the efficacy of HBOT for neurological indications including idiopathic sudden sensorineural hearing loss [34], post stroke and post traumatic brain injury [35–41], central sensitization syndrome such as fibromyalgia syndrome [42, 43] and age related cognitive decline [17] and animal models of Alzheimer’s disease [44]. For the first time, the current study aimed to evaluate the physiological effect on the cellular level in aging humans without any functional limiting disease.
Study limitations
The current study has several limitations and strengths to consider. First, the limited sample size has to be taken into account. Second, the lack of control group. However, the study suggests impressive results on TL and senescent cell clearance, which weren't observed in other interventions. Moreover, the baseline telomere length values of our cohort match the expected values for the aging population [45–47]. Third, the duration of the effect has yet to be determined in long-term follow-ups. Fourth, telomerase activity was not evaluated due to the method chosen for blood preservation and evaluation. Nevertheless, several strengths should be stressed. In this study, CD28 was used as a biomarker for senescent cells whereas CD57 was not available as a confirmatory marker for T cell senescence. Biomarkers were assessed on specific leukocytes populations rather than using the entire PBMCs as one group. The isolated HBOT effect was measured and participants were monitored for not making any lifestyle changes (such as nutrition and exercise), medications or any other intervention that may have acted as possible confounders.
In summary, the study indicates that HBOT can induce significant senolytic effects, including significant increased telomere length and clearance of senescent cells in aging populations.
Materials and Methods
Subjects
Thirty-five adults without pathological cognitive declines, aged 64 and older, who lived independently in good functional and cognitive status, were enrolled. The study was performed between 2016-2020 in the Shamir (Assaf-Harofeh) Medical Center, Israel. Included patients did not have cardiac or cerebrovascular ischemia histories for the last year prior to inclusion. Exclusion criteria included: previous treatment with HBOT for any reason during the last three months, any history of malignancy during the last year, any pathological cognitive decline, severe chronic renal failure (GFR <30), uncontrolled diabetes mellitus (HbA1C>8, fasting glucose>200), immunosuppressants, MRI contraindications (including BMI>35), active smoking or pulmonary diseases.
Study design
The study protocol was approved by Institutional Review Board of the Shamir Medical Center, Israel. The study was performed as a prospective clinical trial. After signing an informed consent and undergoing a baseline evaluation, the subjects were assigned to HBOT. Measurement points were evaluated at baseline, half-point of the treatment protocol (30th session), the day of the last HBOT session and 1-2 weeks after the HBOT.
The study cohort included only patients treated by HBOT, which is part of a larger cohort of normal ageing population studied at the Shamir medical center, Israel (NCT02790541 [17]).
Interventions
The HBOT protocol was administrated in a Multiplace Starmed-2700 chamber (HAUX, Germany). The protocol comprised of 60 daily sessions, five sessions per week within a three-month period. Each session included breathing 100% oxygen by mask at 2ATA for 90 minutes with 5-minute air breaks every 20 minutes. Compression/decompression rates were 1 meter/minute. During the trial, neither lifestyle and diet changes, nor medications adjustments were allowed.
Blood samples
Whole blood samples were collected into EDTA tubes using a standard technique, at baseline, at the half-point of the HBOT protocol (30th session), the day of the last HBOT session (60th session) and 1-2 weeks following the last HBOT session.
Peripheral blood mononuclear cells (PBMCs) isolation
Whole blood was diluted using phosphate buffered saline (PBS). Density gradient separation was performed using Leucosep tubes filled with Lymphoprep. The tubes were then centrifuged at 1000×g for 10 min at 25° C degrees. Following centrifugation, the cell layers (buffy coat) were immediately collected via pipette and transferred to 50 mL conical centrifuge tubes, resuspended with sufficient 1X PBS to a volume of 50 mL and centrifuged at 300×g for 10 min at 25° C degrees. Following removal of the supernatant, each sample was labeled.
Telomere length
Telomeres were labelled according to the Dako PNA/FITC kit protocol (Code K5327). On a single cell suspension consisting of a mixture of PBMCs (sample cells) and TCL 1301 cell line (control cells), the DNA was denatured for 10 minutes at 82° C in a microcentrifuge tube either in the presence of hybridization solution without probe or in hybridization solution containing the fluorescein-conjugated PNA telomere probe. The hybridization took place in the dark at room temperature (RT) overnight. The hybridization was followed by two 10-minute post-hybridization washes with a wash solution at 40° C. The sample was then labeled with CD4+, CD8+, CD3+, CD19+ and CD56+ conjugated antibodies in an appropriate buffer for further flow cytometric analysis [48, 49]. Each sample was run in duplicate. Following flow cytometric analysis, the relative telomere length (RTL) was calculated for CD3+/CD4+ (T-helper), CD3+/CD8+ (T-cytotoxic), CD3+/CD56+ (natural killer) and CD19+ (B-cells). The RTL value was calculated as the ratio between the telomere signal of each sample and the control cell (TCL 1301 cell line) with correction for the DNA index of G0/1 cells. Sample cells and control cells were analyzed separately for DNA ploidy using propidium iodide staining to standardize the number of telomere ends per cell and thereby telomere length per chromosome. See Figure 4 for FACS analysis example.
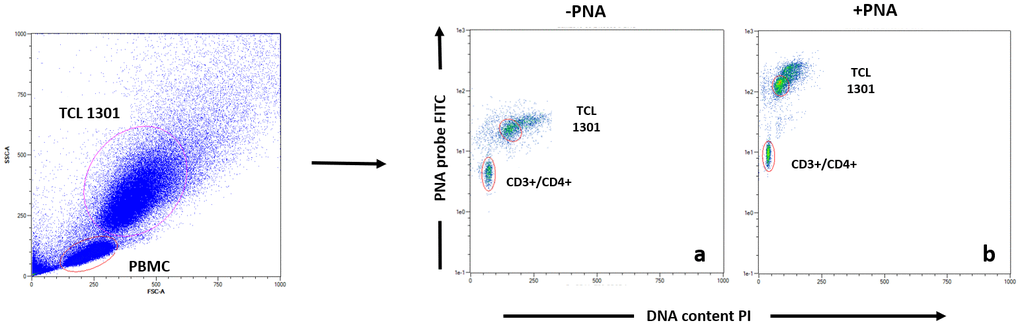
Figure 4. Example of Flow Fish data analysis of T helper subpopulation. Each blood sample was either stained with PNA probe (b) or without (a), following by antibodies staining (CD3, CD4, CD8, CD16, CD19), before data acquisition.
Immunophenotyping
Percentages of CD3+CD4+CD28-null T cells (senescent T helpers) and CD3+CD8+CD28-null T cells (senescent T cytotoxics) were determined by flow-cytometric analysis. PBMC were stained with VioBlue conjugated anti-CD3, Viogreen conjugated anti-CD8, PE-VIO 770A conjugated anti-CD4 and APC-VIO 770A anti-CD28 antibodies (Miltenyi Biotec). Cells were analyzed with a MACSQuant Flow Cytometer (Miltenyi Biotec). The percentage of CD28null T cells within the CD4+ or CD8+ T cell population was then calculated.
Hypoxia induced factor (HIF-1alpha)
Intracellular HIF1a staining was performed with APC conjugated anti-HIF1a antibody or corresponding Isotype Control (R&D systems) following fixation and permeabilization (Life Technologies). Cells were analyzed with a MACSQuant Flow Cytometer (Miltenyi Biotec) and the percentage of HIF1a expressing PBMCs, was determined.
Statistical analysis
Unless otherwise specified, continuous data were expressed as means ± standard-deviation. The normal distribution for all variables was tested using the Kolmogorov-Smirnov test. One-way ANOVA was performed to compare variables between and within the three groups at baseline.
Categorical data is expressed in numbers and percentages and compared by chi-square tests. Univariate analyses were performed using Chi-Square/Fisher’s exact test to identify significant variables (P<0.05).
To evaluate HBOT’s effects, a repeated measures ANOVA model was used to test the main within-subject effect. Post hoc tests on the means was conducted to test for time differences using t tests with a Bonferroni correction.
Author Contributions
All authors contributed substantially to the preparation of this manuscript. HY, HA, ES were responsible for protocol design. HA, ZY, BY, ES, DKM were responsible for patients' recruitment. YH, AHR, SM, YY, SM, ZR, ESW, HA, DKM, SG, BGR, DG, HY, AHR, FG, LE, PN, DK, FM, ZY, BY were responsible for data acquisition. HY, HA. and ES were responsible for data analysis. All authors interpreted the data. HY, HA, CM, and ES wrote the manuscript. All authors revised and finalized the manuscript.
Acknowledgments
We would like to thank Dr. Mechael Kanovsky for his editing of this manuscript.
Conflicts of Interest
AH, BY, ZY work for AVIV Scientific LTD. ES is a shareholder at AVIV Scientific LTD.
Funding
The study was funded by a research grant from the Sagol network for neuroscience established by Mr. Sami Sagol.
References
- 1. López-Otín C, Blasco MA, Partridge L, Serrano M, Kroemer G. The hallmarks of aging. Cell. 2013; 153:1194–217.a https://doi.org/10.1016/j.cell.2013.05.039 [PubMed]
- 2. Tsoukalas D, Fragkiadaki P, Docea AO, Alegakis AK, Sarandi E, Vakonaki E, Salataj E, Kouvidi E, Nikitovic D, Kovatsi L, Spandidos DA, Tsatsakis A, Calina D. Association of nutraceutical supplements with longer telomere length. Int J Mol Med. 2019; 44:218–26. https://doi.org/10.3892/ijmm.2019.4191 [PubMed]
- 3. Starkweather AR, Alhaeeri AA, Montpetit A, Brumelle J, Filler K, Montpetit M, Mohanraj L, Lyon DE, Jackson-Cook CK. An integrative review of factors associated with telomere length and implications for biobehavioral research. Nurs Res. 2014; 63:36–50. https://doi.org/10.1097/NNR.0000000000000009 [PubMed]
- 4. Puhlmann LM, Valk SL, Engert V, Bernhardt BC, Lin J, Epel ES, Vrticka P, Singer T. Association of short-term change in leukocyte telomere length with cortical thickness and outcomes of mental training among healthy adults: a randomized clinical trial. JAMA Netw Open. 2019; 2:e199687. https://doi.org/10.1001/jamanetworkopen.2019.9687 [PubMed]
- 5. Åström MJ, von Bonsdorff MB, Perälä MM, Salonen MK, Rantanen T, Kajantie E, Simonen M, Pohjolainen P, Haapanen MJ, Guzzardi MA, Iozzo P, Kautiainen H, Eriksson JG. Telomere length and physical performance among older people-the helsinki birth cohort study. Mech Ageing Dev. 2019; 183:111145. https://doi.org/10.1016/j.mad.2019.111145 [PubMed]
- 6. Xie Z, Jay KA, Smith DL, Zhang Y, Liu Z, Zheng J, Tian R, Li H, Blackburn EH. Early telomerase inactivation accelerates aging independently of telomere length. Cell. 2015; 160:928–39. https://doi.org/10.1016/j.cell.2015.02.002 [PubMed]
- 7. Goglin SE, Farzaneh-Far R, Epel ES, Lin J, Blackburn EH, Whooley MA. Change in leukocyte telomere length predicts mortality in patients with stable coronary heart disease from the heart and soul study. PLoS One. 2016; 11:e0160748. https://doi.org/10.1371/journal.pone.0160748 [PubMed]
- 8. Armanios M. Telomeres and age-related disease: how telomere biology informs clinical paradigms. J Clin Invest. 2013; 123:996–1002. https://doi.org/10.1172/JCI66370 [PubMed]
- 9. Richards JB, Valdes AM, Gardner JP, Paximadas D, Kimura M, Nessa A, Lu X, Surdulescu GL, Swaminathan R, Spector TD, Aviv A. Higher serum vitamin D concentrations are associated with longer leukocyte telomere length in women. Am J Clin Nutr. 2007; 86:1420–25. https://doi.org/10.1093/ajcn/86.5.1420 [PubMed]
- 10. Bodnar AG, Ouellette M, Frolkis M, Holt SE, Chiu CP, Morin GB, Harley CB, Shay JW, Lichtsteiner S, Wright WE. Extension of life-span by introduction of telomerase into normal human cells. Science. 1998; 279:349–52. https://doi.org/10.1126/science.279.5349.349 [PubMed]
- 11. Townsley DM, Dumitriu B, Liu D, Biancotto A, Weinstein B, Chen C, Hardy N, Mihalek AD, Lingala S, Kim YJ, Yao J, Jones E, Gochuico BR, et al. Danazol treatment for telomere diseases. N Engl J Med. 2016; 374:1922–31. https://doi.org/10.1056/NEJMoa1515319 [PubMed]
- 12. Coutts F, Palmos AB, Duarte RR, de Jong S, Lewis CM, Dima D, Powell TR. The polygenic nature of telomere length and the anti-ageing properties of lithium. Neuropsychopharmacology. 2019; 44:757–65. https://doi.org/10.1038/s41386-018-0289-0 [PubMed]
- 13. Cimino F, Balestra C, Germonpré P, De Bels D, Tillmans F, Saija A, Speciale A, Virgili F. Pulsed high oxygen induces a hypoxic-like response in human umbilical endothelial cells and in humans. J Appl Physiol (1985). 2012; 113:1684–89. https://doi.org/10.1152/japplphysiol.00922.2012 [PubMed]
- 14. Sunkari VG, Lind F, Botusan IR, Kashif A, Liu ZJ, Ylä-Herttuala S, Brismar K, Velazquez O, Catrina SB. Hyperbaric oxygen therapy activates hypoxia-inducible factor 1 (HIF-1), which contributes to improved wound healing in diabetic mice. Wound Repair Regen. 2015; 23:98–103. https://doi.org/10.1111/wrr.12253 [PubMed]
- 15. Milovanova TN, Bhopale VM, Sorokina EM, Moore JS, Hunt TK, Hauer-Jensen M, Velazquez OC, Thom SR. Hyperbaric oxygen stimulates vasculogenic stem cell growth and differentiation in vivo. J Appl Physiol (1985). 2009; 106:711–28. https://doi.org/10.1152/japplphysiol.91054.2008 [PubMed]
- 16. Yang Y, Wei H, Zhou X, Zhang F, Wang C. Hyperbaric oxygen promotes neural stem cell proliferation by activating vascular endothelial growth factor/extracellular signal-regulated kinase signaling after traumatic brain injury. Neuroreport. 2017; 28:1232–38. https://doi.org/10.1097/WNR.0000000000000901 [PubMed]
- 17. Hadanny A, Daniel-Kotovsky M, Suzin G, Boussi-Gross R, Catalogna M, Dagan K, Hachmo Y, Abu Hamed R, Sasson E, Fishlev G, Lang E, Polak N, Doenyas K, et al. Cognitive enhancement of healthy older adults using hyperbaric oxygen: a randomized controlled trial. Aging (Albany NY). 2020; 12:13740–61. https://doi.org/10.18632/aging.103571 [PubMed]
- 18. Hadanny A, Efrati S. The hyperoxic-hypoxic paradox. Biomolecules. 2020; 10:958. https://doi.org/10.3390/biom10060958 [PubMed]
- 19. Freitas-Simoes TM, Cofán M, Blasco MA, Soberón N, Foronda M, Serra-Mir M, Roth I, Valls-Pedret C, Doménech M, Ponferrada-Ariza E, Calvo C, Rajaram S, Sabaté J, et al. Walnut consumption for two years and leukocyte telomere attrition in mediterranean elders: results of a randomized controlled trial. Nutrients. 2018; 10:1907. https://doi.org/10.3390/nu10121907 [PubMed]
- 20. Dimauro I, Scalabrin M, Fantini C, Grazioli E, Beltran Valls MR, Mercatelli N, Parisi A, Sabatini S, Di Luigi L, Caporossi D. Resistance training and redox homeostasis: correlation with age-associated genomic changes. Redox Biol. 2016; 10:34–44. https://doi.org/10.1016/j.redox.2016.09.008 [PubMed]
- 21. Werner CM, Hecksteden A, Morsch A, Zundler J, Wegmann M, Kratzsch J, Thiery J, Hohl M, Bittenbring JT, Neumann F, Böhm M, Meyer T, Laufs U. Differential effects of endurance, interval, and resistance training on telomerase activity and telomere length in a randomized, controlled study. Eur Heart J. 2019; 40:34–46. https://doi.org/10.1093/eurheartj/ehy585 [PubMed]
- 22. Sanft T, Usiskin I, Harrigan M, Cartmel B, Lu L, Li FY, Zhou Y, Chagpar A, Ferrucci LM, Pusztai L, Irwin ML. Randomized controlled trial of weight loss versus usual care on telomere length in women with breast cancer: the lifestyle, exercise, and nutrition (LEAN) study. Breast Cancer Res Treat. 2018; 172:105–12. https://doi.org/10.1007/s10549-018-4895-7 [PubMed]
- 23. Mason C, Risques RA, Xiao L, Duggan CR, Imayama I, Campbell KL, Kong A, Foster-Schubert KE, Wang CY, Alfano CM, Blackburn GL, Rabinovitch PS, McTiernan A. Independent and combined effects of dietary weight loss and exercise on leukocyte telomere length in postmenopausal women. Obesity (Silver Spring). 2013; 21:E549–54. https://doi.org/10.1002/oby.20509 [PubMed]
- 24. Krishna BH, Keerthi GS, Kumar CK, Reddy NM. Association of leukocyte telomere length with oxidative stress in yoga practitioners. J Clin Diagn Res. 2015; 9:CC01–03. https://doi.org/10.7860/JCDR/2015/13076.5729 [PubMed]
- 25. Tehfe M, Dowden S, Kennecke H, El-Maraghi R, Lesperance B, Couture F, Letourneau R, Liu H, Romano A. Erratum to: nab-paclitaxel plus gemcitabine versus gemcitabine in patients with metastatic pancreatic adenocarcinoma: canadian subgroup analysis of the phase 3 MPACT trial. Adv Ther. 2017; 34:277–79. https://doi.org/10.1007/s12325-016-0442-2 [PubMed]
- 26. Barnes RP, Fouquerel E, Opresko PL. The impact of oxidative DNA damage and stress on telomere homeostasis. Mech Ageing Dev. 2019; 177:37–45. https://doi.org/10.1016/j.mad.2018.03.013 [PubMed]
- 27. von Zglinicki T. Oxidative stress shortens telomeres. Trends Biochem Sci. 2002; 27:339–44. https://doi.org/10.1016/s0968-0004(02)02110-2 [PubMed]
- 28. Sampson MJ, Winterbone MS, Hughes JC, Dozio N, Hughes DA. Monocyte telomere shortening and oxidative DNA damage in type 2 diabetes. Diabetes Care. 2006; 29:283–89. https://doi.org/10.2337/diacare.29.02.06.dc05-1715 [PubMed]
- 29. Reichert S, Stier A. Does oxidative stress shorten telomeres in vivo? a review. Biol Lett. 2017; 13:20170463. https://doi.org/10.1098/rsbl.2017.0463 [PubMed]
- 30. Oh S, Lee E, Lee J, Lim Y, Kim J, Woo S. Comparison of the effects of 40% oxygen and two atmospheric absolute air pressure conditions on stress-induced premature senescence of normal human diploid fibroblasts. Cell Stress Chaperones. 2008; 13:447–58. https://doi.org/10.1007/s12192-008-0041-5 [PubMed]
- 31. Shlush LI, Skorecki KL, Itzkovitz S, Yehezkel S, Segev Y, Shachar H, Berkovitz R, Adir Y, Vulto I, Lansdorp PM, Selig S. Telomere elongation followed by telomere length reduction, in leukocytes from divers exposed to intense oxidative stress—implications for tissue and organismal aging. Mech Ageing Dev. 2011; 132:123–30. https://doi.org/10.1016/j.mad.2011.01.005 [PubMed]
- 32. Godman CA, Joshi R, Giardina C, Perdrizet G, Hightower LE. Hyperbaric oxygen treatment induces antioxidant gene expression. Ann N Y Acad Sci. 2010; 1197:178–83. https://doi.org/10.1111/j.1749-6632.2009.05393.x [PubMed]
- 33. Pignolo RJ, Passos JF, Khosla S, Tchkonia T, Kirkland JL. Reducing senescent cell burden in aging and disease. Trends Mol Med. 2020; 26:630–38. https://doi.org/10.1016/j.molmed.2020.03.005 [PubMed]
- 34. LE W. Hyperbaric Oxygen Therapy Indications. UHMS. 2008; 12th edition:215–218.
- 35. Boussi-Gross R, Golan H, Fishlev G, Bechor Y, Volkov O, Bergan J, Friedman M, Hoofien D, Shlamkovitch N, Ben-Jacob E, Efrati S. Hyperbaric oxygen therapy can improve post concussion syndrome years after mild traumatic brain injury - randomized prospective trial. PLoS One. 2013; 8:e79995. https://doi.org/10.1371/journal.pone.0079995 [PubMed]
- 36. Efrati S, Fishlev G, Bechor Y, Volkov O, Bergan J, Kliakhandler K, Kamiager I, Gal N, Friedman M, Ben-Jacob E, Golan H. Hyperbaric oxygen induces late neuroplasticity in post stroke patients—randomized, prospective trial. PLoS One. 2013; 8:e53716. https://doi.org/10.1371/journal.pone.0053716 [PubMed]
- 37. Mukherjee A, Raison M, Sahni T, Arya A, Lambert J, Marois P, James PB, Parent A, Ballaz L. Intensive rehabilitation combined with HBO2 therapy in children with cerebral palsy: a controlled longitudinal study. Undersea Hyperb Med. 2014; 41:77–85. [PubMed]
- 38. Hadanny A, Golan H, Fishlev G, Bechor Y, Volkov O, Suzin G, Ben-Jacob E, Efrati S. Hyperbaric oxygen can induce neuroplasticity and improve cognitive functions of patients suffering from anoxic brain damage. Restor Neurol Neurosci. 2015; 33:471–86. https://doi.org/10.3233/RNN-150517 [PubMed]
- 39. Tal S, Hadanny A, Berkovitz N, Sasson E, Ben-Jacob E, Efrati S. Hyperbaric oxygen may induce angiogenesis in patients suffering from prolonged post-concussion syndrome due to traumatic brain injury. Restor Neurol Neurosci. 2015; 33:943–51. https://doi.org/10.3233/RNN-150585 [PubMed]
- 40. Hadanny A, Rittblat M, Bitterman M, May-Raz I, Suzin G, Boussi-Gross R, Zemel Y, Bechor Y, Catalogna M, Efrati S. Hyperbaric oxygen therapy improves neurocognitive functions of post-stroke patients - a retrospective analysis. Restor Neurol Neurosci. 2020; 38:93–107. https://doi.org/10.3233/RNN-190959 [PubMed]
- 41. Tal S, Hadanny A, Sasson E, Suzin G, Efrati S. Hyperbaric oxygen therapy can induce angiogenesis and regeneration of nerve fibers in traumatic brain injury patients. Front Hum Neurosci. 2017; 11:508. https://doi.org/10.3389/fnhum.2017.00508 [PubMed]
- 42. Efrati S, Golan H, Bechor Y, Faran Y, Daphna-Tekoah S, Sekler G, Fishlev G, Ablin JN, Bergan J, Volkov O, Friedman M, Ben-Jacob E, Buskila D. Hyperbaric oxygen therapy can diminish fibromyalgia syndrome—prospective clinical trial. PLoS One. 2015; 10:e0127012. https://doi.org/10.1371/journal.pone.0127012 [PubMed]
- 43. Hadanny A, Bechor Y, Catalogna M, Daphna-Tekoah S, Sigal T, Cohenpour M, Lev-Wiesel R, Efrati S. Hyperbaric oxygen therapy can induce neuroplasticity and significant clinical improvement in patients suffering from fibromyalgia with a history of childhood sexual abuse-randomized controlled trial. Front Psychol. 2018; 9:2495. https://doi.org/10.3389/fpsyg.2018.02495 [PubMed]
- 44. Shapira R, Efrati S, Ashery U. Hyperbaric oxygen therapy as a new treatment approach for Alzheimer’s disease. Neural Regen Res. 2018; 13:817–18. https://doi.org/10.4103/1673-5374.232475 [PubMed]
- 45. Steenstrup T, Kark JD, Verhulst S, Thinggaard M, Hjelmborg JV, Dalgård C, Kyvik KO, Christiansen L, Mangino M, Spector TD, Petersen I, Kimura M, Benetos A, et al. Telomeres and the natural lifespan limit in humans. Aging (Albany NY). 2017; 9:1130–42. https://doi.org/10.18632/aging.101216 [PubMed]
- 46. Shammas MA. Telomeres, lifestyle, cancer, and aging. Curr Opin Clin Nutr Metab Care. 2011; 14:28–34. https://doi.org/10.1097/MCO.0b013e32834121b1 [PubMed]
- 47. Teubel I, Elchinova E, Roura S, Fernández MA, Gálvez-Montón C, Moliner P, de Antonio M, Lupón J, Bayés-Genís A. Telomere attrition in heart failure: a flow-FISH longitudinal analysis of circulating monocytes. J Transl Med. 2018; 16:35. https://doi.org/10.1186/s12967-018-1412-z [PubMed]
- 48. Baerlocher GM, Lansdorp PM. Telomere length measurements in leukocyte subsets by automated multicolor flow-FISH. Cytometry A. 2003; 55:1–6. https://doi.org/10.1002/cyto.a.10064 [PubMed]
- 49. Baerlocher GM, Lansdorp PM. Telomere length measurements using fluorescence in situ hybridization and flow cytometry. Methods Cell Biol. 2004; 75:719–50. https://doi.org/10.1016/s0091-679x(04)75031-1 [PubMed]


