Features selection and morphology-based radiomics signature construction
The comparison of traditional morphological and radiomics features between ruptured and unruptured aneurysms is summarized in Table 1. The eleven traditional morphological features in the derivation cohort with p < 0.20 that were analyzed using multivariable logistic regression included: size, neck, height, width, AR, SR, irregular shape, neck, branching to parent ratio (BPR), neck to parent ratio (NPR), and bifurcation.
Ten radiomics morphological features were identified as potential indicators, including surface volume ratio, spherical disproportion, maximum 3D diameter, maximum 2D diameter slice, major axis length, least axis length, maximum 2D diameter column, maximum 2D diameter row, elongation, and flatness. These ten features had coefficients > 0 in the least absolute shrinkage and selection operator (LASSO) logistic regression model and were included in the radiomics signature score (rad-score) calculation formula (Figure 4).
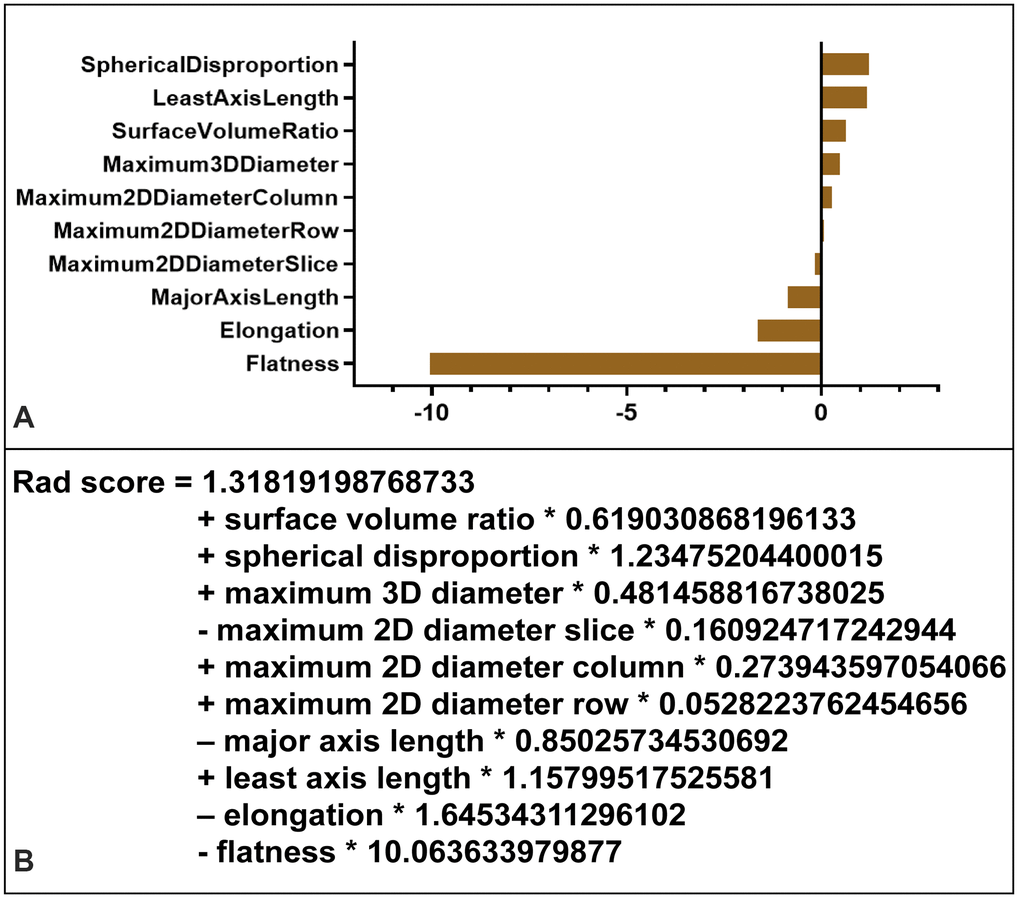
Figure 4. Radiomics signature score (rad-score) calculation. (A) Radiomic features ranked by coefficients of the least absolute shrinkage and selection operator (LASSO) binary logistic regression model. The flatness was the most correlated indicator with IA rupture. (B) Radiomics signature (rad-score) was constructed from a linear combination of selected features that were weighted based on their respective LASSO coefficients.
Performance of the morphology-based radiomics signature
The rad-scores of the ruptured group were significantly higher than that of the unruptured group in both the derivation and validation cohorts (p < 0.001, Table 1, Figure 5). A significant association between the rad-score and IA rupture was also found in the IAs at a different location (Supplementary Table 3). The radiomics signature yielded areas under the curve (AUCs) of 0.814 (CI 95%, 0.746-0.881) in the derivation cohort and 0.835 (CI 95%, 0.739-0.930) in the validation cohort (Figure 6).
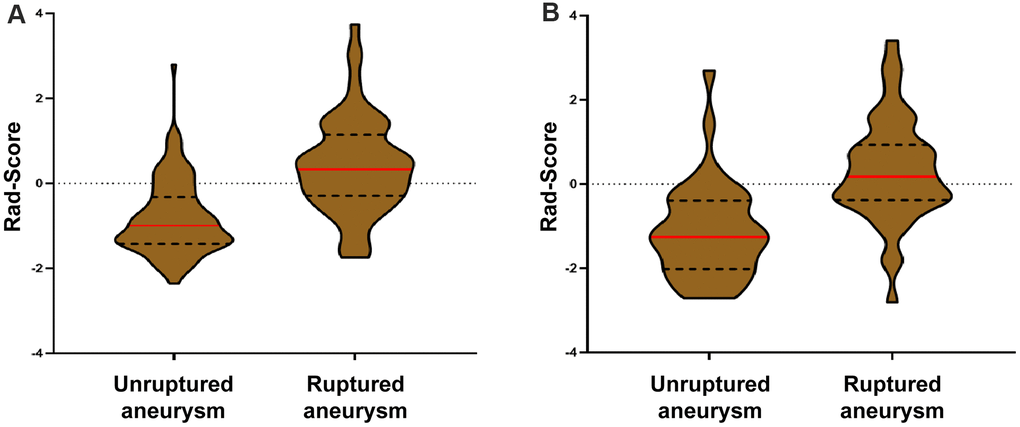
Figure 5. Violin plots of the radiomics signature score (rad-score). There was a significant difference in the rad-score between unruptured IA and ruptured IA in the derivation cohort (p < 0.001, III-A), which was then confirmed in the validation cohort (p < 0.001, III-B).
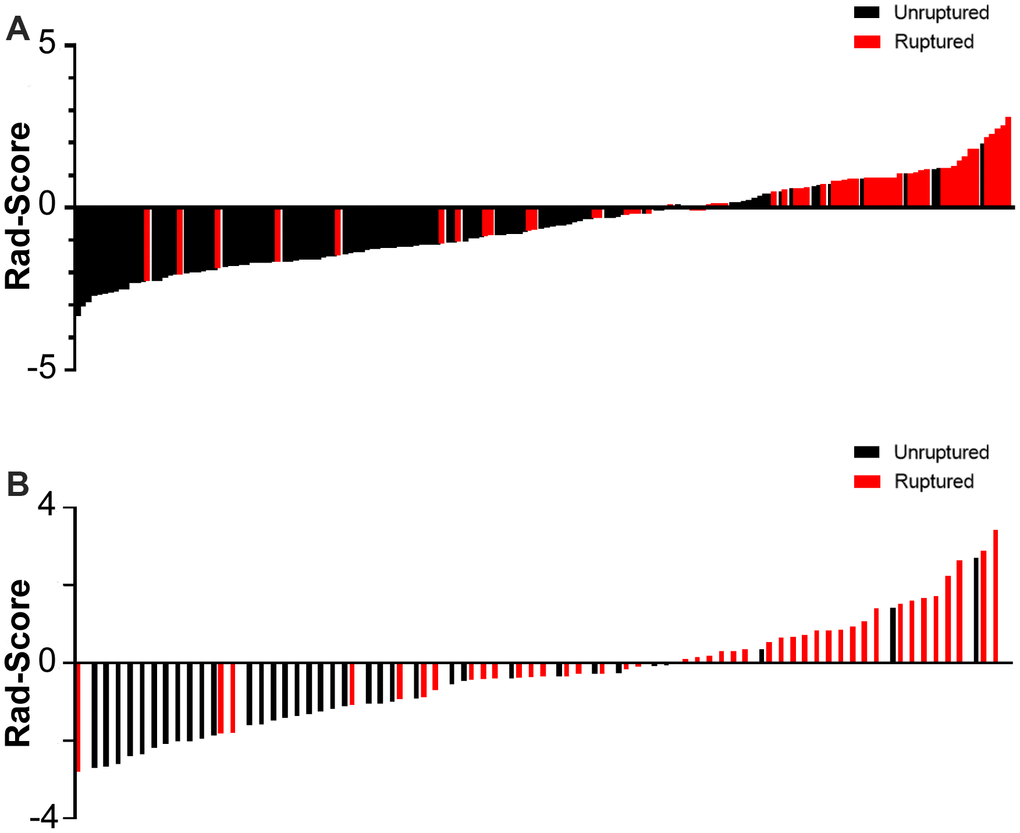
Figure 6. Rad-score for every aneurysm in each in the derivation (A) and validation cohort (B).
Individualized nomogram model development and selection
Multivariate logistic regression analysis yielded 3 rupture discriminations models:
the morphology-based radiomics signature (MRS) model, which include radiomics signature and traditional morphological features,
odds MRS = [0.90(Radiomics Signature) + 0.79(SR) + 1.23(BPR) – 2.84];
the morphology-based radiomics features (MRF) model, which include radiomics features and traditional morphological features,
odds MRF = [0.26(Maximum 3D Diameter) +0.88 (SR) - 5.89(Flatness) + 0.31]; and
the morphology-based traditional features (MTF) model, which include only traditional morphological features,
odds MTF = [1.66 (AR) + 0.96 (NPR) + 0.73 (Irregular shape) – 3.90];
where odds are the ratios of the probability of ruptured status to the probability of unruptured status of an IA.
Independently significant discriminants of the MRS model included radiomics signature, SR, and BPR. Discriminants of the MRF model included flatness, maximum 3D diameter, and SR. Discriminants of the MTF model include AR, NPR, and irregular shape (Table 2). We found that only SR was incorporated in both the MRS model (OR, 3.430; CI 95%, 1.275-4.521) and the MRF model (OR, 2.400; CI 95%, 1.226-4.900).
Table 2. Multivariate analysis for patient with aSAH and MIAs.
| Model | Risk factors | Odds ratio (95% CI) | P | VIF |
MRS
Model | Radiomics Signature | 2.466(1.756-3.618) | 0.003 | 1.116 |
| SR | 3.430(1.275-4.521) | 0.023 | 1.073 |
| BPR | 3.430(1.275-9.890) | 0.018 | 1.056 |
MRF
Model | Flatness | 0.003(<0.001-0.0600) | <0.001 | 1.044 |
| Maximum 3D Diameter | 1.359(0.109-16.488) | 0.010 | 1.307 |
| SR | 2.400(1.226-4.900) | 0.013 | 1.295 |
MTF
Model | AR | 5.240(2.451-12.099) | <0.001 | 1.149 |
| NPR | 2.621(1.373-5.257) | 0.004 | 1.144 |
| Irregular shape | 2.078(1.036-4.173) | 0.039 | 1.022 |
| MRS model, morphology-based radiomics signature model; MRF model, morphology-based radiomics features model; MTF model, morphology-based traditional features model; SR, size ratio; AR, aspect ratio; NPR, neck to parent diameter ratio; VIF, variation inflation factors. |
For all three models, the variance inflation factors (VIFs) of all the candidate indicators ranged from 1.050–1.307, demonstrating that there was no collinearity in any of the three models. The MRS model (AUC, 0.842; 95% CIs, 0.786-0.899) assessed the risk of aneurysm rupture in the derivation cohort more accurately than the MTF model (AUC, 0.747; 95% CIs, 0.673-0.822) or the MRF model (AUC, 0.820; 95% CIs, 0.755-0.885) (Figure 7). In the validation cohort, the MRS model (AUC, 0.849, 95% CIs, 0.752-0.946) also had the largest AUC compared with the MTF (AUC, 0.666; 95% CIs, 0.539-0.793) and MRF models (AUC, 0.799; 95% CIs, 0.697-0.902). As the optimal model, the MRS model was developed as the nomogram (Figure 8A).
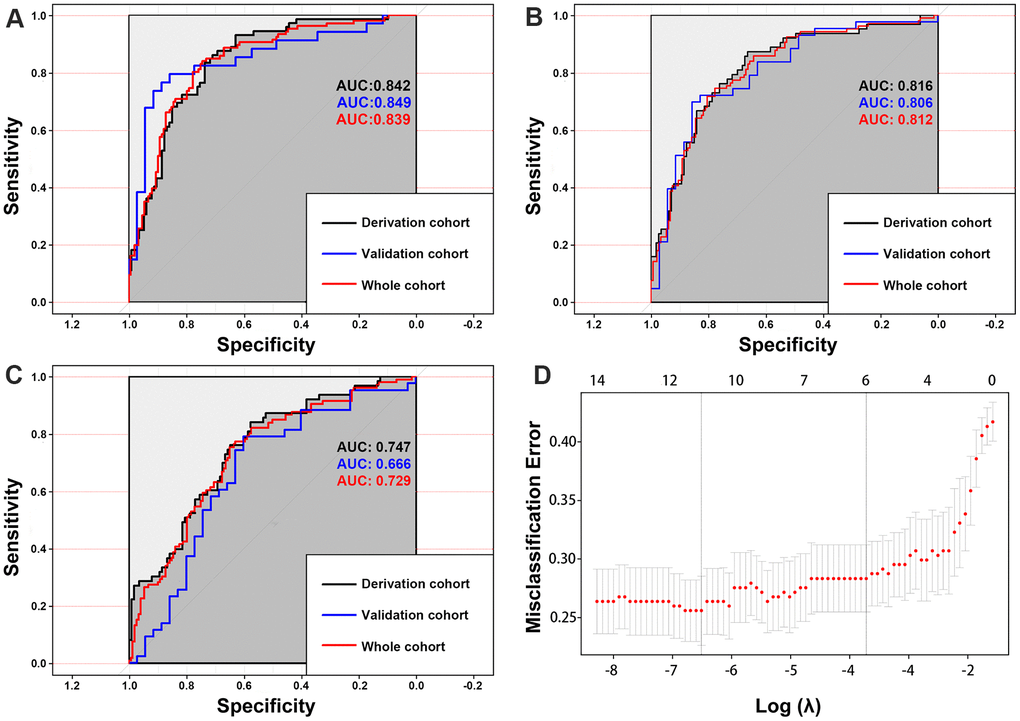
Figure 7. The area under the curves (AUCs) shows that the morphology-based radiomics signature model (A) has better discrimination compared with the morphology-based radiomics features model (B) and morphology-based radiomics features model (C). Radiomics morphological feature selection used the LASSO binary logistic regression model (D).
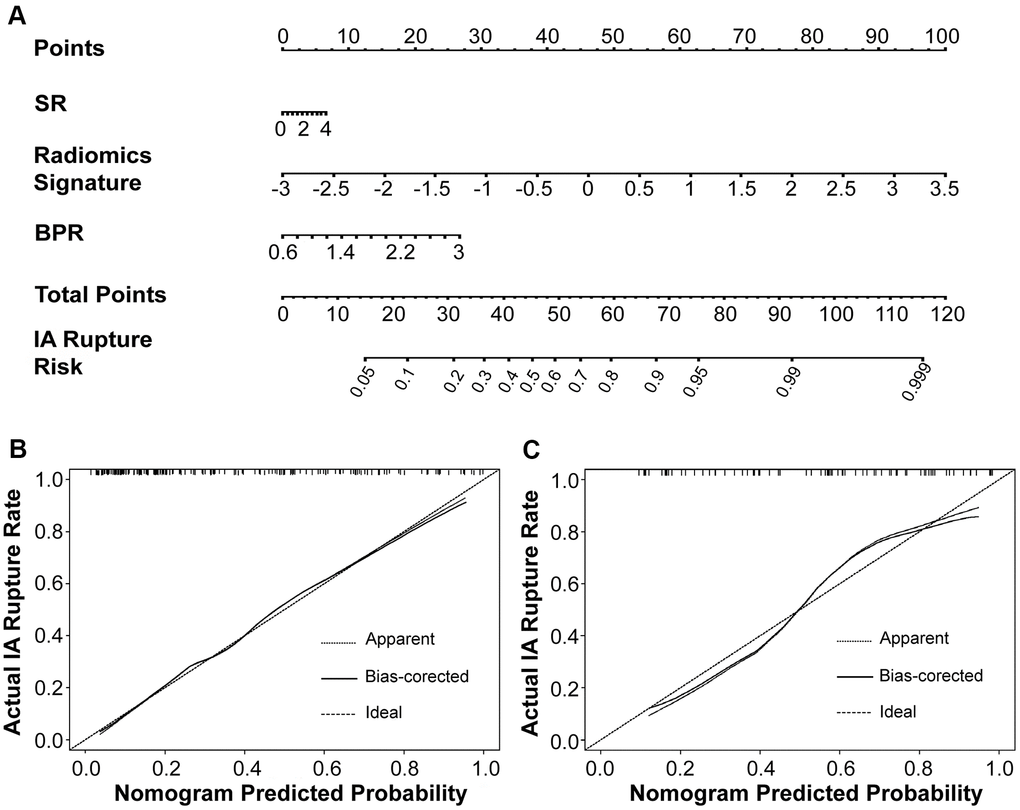
Figure 8. The morphology-based radiomics signature model was developed into nomogram (A). Calibration curves suggest that our nomogram performed well in both the derivation (B) and validation (C) cohorts.