Introduction
Colorectal cancer (CRC) is a kind of molecular heterogeneous disease that undergo a variety of clinical courses and possess diverse therapeutic responses [1–3]. It has developed to be the third most common malignancy in women and the fourth among men, and it is the fifth cause of cancer-related death in China [4]. Emerged early diagnosed test, painless colonoscopy, oncotarget and immune checkpoint therapy have contributed to improving screening, diagnosis and survival of the disease [5–7], nevertheless, the early diagnostic rate and outcome of CRC patient are still unsatisfactory. The incidence and mortality rates of CRC were rapidly increased in developing countries including China [8], and high case-fatality ratio (14.0%) and mortality/incidence ratio (52.1%) were observed in the past decade in China [9]. Therefore, it is urgent for us to explore the effective tools to precisely screening and discriminating the high-risk individual and to directly manage of the recurrent and metastatic patients.
In recent decades, a continued rightward of CRC was reported by several population-based epidemiological studies [10,11], and the different origin of development as well as distinct anatomic structure were observed in colon and rectal cancer [12]. For this, accumulating studies paid more attention to the role of primary tumor sidedness in this disease. It’s widely recognized an obvious clinical and biological distinction within left- and right-sided CRC [13–15]. However, the clinical utility of this distinction remains unclear in adjuvant therapy response, recurrence and clinical outcome within the right- and light-sided localized CRC. Furthermore, the debates in terms of the clinical efficacy of bevacizumab plus adjuvant chemoradiotherpay within metastatic CRC are ongoing. Cetuximab plus fluorouracil based chemotherapy was commonly recommended and accepted for treatment of KRAS wild-type metastatic CRC (mCRC) patient, whereas the left-sided individual was reported more responsive to the therapeutic regimen [16,17], and the survival of left-mCRC individual was extremely superior to the right patients [15,18]. However, the leading cause of this distinct response remains unknown, and other unmeasured confounding factors that would interfere with the regimen efficacy should be considered within the two-sided mCRC.
Systematic inflammation has been reported as an obvious hallmark within CRC [19,20]. It confers to trigger mutation of oncogene and to form a pre-metastatic niche in secondary organs and tissue sites to promote onset and subsequent metastasis of the cancer [21]. Meanwhile, due to the host response and progression of the disease, malnutrition is another significant determinant in mCRC, and it leads to total extended hospital stay time and pro-treatment poor prognosis and life quality of the patients [22,23]. Albumin (Alb) to fibrinogen (Fib) ratio (AFR) and Fib to pre-albumin (pAlb) ratio (FPR), two novel effective indicators for both chronic inflammation and nutrition status, were significantly related to overall survival (OS) within the II-III stage patient in our previous study [24]. Until now, the role of two indicators within the advanced patients undergoing palliative resection, adjuvant chemoradiotherpay or cetuximab and bevacizumab target therapy remains unknown. Thus, a plausible hypothesis in our study is that underlying chronic inflammation and nutritional status represented by AFR and FPR may involve in clinical efficacy of the common therapeutic regimen and outcome of the two-sided mCRC patient.
In present study, we investigated the association between FPR, AFR, localization of the primary tumor, clinical therapy and survival within discovery (302 left-sided and 128 right-sided mCRC patients) and validation cohort (46 left-sided and 31 right-sided mCRC patients). We found that significant severe chronic inflammation and malnutrition represented by FPR in right- and left-sided mCRC contributed to radiochemoresistance, resulting in poor response and survival in both sides of mCRC patient. Circulating FPR was an effective, economical and practice indicator to stratify the patient to receive the optimal therapeutic regimen, and to predict progression and survival of left-sided mCRC patient.
Results
Baseline characteristics of the patients
Overall, a total of 990 firstly diagnosed mCRC patients from November 2011 to May 2015 were prospectively identified in present study, discovery cohort including 430 mCRC patients who didn’t receive targeted therapy and validation cohort containing 77 mCRC cases undergoing bevacizumab plus radiochemotherapy were enrolled as eligible patients according to the inclusion and exclusion criteria. The detail screening flow diagram of eligible patients and the baseline characteristics as well as laboratory detection were described in Figure 1 and Supplementary Table 1. All of the patients were firstly diagnosed mCRC, and liver, peritoneum and multiple site metastasis within the patients accounted for 51.16%, 20.47% and 11.63% in discovery cohort, respectively. Due to poverty or oldness, 20.47% of the patient did not receive any treatment after the firstly diagnosis. Sixty-four and 152 cases received palliative resection and adjuvant radiochemotherapy alone. Only 126 and 77 cases received palliative surgery plus radiochemotherapy and bevacizumab plus radiochemotherapy, respectively. The median AFR and FPR in mCRC patient were 11.13 (IQR: 8.83-14.05) and 23.18 (IQR: 15.31-43.08), 10.42 (IQR: 8.32-12.61) and 25.5 (IQR: 14.57-36.83) in the two cohorts, respectively. After the three years’ follow-up, the median PFS and OS were 8.0 (IQR: 4.0-13.0), 12.0 (IQR: 5.0–23.0) months in discovery cohort and 14.5 (IQR: 8.0-20.0), 16.0 (IQR: 10.0-27.0) in validation cohort, respectively.
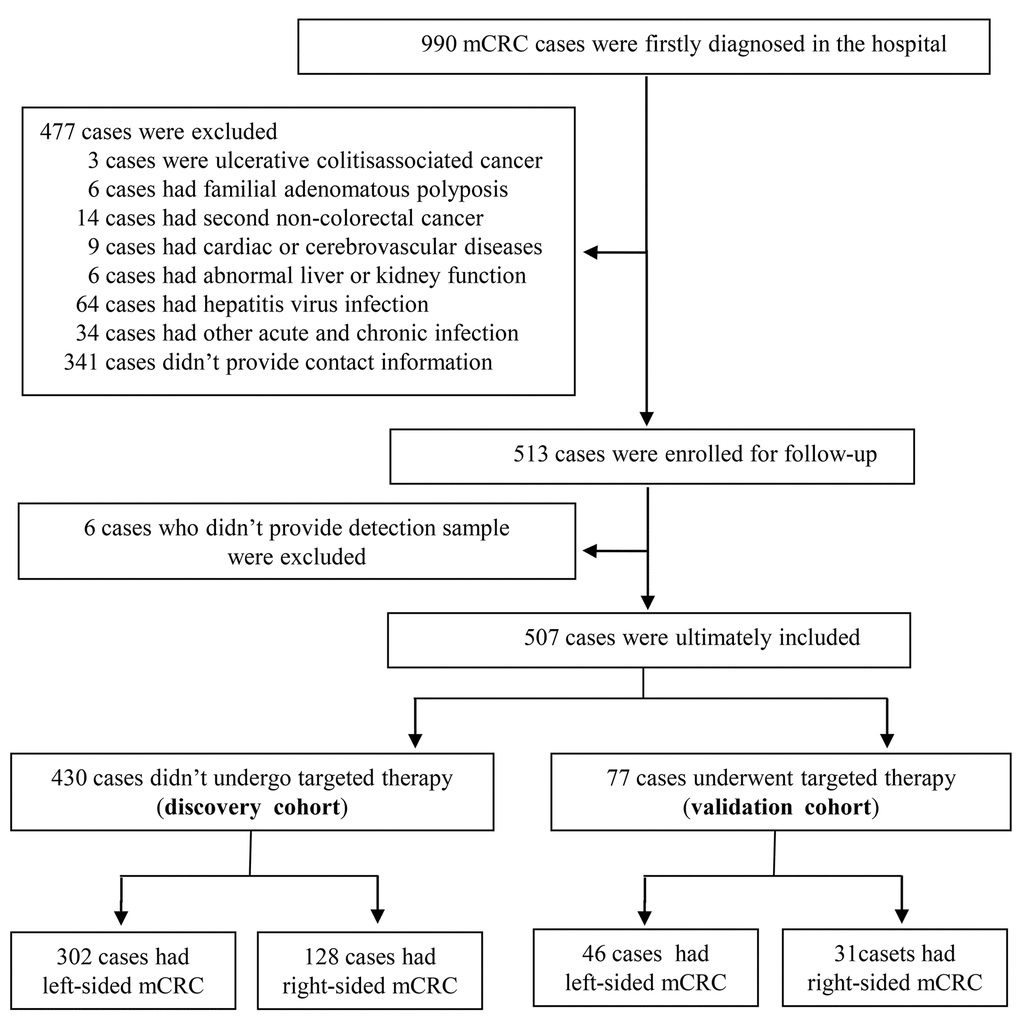
Figure 1. Flow diagram of eligible cases selection in present study.
Systematic inflammation and survival in discovery cohort
In order to investigate the difference of systematic inflammation between left- and right-sided mCRC, we compared the inflammatory indicators in discovery cohort. As shown from Figure 2a-b and Supplementary Figure 1a-b, elevated FPR (p=0.014), Fib (p=0.002), PLR (p<0.001) and low AFR (p<0.001), pAlb (p=0.019), Alb (p=0.003) and LMR (p=0.040) were observed in right-sided mCRC in comparison with the left-sided cancer. However, there was no significant difference of NLR, dNLR, CEA and CA199 between the two-sided diseases. Comparing to left-sided mCRC, the number of dead patient (85.16% vs.78.48%, p=0.004) was obviously increased in right-sided mCRC and OS (13.0 months vs. 9.0 months, plog-rank test=0.005) within left-sided mCRC was extremely longer than that within the right-sided patient, but not PFS (Figure 2c-d). When left-sided mCRC stratified into left colon and rectum, no significant difference of PFS and OS was observed between the two subgroups (Supplementary Figure 1c-d).
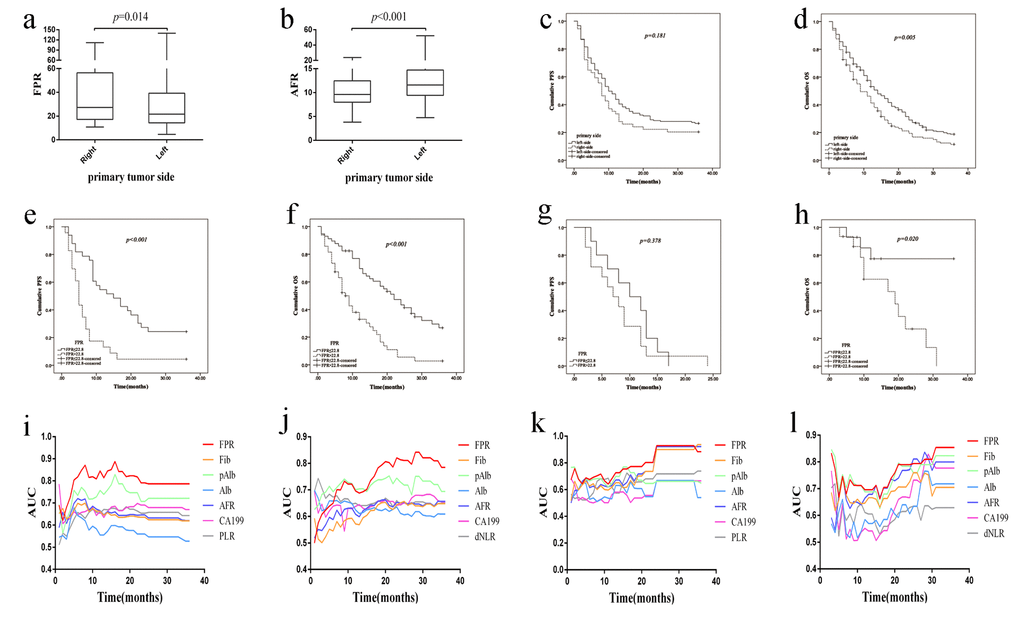
Figure 2. Comparison and evaluation of FPR, AFR and survival between right- and left-sided mCRC patient in two cohorts. (a) FPR in discovery cohort; (b) AFR in discovery cohort; (c) Kaplan-Meier curve of primary tumor sidedness for PFS; (d) Kaplan-Meier curve of primary tumor sidedness for OS; (e) Kaplan-Meier curve of FPR for PFS of left-sided mCRC patient in discovery cohort; (f) Kaplan-Meier curve of FPR for OS of left-sided mCRC patient in discovery cohort; (g) Kaplan-Meier curve of FPR for PFS of left-sided mCRC patient in validation cohort; (h) Kaplan-Meier curve of FPR for OS of left-sided mCRC patient in validation cohort; (i) Time-dependent ROC analysis for PFS of left-sided mCRC patient in discovery cohort; (j) Time-dependent ROC analysis for OS of left-sided mCRC patient in discovery cohort; (k) Time-dependent ROC analysis for PFS in validation cohort; (l) Time-dependent ROC analysis for OS in validation cohort.
Prognostic role of chronic inflammatory indicator in discovery cohort
Using X-tile software, the optimal cut-off points based on OS within the overall mCRC patients were identified as 22.8 for FPR, 9.9 for AFR, 3.9 g/L for Fib, 139.8 mg/L for pAlb, 35.7 g/L for Alb, 2.9 for NLR, 3.7 for dNLR, 166.1 for PLR and 1.5 for LMR in discovery cohort (Supplementary Figure 2). According to the optimal cut-off values, the patients were divided into high and low subgroups by each indicator.
In overall population, results of Kaplan-Meier curve, univariate and multivariate Cox regression showed that median survival of mCRC patients with elevated FPR (plog-rank test<0.001, adjusted HR=1.896, 95%CI=1.097-3.279 for PFS; plog-rank test<0.001, adjusted HR=1.583, 95%CI=1.042-2.405 for OS) was significantly short comparing to those with low FPR, respectively (Supplementary Figure 3a-b and Supplementary Table 2). Furthermore, median PFS of the patient with high PLR (plog-rank test<0.001, adjusted HR=1.601, 95%CI=1.106-2.317) was obviously worse than the cases harbored low PLR, and there were significant differences of OS within high and low subgroup stratified by dNLR (plog-rank test<0.001, adjusted HR=1.629, 95%CI=1.298-2.044), Fib (plog-rank test<0.001, adjusted HR=1.344, 95%CI=1.024-1.764) and pAlb (plog-rank test=0.002, adjusted HR=0.478, 95%CI=0.321-0.711), respectively (Supplementary Table 2).
In left-sided mCRC patients, elevated FPR (plog-rank test<0.001, adjusted HR=2.254, 95%CI=1.167-4.354 for PFS; plog-rank test<0.001, adjusted HR=1.769, 95%CI=1.066- 2.935 for OS), PLR (plog-rank test<0.001, adjusted HR=1.600, 95%CI=1.052-2.234 for PFS), dNLR (plog-rank test<0.001, adjusted HR=1.726, 95%CI=1.294-2.303 for OS), Fib (plog-rank test<0.001, adjusted HR=1.934, 95%CI=1.153-3.243 for PFS; plog-rank test<0.001, adjusted HR=1.428, 95%CI=1.017-2.007 for OS), and low AFR (plog-rank test<0.001, adjusted HR=0.568, 95%CI=0.340-0.951 for PFS), Alb (plog-rank test=0.001, adjusted HR=0.603, 95%CI=0.370-0.983 for PFS; plog-rank test<0.001, adjusted HR=0.716, 95%CI=0.522-0.982 for OS) and pAlb (plog-rank test=0.004, adjusted HR=0.517, 95%CI=0.322-0.831 for OS) were associated with poor survival in Kaplain-Meier curve and Cox regression (Figure 2e-f and Supplementary Table 3).
Comparing to high pAlb patients, poor OS was observed in the patients harbored low pAlb (plog-rank test=0.044) in right-sided mCRC individuals. However, there was no significant association between them when it was adjusted by the other factors. The other inflammatory indicators were not related to the survival of right-sided mCRC patients (Supplementary Figure 3c-d and Supplementary Table 4).
Prognostic role of FPR in validation cohort
In overall population, the median PFS (plog-rank test=0.047, crude HR=1.914, 95%CI=1.022-3.583) and OS (plog-rank test=0.001, crude HR=4.473, 95%CI= 1.648-12.141) within high FPR mCRC patient were obviously worse than the low FPR patient (Supplementary Figure 3e-f). Meanwhile, FPR was still significantly associated with OS (adjusted HR=4.206, 95%CI=1.159-15.266) when it was adjusted by the other confounding factors (Supplementary Table 5). In Kaplan-Meier curve and Cox regression, significant association was also observed between elevated FPR and OS in left-sided mCRC patient (plog-rank test=0.020, crude HR=4.112, 95%CI=1.126-15.015) (Figure 2g-h and Supplementary Table 6). However, no significant association was observed between FPR and survival of right-sided mCRC patient in validation cohort (Supplementary Table 7).
Predicted efficacy of FPR in two cohorts
Time-dependent ROC curve was used to evaluate the predicted efficacy of FPR in mCRC patient, and area under the curve (AUC) was selected as the common tool to compare the difference between them. The AUCs of FPR were 0.749 for PFS and 0.740 for OS in overall discovery cohort (Supplementary Figure 4a-b), and all of them were obviously higher than Fib, pAlb, Alb, AFR, PLR, dNLR and CA199, respectively. In left-sided mCRC individual, the first and second highest AUCs of the indicator predicting survival of the patients was FPR (AUC=0.787 for PFS, AUC=0.785 for OS) and pAlb (AUC=0.721 for PFS, AUC=0.694 for OS) (Figure 2i-j). However, the predicted efficacy of pAlb was significantly inferior to FPR. Unfortunately, the predicted AUC of FPR was lower than the other indicators, and CA199 harbored the highest AUC for predicting PFS (AUC=0.822) and OS (AUC=0.739) in right-sided mCRC (Supplementary Figure 4c-d).
In validation cohort, AUC of FPR was 0.884 for predicting PFS and it was the same to Fib and AFR, but it was significantly higher than the other indicators (Figure 2k). Even more intriguingly, AUC of FPR reached up to 0.854 and it was the best indicator to forecast OS in overall population (Figure 2l). Meanwhile, the indicators that harbored the first and second highest AUCs for predicting OS were AFR (AUC=0.877) and FPR (AUC=0.868) in left-sided mCRC patients, and there was no significant difference between them (Supplementary Figure 4e). FPR (AUC=0.813) and CA199 (AUC=0.798) harbored the higher AUCs for predicting OS in right-sided patients (Supplementary Figure 4f). Due to insufficient data, AUC of FPR for predicting PFS in right- or left-sided patients wasn’t calculated.
FPR and clinical baseline characteristics
The association between FPR and the baseline characteristics was examined in the two cohorts. The numbers of mCRC case with disease progression (overall population: 94.59% vs. 78.57%, p=0.040; left-sided mCRC: 95.65% vs. 75.76%, p=0.047) and death (overall population: 86.84% vs. 65.75%, p=0.007; left-sided mCRC: 85.71% vs. 66.67%, p=0.006) within high FPR subgroup were significant higher than the low group only in overall and left-sided mCRC in discovery cohort (Figure 3a-b). Moreover, the number of death in high FPR subgroup was significant higher than the low group in overall and left-sided mCRC (overall population: 72.00% vs. 21.74%, p<0.001; left-sided mCRC: 73.33% vs. 21.43%, p=0.009) in validation cohort. However, no obvious association was examined between FPR and the other characteristics in two cohorts.
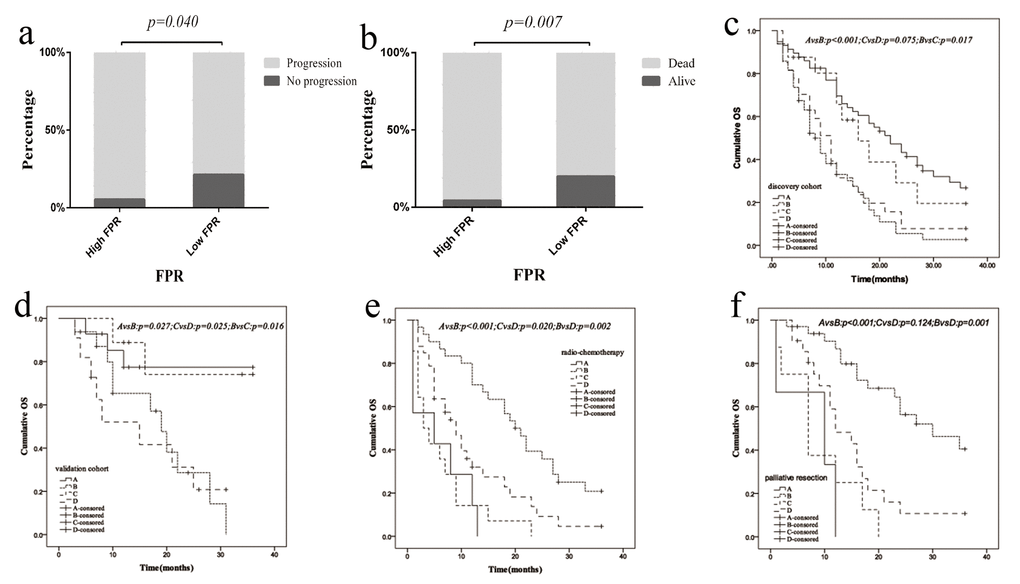
Figure 3. Relationship between FPR, clinical characteristics and primary tumor sidedness as well as clinical therapeutic efficacy in present study. (a) progression status in discovery cohort stratified by FPR ; (b) death status in discovery cohort stratified by FPR; (c) overall survival difference between left- and right-sided CRC cases stratified by FPR in discovery cohort; (d) overall survival difference between left- and right-sided CRC cases stratified by FPR in validation cohort; (e) overall survival difference between high- and low-FPR patients in radiochemotherapy subgroup (no palliative resection); (f) overall survival difference between high- and low-FPR patients in palliative resection subgroup. Abbreviation within in Panels 3c-d: A: left-sided patients with low-FPR; B: left-sided mCRC patients with high-FPR; C: right-sided patients with low-FPR; D: right-sided mCRC patients with high-FPR. Abbreviation within in Panels 3e-f: A: low-FPR mCRC patients without radiochemotherapy; B: low-FPR mCRC patient with radiochemotherapy; C: high-FPR mCRC patient without radiochemotherapy; D: high-FPR mCRC patient with radiochemotherapy.
FPR, primary tumor sidedness and clinical therapeutic regimen
In present study, the relationship between FPR, primary tumor sidedness and therapeutic regimen was investigated to explore the optimal treatment for mCRC patient. The median OS of low and high FPR mCRC patient were 18.0 and 8.0 months, 20.0 and 7.0 months in both overall population and left-sided subgroups of discovery cohort, and the median OS was 16.0 and 10.0 months, 14.0 and 10.0 months in the two subgroups in validation cohort, respectively. Meanwhile, we also observed the survival of left-sided mCRC patients was obviously longer than that of right-sided individuals in discovery cohort (plog-rank test=0.005 for OS). Moreover, the median OS of left-sided mCRC patient with high FPR was obviously worse than right-sided patients harbored low FPR in discovery (plog-rank test=0.017) and validation (plog-rank test=0.016) cohort (Figure 3c-d). Median OS of high FPR cases was extremely poor in comparison with low FPR patients in both radiochemotherapy (plog-rank test=0.002) and palliative resection plus radiochemotherapy subgroup (plog-rank test=0.001) (Figure 3e-f). However, no survival difference was examined between left- and right- sided mCRC individual harbored low (discovery cohort: plog-rank test=0.492, validation cohort: plog-rank test=0.863) or high FPR (discovery cohort: plog-rank test=0.446, validation cohort: plog-rank test=0.792) in the two cohorts (Figure 3c-d).
In low FPR subgroup, the survival of radiochemotherapy treated mCRC patient was significantly longer than those without the treatment in both palliative surgery (plog-rank test<0.001) and non-surgery subgroup (plog-rank test<0.001) (Figure 3e-f). In the same time, the survival of palliative resection plus radiochemotherapy treated mCRC patient was superior to the patients undergoing radiochemotherapy (plog-rank test=0.064). However, no survival difference was observed between palliative resection plus radiochemotherapy treated mCRC patients and the patients undergoing bevacizumab plus radiochemotherapy plog-rank test=0.899 (Figure 4a).
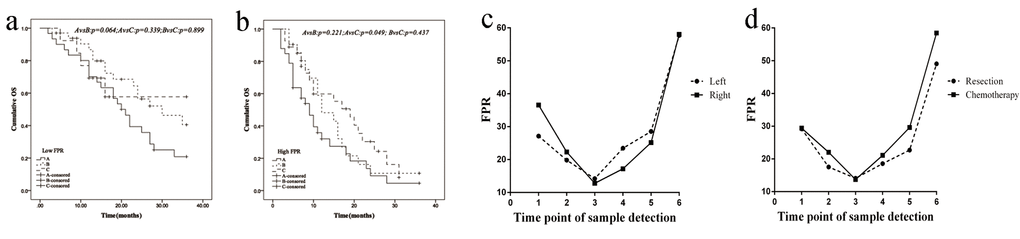
Figure 4. Survival comparison of the patient received different treatments in the high and low FPR subgroups and the dynamic change of FPR during the treatment. (a) Kaplan-Meier curve of OS within the patient received different treatment in low-FPR subgroup; (b) Kaplan-Meier curve of OS within the patient received different treatment in high-FPR subgroup; (c) dynamic change of FPR in left- and right-sided mCRC patients; (d) dynamic change of FPR of mCRC patient undergoing chemotherapy or palliative resection Abbreviation within in Panels 4a-b: A: radiochemotherapy; B: palliative resection plus radiochemotherapy; C: bevacizumab plus radiochemotherapay. Abbreviation within in Panels 4c-d: 1: the diagnostic time; 2: one month after the first treatment; 3: regular examination without disease progression; 4: one month before disease progression; 5: time of imaging confirmed progression; 6: within three months before death.
In high FPR subgroup, the survival was gradually decreased in mCRC patient treated with bevacizumab plus radiochemotherapy, palliative resection plus radiochemotherapy and radiochemotherapy alone (Figure 4b). OS of the patient treated with radiochemotherapy was superior to the non-treated case (plog-rank test =0.020) (Figure 3e). The survival of palliative resection plus radiochemotherapy treated mCRC patient was equal to the patient treated with palliative resection or radiochemotherapy alone (palliative resection: plog-rank test=0.124, radiochemotherapy: plog-rank test=0.221). Whereas, the significant survival difference was observed between bevacizumab plus radiochemotherapy and radiochemotherapy treated mCRC patient (plog-rank test =0.049) (Figure 4b).
Role of FPR in predicting progression of mCRC patients
According to the inclusion criteria and willing of the patient, seventeen palliative resection and thirty-four radiochemotherapy treated mCRC patients were included to investigate the role of FPR in predicting progression of mCRC patients. Each of them provided detected sample in each time point, and all of them were progressed and dead in the follow-up period. As shown from Figure 4c-d, circulating FPR was extremely decreased after the first-treatment, and it reduced significantly to the lowest value in the following two-three months in subgroups stratified by treatment or primary tumor sidedness (all p<0.05). Furthermore, it was significantly increased in the time of one month before clinical imaging confirmed progression compared with the lowest point (p<0.05), and it reached up to the highest value within three months before death (p<0.01).
Assessment of FPR contained prognostic nomogram in overall mCRC cases
Using the significant characteristics and FPR, we established the prognostic nomograms and evaluated progression and death risk of overall mCRC patients within three years. The prognostic nomograms with or without FPR were showed in Figure 5. The c-indexes of prognostic nomograms with FPR were 0.65 for three years’ progression and 0.74 for three years’ OS. On the contrary, c-indexes of the nomograms without FPR predicting three years’ PFS and OS were only 0.62 and 0.69, respectively. Moreover, the predicted efficacy of the nomogram including FPR was significantly higher than that without FPR in predicting both 3 years’ progression (p<0.05) and death (p<0.01).
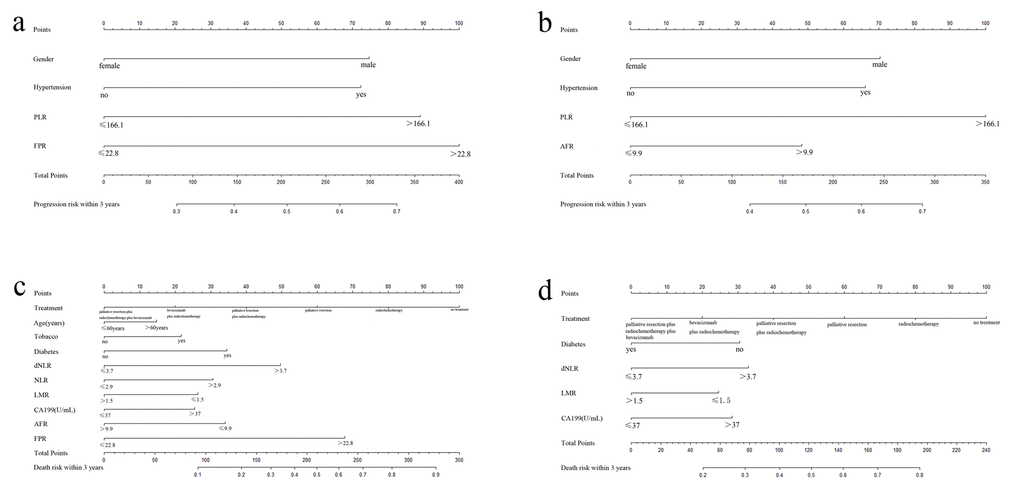
Figure 5. Prognostic nomograms with or without FPR for predicting survival of mCRC patient. (a) nomogram including FPR for predicting 3 years’ PFS; (b) nomogram without FPR for predicting 3 years’ PFS; (c) nomogram including FPR for predicting 3 years’ OS; (d) nomogram without FPR for predicting 3 years’ OS.
Discussion
Despite high risk of disease progression triggered by chronic inflammation and malnutrition [25–28], the prognostic, predictive and monitoring role of FPR in left- and right-sided mCRC is not defined. In present study, we found a significant difference of systematic inflammation between left- and right-sided mCRC patient, high FPR was superior to other inflammatory indicators to independently and effectively predict poor PFS and OS for overall mCRC patients, especially for left-sided mCRC individuals. Moreover, FPR could stratify the patient to achieve maximum benefit from the optimal therapeutic regimen. Circulating dynamic FPR was better than common imaging detection to monitor the progression of the disease after the first treatment. In addition, it could improve the prognostic nomograms to predict the survival of mCRC patient.
It has been well known that Fib, Alb and pAlb are not only commonly recognized as a vital factor in coagulation cascade reaction and as a useful indicator to imply nutrition status, respectively, but also can effectively respond to para-inflammation and systematic inflammation in cancer [29–32]. Hyperfibrinogenemia and hypoalbuminemia are usually detected in CRC patients, particularly in mCRC individual [32,33]. Several studies have reported that circulating AFR and FPR can predict the survival of malignancies such as non-small cell lung cancer, esophageal cancer and hepatocellular carcinoma as well as gastric cancer [34–37]. In present study, severe systematic inflammation represented by FPR and other inflammatory indicators was observed in right-sided mCRC comparing to the left-sided case [15,38], which consisted with the report by Patel M and McSorley ST [39]. More progression and death cases were found in overall and left-sided high FPR mCRC patients, and elevated FPR was significantly associated with poor survival of the overall and left-sided patients in the two cohorts, illustrating that FPR wasn’t correlated with the survival of right-sided mCRC cases, but was an independent prognostic factor in predicting clinical outcome of left-sided mCRC patient. AUCs of FPR for predicting PFS and OS were the highest in overall and left-sided mCRC patients in two cohorts, demonstrating that FPR was the most efficient indicator to predict the prognosis of the patient.
Nowadays, left- and right-sided CRC have been known as two distinct diseases, for significant differences in mutation spectrum of oncogene and anti-oncogene and prognosis of the two-sided diseases [12,40–42]. In our study, we confirmed the previous findings that the right-sided mCRC patients’ survival was inferior to the left-sided cases in discovery cohort. We also found poor survival within high FPR patients in comparison with the low FPR cases in both right- and left-sided patients. OS of right-sided low FPR mCRC patients was superior to the left-sided high FPR cases in the two cohorts, indicating that clinical outcome of right-sided patients was not completely inferior to the left-sided cases, and FPR could be considered as an important stratified factor to predict prognosis of mCRC patients. To our surprise, there was no different survival between the two sides in low or high FPR subgroup, revealing that FPR was an important confounding factor to impact the prognostic role of primary tumor sidedness in mCRC patients, and survival of the patient was not associated with primary tumor sidedness, but was related to the severity of chronic inflammation. Clinical outcome of low FPR patient was superior to the high FPR cases in radiochemotherapy and palliative resection plus radiochemotherapy subgroups, and chemotherapy treated mCRC patient was equal to the patient without any treatment in palliative surgery subgroup, indicating that only low FPR mCRC patients could benefit from the common treatments, and high FPR might confer to radiochemoresistance in both right- and left-sided mCRC patients (Figure 6).
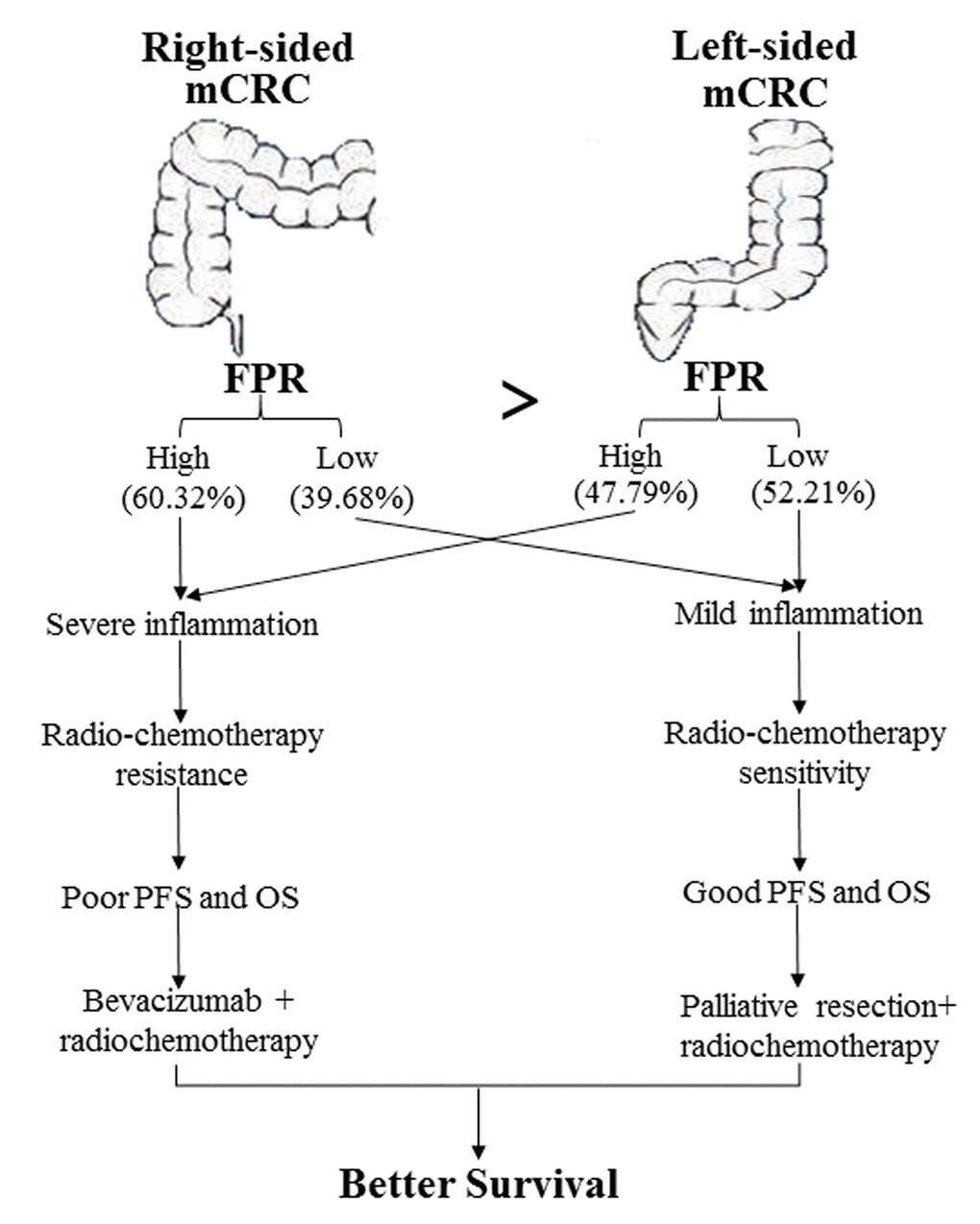
Figure 6. Diagram depicting the cause of survival difference between left- and right-sided mCRC and the optimal common treatment selection for the patients according to FPR.
Our previous study also showed that FPR could stratify the eligible surgical cases who can benefit from adjuvant radiochemotherapy [24]. In present study, the survival of palliative surgery resection plus radiochemotherapy treated low FPR case was the longest in those receiving the common treatments, and was the same to bevacizumab plus radiochemotherapy received patient. On the contrary, survival of bevacizumab plus radiochemotherapy treated high FPR patient was superior to the patient with treatment of adjuvant radiochemotherapy. These findings revealed that palliative resection plus radiochemotherapy and bevacizumab plus radiochemotherapy were the optimal clinical regimens for low and high FPR mCRC patient, respectively (Figure 6). Furthermore, circulating FPR was gradually decreased to the lowest value from the first clinical treatment to the following months without progression, and it was gradually increased from the time of one month before clinical imaging confirmed progression to the last detection before death, elucidating that the indicator could effectively monitor disease progression of the patient. Additionally, the predicted efficacy of prognostic nomogram including FPR was significantly higher than that without the indicator, showing that FPR could improve the prediction efficacy of the prognostic nomogram.
As we known, the interaction between stromal cell, inflammation-related cells such as neutrophil, macrophage and monocyte, inflammatory cytokine and cancer cell remodeled an adapted microenvironment not only to promote progression of the disease but also to involve in resistance to anticancer therapy [43–45]. C-terminal region of Fib γ-chain could interact with CD11b or CD11c/CD18 integrin receptor of inflammatory cell to activate a wide range of inflammatory immune cells such as monocyte, macrophage and neutrophil [46]. These activated immune cells and stromal cells such as CD90+ colonic myofibroblast, fibroblast, endothelial cell could secret interleukin-6(IL-6), IL-21 and IL-33 to activate NF-κB and JAK/STAT pathway to promote systematic inflammation of mCRC by regulating differentiation of T helper 17 cell and regulatory T cell [47–49]. Fib, Alb and pAlb were the acute phase reaction proteins in response to the chronic inflammation [50], IL-6 secreted by cancer-associated fibroblast and cancer cell could inhibit pAlb and stimulate Fib, eventually leading to low pAlb and elevated Fib. Meanwhile, IL-6 contributed to cancer chemoresistance by gp130/MAPK/STAT3 mediated activation of transcription factors C/EBPβ/δ, epithelial to mesenchymal transition, overexpression of p-glycoprotein and expansion of cancer stem cells [51]. Moreover, malajusted miR- 155-5p/C/EBPβ/IL6 signaling in tumor-associated macrophage could induce chemoresistance by regulating the IL6R/STAT3/miR-204-5p axis [52]. On the contrary, down-regulated IL-6/GP130 improved 5-fluorouracil-based chemotherapy sensitivity in colon cancer [53]. Consequently, severe cancer chronic inflammation represented by elevated FPR could confer to radiochemoresistance and poor prognosis. Moreover, Severe malnutrition within mCRC patients damaged the patients’ immunologic defense and surveillance [54,55], resulting in unsatisfied response to adjuvant chemotherapy and poor survival of the cancer patient. Additionally, more severe systematic inflammation was observed in right-sided comparing to left-sided patients, and the majority of right-sided mCRC harbored elevated FPR, and low FPR mCRC cases accounted for a small proportion. Therefore, the prognosis of right-sided mCRC patients was inferior to the left-sided cases, and high FPR conferred to poor clinical efficacy of adjuvant chemotherapy, leading to poor survival of the patient.
The prospective study is the first time for us to evaluate the predictive, prognostic and monitoring role of FPR in left- and right-sided mCRC patients. It is also the first time for us to illustrate that severe systematic inflammation involving in radiochemoresistance is the main reason for the survival difference between left- and right-sided mCRC cases. Additionally, dynamic monitoring FPR can predict the disease progression ahead clinical imaging detection, and prognostic nomogram including FPR can efficiently predict the progression and death outcome of mCRC patients. However, the cases in our study are from the single center, and the sample size isn’t large enough. Thus our findings needed to be validated by other prospective study with large sample size from multiple centers. Moreover, in vivo and in vitro experiments are not carried out to furtherly confirm the association between high FPR, radiochemoresistance and poor survival in the mCRC patient.
Conclusions
In summary, our findings have demonstrated that significant difference of chronic inflammation represented by FPR has an impact on radiochemotherapy sensitivity, resulting in significant survival difference in right- and left-sided mCRC. Elevated FPR is an efficient and independent prognostic factor to predict poor survival of left-sided mCRC patients and to improve the efficacy of its prognostic nomogram. It serves as a readily valuable indicator for monitoring progression and can be considered as a precise stratification factor in future clinical trials aiming to optimize common treatment strategies for the disease.
Materials and Methods
Population
In our study, a total of 990 firstly diagnosed mCRC patients in the Second Affiliated Hospital of Nanchang University were prospectively identified from November 2011 to May 2015. We screened the eligible case according to the following inclusion and exclusion criteria: 1) the patient should be firstly diagnosed as mCRC by X-ray, CT, MRI or pathological detection; 2) all patients should be free of hereditary polyposis and nonpolyposis CRC, emergency surgery, palliative operation, neoadjuvant chemoradiotherapy, ulcerative colitis-associated cancer ahead the clinical confirmation; 3) the eligible cases were not suffered from other malignancies, recent bacterium and virus infection, autoimmune and hematologic as well as cardiovascular and cerebrovascular disease; 4) liver and kidney function should be normal in all the included patients; 5) all included patients didn’t intake either drugs such as antibacterial agent, non-steroidal anti-inflammatory drug, antiplatelet or anticoagulant drug nor intravenous albumin supplement in recent three months; 6) the eligible patient could provide complete clinical characteristics, and contact information for three years’ follow-up; 7) the patient signed the informed consent and they agreed to collect pre-treatment peripheral, serum, and plasma samples for late-stage detection. The study was approved by the Medical Ethics Committee of the local hospital.
Clinical baseline characteristics and follow-up
The baseline characteristics such as demographic and clinicopathological data and clinical therapeutic regimen were extracted from the medical record. The tumor location from ileocecal section to the splenic flexure (without it) and the splenic flexure to rectum were considered as right- and left-sided CRC, respectively. Routine three years’ follow-up (one season a time within the first two years, and six months in the third year) were performed by means of email, telephone, and medical record in all eligible patients after the first time treatment and the follow-up deadline was July 2018. Three years’ progression-free survival (PFS) and overall survival (OS) were the main endpoints in present study, the two of them were measured from the first clinical confirmation until the date of local progression or new distant-site metastasis and death from any cause, respectively.
Sample collection and laboratory detection
In order to investigate the relationship of systematic inflammation, primary tumor location with clinical efficacy and outcome of mCRC patient, the respective two milliliters pre-treatment peripheral blood, serum, and plasma samples were collected from all eligible patients for detection. All the samples were collected at 7:00 to 9:00 am ahead the first clinical confirmed time. Moreover, mCRC patients with both progression and death event were selected to collect these samples in the following each time point (one month after the first treatment, regular examination without disease progression, one month before the progression, time of clinical imaging confirmed progression, within three months before death) and all the detections were completed within two hours after the sample collection.
SYSMEX XE-2100 machine (Sysmex, Tokyo, Japan) with nucleic acid fluorescence staining and laser flow analysis method was used to detect differential white cell count. Plasma Fib was measured by clauss method using SYSMEX CA-7000 machine (Sysmex, Tokyo, Japan). Bromcresol green dye method, immunoturbidimetric assay and electrochemiluminescence immunoassay were selected to examine serum Alb, pAlb, carcinoembryonic antigen (CEA) and carbohydrate antigen 199 (CA199) with machines of OLYMPUS AU5400 (Beckman Coulter, Tokyo, Japan) and SIEMENS ADVIA Centaur CP machine (Siemens, Erlangen, Germany), respectively. The inter- and intra-batch coefficients of variation of immune cell count, Fib, Alb, pAlb, CEA and CA199 kits were less than 5%. According to the detection result, we calculated the following ratios: Alb to Fib ratio (AFR), Fib to pAlb ratio (FPR), neutrophil to lymphocyte ratio (NLR), (total white cell-lymphocyte) to lymphocyte ratio (derived neutrophil to lymphocyte ratio, dNLR), platelet to lymphocyte ratio (PLR), lymphocyte to monocyte ratio (LMR).
Statistics
Continuous variables with normal and skewed distribution were expressed as mean±standard deviation, median and inter-quartile ranger (IQR), respectively. Chi-square or Fisher’s exact test was used to compare the difference of categorical variable, and continuous variable with skewed distribution was compared by Mann-Whitney U test. The optimal cut-off points of Fib, Alb and pAlb and the ratios replying on three years’ OS were determined by X-tile 3.6.1 software (Yale University, New Haven, CT, USA). The difference of survival rate was calculated using Kaplan-Meier curve with log-rank test. Cox proportional regression with hazard ratio (HR) and 95% confidential interval (CI) was applied to examine the prognostic role of clinical baseline characteristics and laboratory detected indicators in overall, left- and right-sided mCRC patient. Prognostic predictive efficacy of the significant factor was assessed and compared by time-dependent receiver operating characteristic (ROC) curve. The significant characteristics and laboratory markers were used to establish PFS and OS prognostic nomograms, and Harrell’s concordance index (c-index) were selected to evaluate their predicted efficacy. All the statistics were analyzed using SPSS. 22.0 (IBM Corp, Armonk, NY, USA) and R 3.5.1(Institute for Statistics and Mathematics, Vienna, Austria). All analyses were two-sided, and p<0.05 was recognized as a statistical significance.
Ethics approval and consent to participate
The study was approved by the institutional ethics committees of the Second Affiliated Hospital of Nanchang University and all procedures were conducted in accordance with ethical principles.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Author Contributions
Qing-Gen Chen and Lei Zhang carried out the sample preparation and detection, performed the data preparation and statistics, and drafted the manuscript. Qing-Gen Chen, Lei Zhang and Xia-Hong You collected the clinical baseline characteristics and carried out the follow-up. Fan Sun, Shu-Qi Li, Yu-Huan Jiang, Wei-Ming Yang and Qiong-Hui Zhong checked the data and revised the manuscript. Hou-Qun Ying and Xiao-Zhong Wang conceived of the study, and participated in its design and coordination, revised and approved the manuscript. All authors read and approved the final manuscript.
Conflicts of Interest
All the authors agree to publish the study and declared no conflicts of interest.
Funding
This report was supported by the National Natural Science Foundation of China (grant number: 81702090), the Natural Science Youth Foundation of Jiangxi Province (grant number: 20171BAB215054), the Key Technology Research and Development Program of Jiangxi Province (grant number: 20171BBG70049) and the Innovation Fund Designated for Graduate Students of Jiangxi Province (grant number: YC2017-S079).
References
- 1. Zhang B, Wang J, Wang X, Zhu J, Liu Q, Shi Z, Chambers MC, Zimmerman LJ, Shaddox KF, Kim S, Davies SR, Wang S, Wang P, et al, and NCI CPTAC. Proteogenomic characterization of human colon and rectal cancer. Nature. 2014; 513:382–87. https://doi.org/10.1038/nature13438 [PubMed]
- 2. Inamura K. Colorectal Cancers: An Update on Their Molecular Pathology. Cancers (Basel). 2018; 10:10. https://doi.org/10.3390/cancers10010026 [PubMed]
- 3. Strum WB. Colorectal Adenomas. N Engl J Med. 2016; 374:1065–75. https://doi.org/10.1056/NEJMra1513581 [PubMed]
- 4. Chen W, Sun K, Zheng R, Zeng H, Zhang S, Xia C, Yang Z, Li H, Zou X, He J. Cancer incidence and mortality in China, 2014. Chin J Cancer Res. 2018; 30:1–12. https://doi.org/10.21147/j.issn.1000-9604.2018.01.01 [PubMed]
- 5. Bergheim J, Semaan A, Gevensleben H, Groening S, Knoblich A, Dietrich J, Weber J, Kalff JC, Bootz F, Kristiansen G, Dietrich D. Potential of quantitative SEPT9 and SHOX2 methylation in plasmatic circulating cell-free DNA as auxiliary staging parameter in colorectal cancer: a prospective observational cohort study. Br J Cancer. 2018; 118:1217–28. https://doi.org/10.1038/s41416-018-0035-8 [PubMed]
- 6. Singal AG, Gupta S, Skinner CS, Ahn C, Santini NO, Agrawal D, Mayorga CA, Murphy C, Tiro JA, McCallister K, Sanders JM, Bishop WP, Loewen AC, Halm EA. Effect of Colonoscopy Outreach vs Fecal Immunochemical Test Outreach on Colorectal Cancer Screening Completion: A Randomized Clinical Trial. JAMA. 2017; 318:806–15. https://doi.org/10.1001/jama.2017.11389 [PubMed]
- 7. Overman MJ, McDermott R, Leach JL, Lonardi S, Lenz HJ, Morse MA, Desai J, Hill A, Axelson M, Moss RA, Goldberg MV, Cao ZA, Ledeine JM, et al. Nivolumab in patients with metastatic DNA mismatch repair-deficient or microsatellite instability-high colorectal cancer (CheckMate 142): an open-label, multicentre, phase 2 study. Lancet Oncol. 2017; 18:1182–91. https://doi.org/10.1016/S1470-2045(17)30422-9 [PubMed]
- 8. Arnold M, Sierra MS, Laversanne M, Soerjomataram I, Jemal A, Bray F. Global patterns and trends in colorectal cancer incidence and mortality. Gut. 2017; 66:683–91. https://doi.org/10.1136/gutjnl-2015-310912 [PubMed]
- 9. Zhu J, Tan Z, Hollis-Hansen K, Zhang Y, Yu C, Li Y. Epidemiological Trends in Colorectal Cancer in China: An Ecological Study. Dig Dis Sci. 2017; 62:235–43. https://doi.org/10.1007/s10620-016-4362-4 [PubMed]
- 10. Li M, Gu J. Changing patterns of colorectal cancer in China over a period of 20 years. World J Gastroenterol. 2005; 11:4685–88. https://doi.org/10.3748/wjg.v11.i30.4685 [PubMed]
- 11. Fang YJ, Wu XJ, Zhao Q, Li LR, Lu ZH, Ding PR, Zhang RX, Kong LH, Wang FL, Lin JZ, Chen G, Pan ZZ, Wan DS. Hospital-based colorectal cancer survival trend of different tumor locations from 1960s to 2000s. PLoS One. 2013; 8:e73528. https://doi.org/10.1371/journal.pone.0073528 [PubMed]
- 12. Iacopetta B. Are there two sides to colorectal cancer? Int J Cancer. 2002; 101:403–08. https://doi.org/10.1002/ijc.10635 [PubMed]
- 13. Bufill JA. Colorectal cancer: evidence for distinct genetic categories based on proximal or distal tumor location. Ann Intern Med. 1990; 113:779–88. https://doi.org/10.7326/0003-4819-113-10-779 [PubMed]
- 14. Price TJ, Beeke C, Ullah S, Padbury R, Maddern G, Roder D, Townsend AR, Moore J, Roy A, Tomita Y, Karapetis C. Does the primary site of colorectal cancer impact outcomes for patients with metastatic disease? Cancer. 2015; 121:830–35. https://doi.org/10.1002/cncr.29129 [PubMed]
- 15. Lee GH, Malietzis G, Askari A, Bernardo D, Al-Hassi HO, Clark SK. Is right-sided colon cancer different to left-sided colorectal cancer? - a systematic review. Eur J Surg Oncol. 2015; 41:300–08. https://doi.org/10.1016/j.ejso.2014.11.001 [PubMed]
- 16. Lièvre A, Ouine B, Canet J, Cartier A, Amar Y, Cacheux W, Mariani O, Guimbaud R, Selves J, Lecomte T, Guyetant S, Bieche I, Berger F, de Koning L. Correction: protein biomarkers predictive for response to anti-EGFR treatment in RAS wild-type metastatic colorectal carcinoma. Br J Cancer. 2018; 119:387. https://doi.org/10.1038/s41416-018-0130-x [PubMed]
- 17. Brulé SY, Jonker DJ, Karapetis CS, O’Callaghan CJ, Moore MJ, Wong R, Tebbutt NC, Underhill C, Yip D, Zalcberg JR, Tu D, Goodwin RA. Brulã© SY, Jonker DJ, Karapetis CS, O’Callaghan CJ, Moore MJ, Wong R, Tebbutt NC, Underhill C, Yip D, Zalcberg JR. Location of colon cancer (right-sided versus left-sided) as a prognostic factor and a predictor of benefit from cetuximab in NCIC CO.17. Eur J Cancer. 2015; 51:1405–14. https://doi.org/10.1016/j.ejca.2015.03.015
- 18. Kamran SC, Clark JW, Zheng H, Borger DR, Blaszkowsky LS, Allen JN, Kwak EL, Wo JY, Parikh AR, Nipp RD, Murphy JE, Goyal L, Zhu AX, et al. Primary tumor sidedness is an independent prognostic marker for survival in metastatic colorectal cancer: results from a large retrospective cohort with mutational analysis. Cancer Med. 2018; 7:2934–42. https://doi.org/10.1002/cam4.1558 [PubMed]
- 19. Itzkowitz SH, Yio X. Inflammation and cancer IV. Colorectal cancer in inflammatory bowel disease: the role of inflammation. Am J Physiol Gastrointest Liver Physiol. 2004; 287:G7–17. https://doi.org/10.1152/ajpgi.00079.2004 [PubMed]
- 20. Terzić J, Grivennikov S, Karin E, Karin M. Inflammation and colon cancer. Gastroenterology. 2010; 138:2101–2114.e5. https://doi.org/10.1053/j.gastro.2010.01.058 [PubMed]
- 21. Solinas G, Marchesi F, Garlanda C, Mantovani A, Allavena P. Inflammation-mediated promotion of invasion and metastasis. Cancer Metastasis Rev. 2010; 29:243–48. https://doi.org/10.1007/s10555-010-9227-2 [PubMed]
- 22. Barao K, Abe Vicente Cavagnari M, Silva Fucuta P, Manoukian Forones N. Association Between Nutrition Status and Survival in Elderly Patients With Colorectal Cancer. Nutr Clin Pract. 2017; 32:658–63. https://doi.org/10.1177/0884533617706894 [PubMed]
- 23. Read JA, Choy ST, Beale PJ, Clarke SJ. Evaluation of nutritional and inflammatory status of advanced colorectal cancer patients and its correlation with survival. Nutr Cancer. 2006; 55:78–85. https://doi.org/10.1207/s15327914nc5501_10 [PubMed]
- 24. Sun F, Peng HX, Gao QF, Li SQ, Zhang J, Chen QG, Jiang YH, Zhang L, Wang XZ, Ying HQ. Preoperative circulating FPR and CCF score are promising biomarkers for predicting clinical outcome of stage II-III colorectal cancer patients. Cancer Manag Res. 2018; 10:2151–61. https://doi.org/10.2147/CMAR.S167398 [PubMed]
- 25. Mantovani A, Allavena P, Sica A, Balkwill F. Cancer-related inflammation. Nature. 2008; 454:436–44. https://doi.org/10.1038/nature07205 [PubMed]
- 26. Balkwill F, Mantovani A. Inflammation and cancer: back to Virchow? Lancet. 2001; 357:539–45. https://doi.org/10.1016/S0140-6736(00)04046-0 [PubMed]
- 27. Yim GW, Eoh KJ, Kim SW, Nam EJ, Kim YT. Malnutrition Identified by the Nutritional Risk Index and Poor Prognosis in Advanced Epithelial Ovarian Carcinoma. Nutr Cancer. 2016; 68:772–79. https://doi.org/10.1080/01635581.2016.1159702 [PubMed]
- 28. Ikeda M, Natsugoe S, Ueno S, Baba M, Aikou T. Significant host- and tumor-related factors for predicting prognosis in patients with esophageal carcinoma. Ann Surg. 2003; 238:197–202. https://doi.org/10.1097/01.sla.0000080822.22415.cb [PubMed]
- 29. Cai W, Kong W, Dong B, Zhang J, Chen Y, Xue W, Huang Y, Zhou L, Huang J. Pretreatment Serum Prealbumin as an Independent Prognostic Indicator in Patients With Metastatic Renal Cell Carcinoma Using Tyrosine Kinase Inhibitors as First-Line Target Therapy. Clin Genitourin Cancer. 2017; 15:e437–46. https://doi.org/10.1016/j.clgc.2017.01.008 [PubMed]
- 30. Kelly P, Paulin F, Lamont D, Baker L, Clearly S, Exon D, Thompson A. Pre-treatment plasma proteomic markers associated with survival in oesophageal cancer. Br J Cancer. 2012; 106:955–61. https://doi.org/10.1038/bjc.2012.15 [PubMed]
- 31. Allin KH, Bojesen SE, Nordestgaard BG. Inflammatory biomarkers and risk of cancer in 84,000 individuals from the general population. Int J Cancer. 2016; 139:1493–500. https://doi.org/10.1002/ijc.30194 [PubMed]
- 32. Nazha B, Moussaly E, Zaarour M, Weerasinghe C, Azab B. Hypoalbuminemia in colorectal cancer prognosis: nutritional marker or inflammatory surrogate? World J Gastrointest Surg. 2015; 7:370–77. https://doi.org/10.4240/wjgs.v7.i12.370 [PubMed]
- 33. Yamashita H, Kitayama J, Taguri M, Nagawa H. Effect of preoperative hyperfibrinogenemia on recurrence of colorectal cancer without a systemic inflammatory response. World J Surg. 2009; 33:1298–305. https://doi.org/10.1007/s00268-009-9992-7 [PubMed]
- 34. Li SQ, Jiang YH, Lin J, Zhang J, Sun F, Gao QF, Zhang L, Chen QG, Wang XZ, Ying HQ. Albumin-to-fibrinogen ratio as a promising biomarker to predict clinical outcome of non-small cell lung cancer individuals. Cancer Med. 2018; 7:1221–31. https://doi.org/10.1002/cam4.1428 [PubMed]
- 35. Gao QF, Qiu JC, Huang XH, Xu YM, Li SQ, Sun F, Zhang J, Yang WM, Min QH, Jiang YH, Chen QG, Zhang L, Wang XZ, Ying HQ. The predictive and prognostic role of a novel ADS score in esophageal squamous cell carcinoma patients undergoing esophagectomy. Cancer Cell Int. 2018; 18:153. https://doi.org/10.1186/s12935-018-0648-2 [PubMed]
- 36. Zhang L, Chen QG, Li SQ, Zhang J, Ying HQ. Preoperative fibrinogen to prealbumin ratio as a novel predictor for clinical outcome of hepatocellular carcinoma. Future Oncol. 2019; 15:13–22. https://doi.org/10.2217/fon-2018-0376 [PubMed]
- 37. Zhang J, Li SQ, Liao ZH, Jiang YH, Chen QG, Huang B, Liu J, Xu YM, Lin J, Ying HQ, Wang XZ. Prognostic value of a novel FPR biomarker in patients with surgical stage II and III gastric cancer. Oncotarget. 2017; 8:75195–205. https://doi.org/10.18632/oncotarget.20661 [PubMed]
- 38. Kirby JA, Bone M, Robertson H, Hudson M, Jones DE. The number of intraepithelial T cells decreases from ascending colon to rectum. J Clin Pathol. 2003; 56:158. https://doi.org/10.1136/jcp.56.2.158 [PubMed]
- 39. Patel M, McSorley ST, Park JH, Roxburgh CS, Edwards J, Horgan PG, McMillan DC. The relationship between right-sided tumour location, tumour microenvironment, systemic inflammation, adjuvant therapy and survival in patients undergoing surgery for colon and rectal cancer. Br J Cancer. 2018; 118:705–12. https://doi.org/10.1038/bjc.2017.441 [PubMed]
- 40. Takahashi Y, Sugai T, Habano W, Ishida K, Eizuka M, Otsuka K, Sasaki A, Takayuki Matsumoto, Morikawa T, Unno M, Suzuki H. Molecular differences in the microsatellite stable phenotype between left-sided and right-sided colorectal cancer. Int J Cancer. 2016; 139:2493–501. https://doi.org/10.1002/ijc.30377 [PubMed]
- 41. Sinicrope FA, Mahoney MR, Yoon HH, Smyrk TC, Thibodeau SN, Goldberg RM, Nelson GD, Sargent DJ, Alberts SR, and Alliance for Clinical Trials in Oncology. Analysis of Molecular Markers by Anatomic Tumor Site in Stage III Colon Carcinomas from Adjuvant Chemotherapy Trial NCCTG N0147 (Alliance). Clin Cancer Res. 2015; 21:5294–304. https://doi.org/10.1158/1078-0432.CCR-15-0527 [PubMed]
- 42. Summers MG, Smith CG, Maughan TS, Kaplan R, Escott-Price V, Cheadle JP. BRAF and NRAS Locus-Specific Variants Have Different Outcomes on Survival to Colorectal Cancer. Clin Cancer Res. 2017; 23:2742–49. https://doi.org/10.1158/1078-0432.CCR-16-1541 [PubMed]
- 43. Candido J, Hagemann T. Cancer-related inflammation. J Clin Immunol. 2013; 33:S79–84. https://doi.org/10.1007/s10875-012-9847-0 [PubMed]
- 44. Che Y, Wang J, Li Y, Lu Z, Huang J, Sun S, Mao S, Lei Y, Zang R, Sun N, He J. Cisplatin-activated PAI-1 secretion in the cancer-associated fibroblasts with paracrine effects promoting esophageal squamous cell carcinoma progression and causing chemoresistance. Cell Death Dis. 2018; 9:759. https://doi.org/10.1038/s41419-018-0808-2 [PubMed]
- 45. Bakker E, Qattan M, Mutti L, Demonacos C, Krstic-Demonacos M. The role of microenvironment and immunity in drug response in leukemia. Biochim Biophys Acta. 2016; 1863:414–26. https://doi.org/10.1016/j.bbamcr.2015.08.003 [PubMed]
- 46. Davalos D, Akassoglou K. Fibrinogen as a key regulator of inflammation in disease. Semin Immunopathol. 2012; 34:43–62. https://doi.org/10.1007/s00281-011-0290-8 [PubMed]
- 47. Huynh PT, Beswick EJ, Coronado YA, Johnson P, O’Connell MR, Watts T, Singh P, Qiu S, Morris K, Powell DW, Pinchuk IV. CD90(+) stromal cells are the major source of IL-6, which supports cancer stem-like cells and inflammation in colorectal cancer. Int J Cancer. 2016; 138:1971–81. https://doi.org/10.1002/ijc.29939 [PubMed]
- 48. Camporeale A, Poli V. IL-6, IL-17 and STAT3: a holy trinity in auto-immunity? Front Biosci. 2012; 17:2306–26. https://doi.org/10.2741/4054 [PubMed]
- 49. Li Y, Shi J, Qi S, Zhang J, Peng D, Chen Z, Wang G, Wang Z, Wang L. IL-33 facilitates proliferation of colorectal cancer dependent on COX2/PGE2. J Exp Clin Cancer Res. 2018; 37:196. https://doi.org/10.1186/s13046-018-0839-7 [PubMed]
- 50. Ceciliani F, Giordano A, Spagnolo V. The systemic reaction during inflammation: the acute-phase proteins. Protein Pept Lett. 2002; 9:211–23. https://doi.org/10.2174/0929866023408779 [PubMed]
- 51. Conze D, Weiss L, Regen PS, Bhushan A, Weaver D, Johnson P, Rincón M. Autocrine production of interleukin 6 causes multidrug resistance in breast cancer cells. Cancer Res. 2001; 61:8851–58. [PubMed]
- 52. Yin Y, Yao S, Hu Y, Feng Y, Li M, Bian Z, Zhang J, Qin Y, Qi X, Zhou L, Fei B, Zou J, Hua D, Huang Z. The Immune-microenvironment Confers Chemoresistance of Colorectal Cancer through Macrophage-Derived IL6. Clin Cancer Res. 2017; 23:7375–87. https://doi.org/10.1158/1078-0432.CCR-17-1283 [PubMed]
- 53. Li S, Tian J, Zhang H, Zhou S, Wang X, Zhang L, Yang J, Zhang Z, Ji Z. Down-regulating IL-6/GP130 targets improved the anti-tumor effects of 5-fluorouracil in colon cancer. Apoptosis. 2018; 23:356–74. https://doi.org/10.1007/s10495-018-1460-0 [PubMed]
- 54. Leischner C, Burkard M, Pfeiffer MM, Lauer UM, Busch C, Venturelli S. Nutritional immunology: function of natural killer cells and their modulation by resveratrol for cancer prevention and treatment. Nutr J. 2016; 15:47. https://doi.org/10.1186/s12937-016-0167-8 [PubMed]
- 55. Cuervo AM, Macian F. Autophagy, nutrition and immunology. Mol Aspects Med. 2012; 33:2–13. https://doi.org/10.1016/j.mam.2011.09.001 [PubMed]



