Introduction
Chimeric antigen receptor (CAR) T cells are therapeutic T cells that have been genetically engineered to express receptors that recognize specific cancer antigens [1, 2]. In cancer biology, multiple mechanisms can cause cancer cells to escape immune surveillance. Among them, a major issue is the thymic elimination of high-affinity T-cell receptors (TCRs), which leads to relatively low-affinity TCRs against “self” antigens including some cancer antigens [3]. CARs are devised to re-direct T cells to recognize and destroy cancer cells as “foreign” agents. In a typical CAR, the single-chain variable fragment (ScFv) of a cancer antigen-recognizing antibody is fused to the intracellular fragment of the TCR containing the signaling domains CD3ζ and co-stimulatory domains CD28 and 4-1BB [4]. The CARs-encoding DNA is generally delivered into a patient’s T cells in vitro through virus transduction. The T cells expressing the CAR (CAR T cells) are then infused back into the patient’s circulatory system. Due to the high affinity of the ScFv to cancer antigens, CAR T cells can recognize and destroy cancer cells that have escaped the host immune surveillance.
In recent years, CAR T-cell therapies for B cell malignancies have seen dramatic clinical responses with high rates of complete remission [5]. However, their applications in solid tumors remain challenging [1]. Different from leukemia, solid tumors have densely packed cancer cells lacking sufficient nutrients and oxygen and under differential interstitial fluid pressure [6, 7]. The tumor interstitial fluid pressure (TIFP) is caused by rapid accumulation of cancer cell mass, overly stimulated angiogenesis, and interstitial fibrosis [8]. TIFP is estimated to be 5~40 mmHg higher than normal tissues [9–11]. High TIFP can lead to inadequate tumor perfusion resulting from missing lymphatic vessels, a leaky and immature tumor vasculature, which in turn cause inadequate lymphocyte infiltration and drug delivery [8, 12]. High TIFP has also been shown to rewire the global gene transcription programs related to extracellular matrix and stress resistance, leading to growth advantage under the adverse tumor microenvironment [13, 14]. Consistently, high TIFP is correlated with poor prognosis, metastasis and resistance to radiation therapy, and chemotherapy in many types of cancer [15–19]. Lowering TIFP decreases cancerous proliferation and shows promising results in improving chemotherapy [20, 21]. However, in contrast to hypoxia and nutrient limitation, how TIFP induces resistance to cancer therapy remains poorly understood.
PD-1 and PD-L1 are immune checkpoint proteins that mediate cytotoxicity of cancer immune therapy [22, 23]. PD-1 is expressed by activated T lymphocytes and other immune cells on the cell membrane [24]. Tumor cells broadly express PD-1 ligands PD-L1 and PD-L2, which interact with PD-1, therefore inhibiting lymphocyte-mediated cytotoxicity. High PD-L1 expression predicts poor survival in many types of cancer [25, 26]. Anti-PD-1 antibodies such as Pembrolizumab and Cemiplimab block the interaction between PD-1 and PD-L1, therefore improving the cytotoxicity of T cells [27]. Pembrolizumab and Cemiplimab have been approved by FDA as second-line treatment for leukemias refractory to chemotherapy [4]. In the solid tumor microenvironment, hypoxia increases the expression of PD-L1 in various tumor cells, leading to decreased T cell cytotoxicity and increased immune escape [28]. Whether elevated pressure in solid tumors could alter immune checkpoint protein has not been reported.
In this study, we investigated if elevated pressure could affect αROR1-CAR T cell-mediated cytotoxicity in lung cancer cell line A549 and whether immune checkpoint protein PD-L1 was involved. Our results showed that applying additional 100 mmHg to A549 cells reduced the potential of αROR1-CAR T cells to kill A549 cancer cells. We found that the reduced cytotoxicity was attributed to increased PD-L1 expression in A549 cells in response to elevated pressure. Blocking PD-1 and PD-L1 interaction by Pembrolizumab or Cemiplimab increased cytokine release and enhanced αROR1-CAR T cell-mediated cytotoxicity. We further confirmed these results in xenograft mice. Our study could have significant implications for the clinical treatment of solid tumors.
Results
Elevated pressure reduced αROR1-CAR T cell-mediated cytotoxicity in A549 lung cancer cells
We have been interested in improving CAR T cells for solid cancer treatment. We constructed an αROR1-CAR using the highly specific ScFv of a rabbit anti-human ROR1 monoclonal antibody (mAb) published before [29] (see details in Methods). ROR1 was broadly expressed on many tumor cells, including lung adenocarcinomas cell A549 [30, 31]. αROR1-CAR T cells can be activated by ROR1-ScFv conjugation, releasing cytokines including IL-2, IFN-γ and TNF-α and inducing cytotoxicity in cancer cells (Figure 1A). To evaluate whether pressure would alter the cytotoxicity of αROR1-CAR T cells to A549 cells, we added freshly prepared αROR1-CAR T cells to A549 cells that have been cultured in normal or elevated pressure (+100 mmHg) for 2 passages (~7 days). After 4 hours of co-culture, the αROR1-CAR T cells effectively induced apoptotic cell death in A549 cells (Figure 1B–1D). Importantly, both apoptosis and cell death were reduced by elevated pressure. Elevated pressure did not affect apoptosis of A549 cells alone; instead, it slightly increased the cell death in several experimental repeats (Figure 1D).
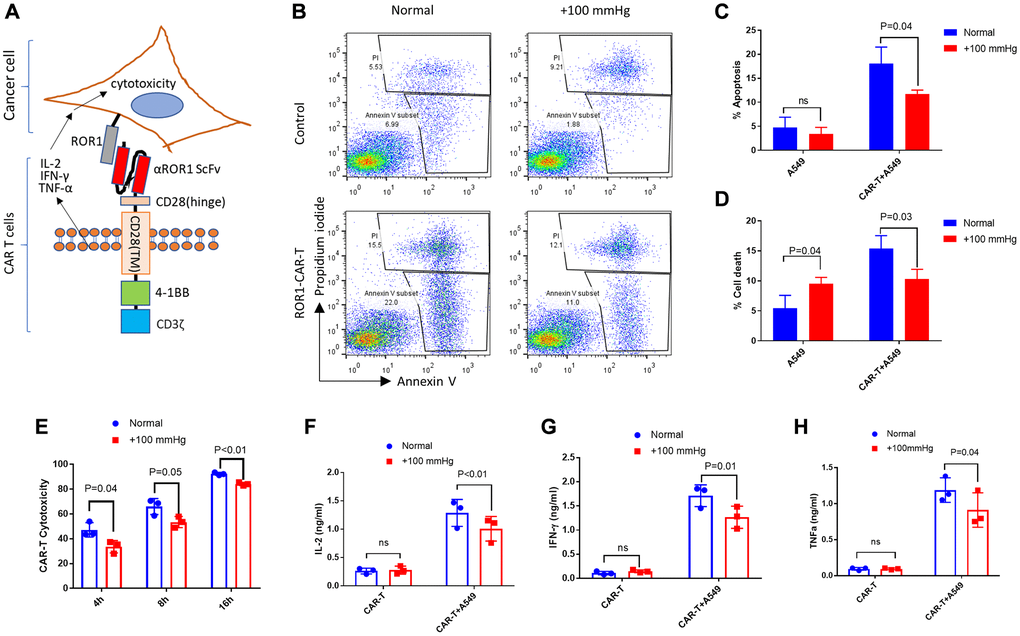
To conveniently evaluate the cytotoxicity of our αROR1-CAR T cells, we incubated A549-Red-Fluc cells stably expressing fly luciferase with CAR-T cells for 4, 8, and 16 hours, and measured cell viability through detecting luciferase activity. Consistently with the flow cytometry results, elevated pressure slightly reduced the cytotoxicity of αROR1-CAR T cells to A549-Red-Fluc cells (Figure 1E). We measured the common cytokines involved in T cell proliferation and cytotoxicity including IL-2, IFN-γ and TNF-α. The results showed that elevated pressure reduced the secretion of these cytokines (Figure 1F–1H). Similar results were obtained by using PBMCs (peripheral blood mononuclear cell) from two other donors.
Pressure preconditioning did not affect the cytotoxicity of αROR1-CAR T cells
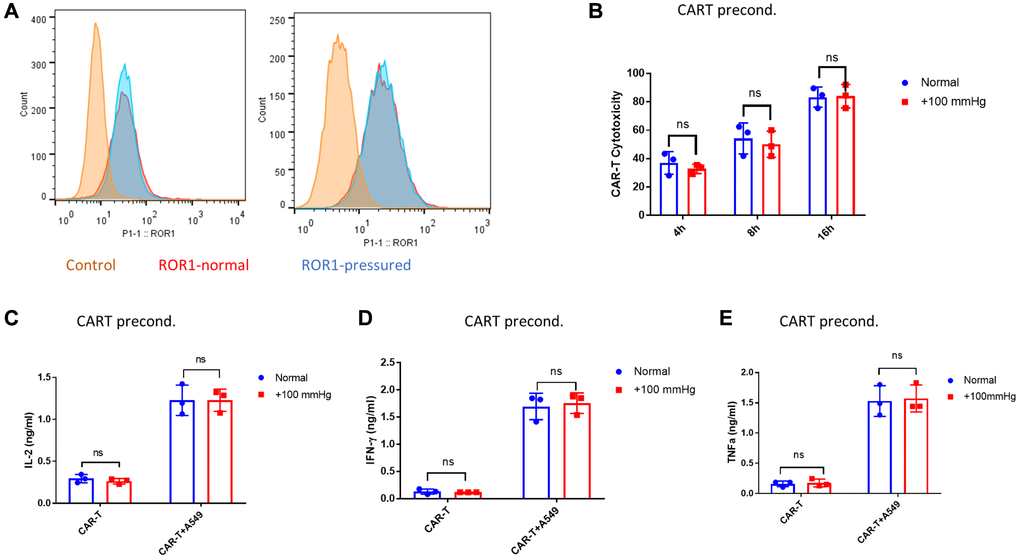
Because both CAR T cells and cancer cells were under elevated pressure in cytotoxicity assay, the reduced cytotoxicity could be attributed to either αROR1-CAR T, A549, or both. We first tested if preconditioning of αROR1-CAR T cells under elevated pressure (+100 mmHg) for 24 hours could result in reduced cytotoxicity. We verified that the αROR1-CAR expression on T cell surface was not changed by 24 hours of pressurized culture (Figure 2A). We then preconditioned αROR1-CAR T cells with +100 mmHg for 24 hours and co-cultured with A549-Red-Fluc cells under normal conditions for 16 hours. Interestingly, 24-hour pressure preconditioning did not significantly alter CAR-T cytotoxicity (Figure 2B). Cytokines in the co-culture medium were evaluated by enzyme-linked immunosorbent assay (ELISA). Consistent with cytotoxicity assay, IL-2, IFN-γ, and TNF-α were not changed by pressure preconditioning of αROR1-CAR T cells (Figure 2C–2E).
Pressure preconditioning A549 cells increased PD-L1 expression and caused resistance to αROR1-CAR T cell treatment
We next asked if A549 cells could become more resistant to CAR-T cells under elevated pressure. To mimic chronic pressure in solid tumors, we have maintained A549 cells in +100 mmHg for at least 2 passages (~7 days). We pressure-preconditioned A549 cells for 7 days but co-cultured with non-pressurized αROR1-CAR T cells for 4, 8, and 16 hours. Indeed, pressure preconditioning of A549 cells slightly increased the resistance to αROR1-CAR T cell cytotoxicity (Figure 3A). To further confirm this result, we cultured A549 cells under +100 mmHg pressure for 1, 3, 7, 14 days and examined the cytotoxicity after incubating with CAR-T cells for 16 hours. We found a time-dependent resistance of A549 cells to CAR-T cytotoxicity (Figure 3B). 14-day and 7-day preconditioning caused significant resistance to αROR1-CAR T cell; 3-day preconditioning followed the same trend (P = 0.06); 1-day preconditioning showed no discernible effect. Consistently, the cytokine release experiment by ELISA confirmed that pressure-preconditioning over 7 days suppressed the release of IL-2, IFN-γ, and TNF-α (Figure 3C–3E).
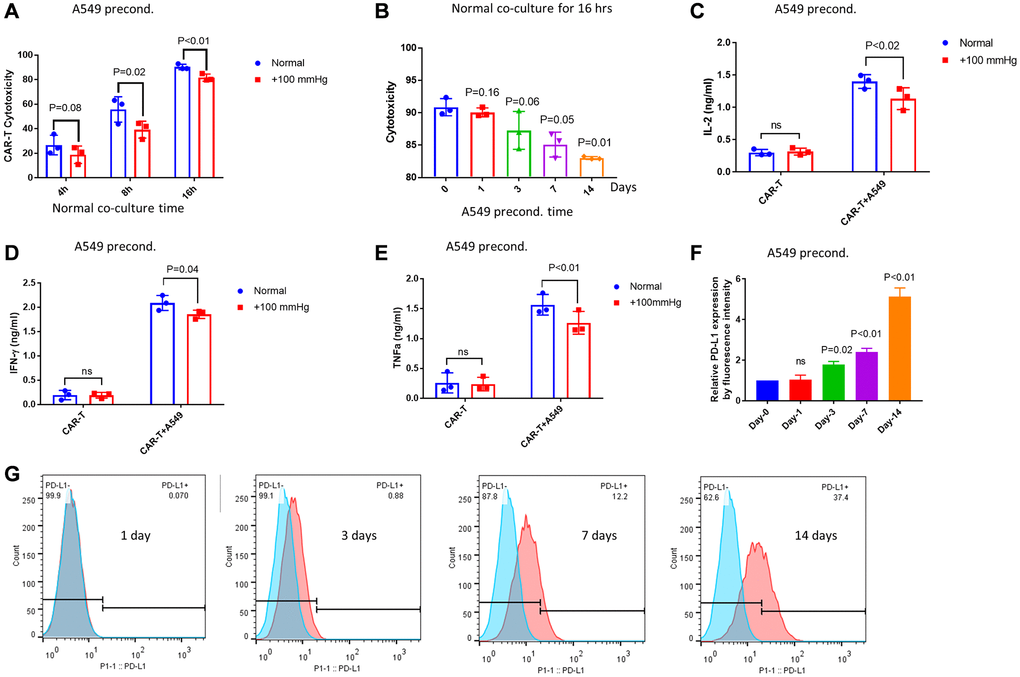
Up-regulation of immune checkpoint proteins can cause resistance to immune cell-mediated cytotoxicity in several cancer types. Among them, PD-L1 has received increasing attention in recent years [28]. We tested if PD-L1 could be upregulated under elevated pressure and cause resistance to αROR1-CAR T treatment. Again, we passaged cells under +100 mmHg for 2 weeks, 1 week, 3 days, 1 day and compared the expression of PD-L1 to cells cultured under normal pressure. As shown by our flow cytometry results (Figure 3F and 3G), the expression of PD-L1 was upregulated by elevated pressure in a time-dependent manner, correlated with the cytotoxicity shown in Figure 3A. We also measured another PD-1 ligand PD-L2 in A549 cells. Indeed, PD-L2 was also elevated in A549 cells (Supplementary Figure 1A). Interestingly, both PD-L1 and PD-L2 expression levels were increased by 100 mmHg (Supplementary Figure 1B and 1C), suggesting that pressure could have suppressing effects on other cancer cells.
PD-1 antibodies enhanced αROR1-CAR T killing of A549 lung cancer cells under elevated pressure
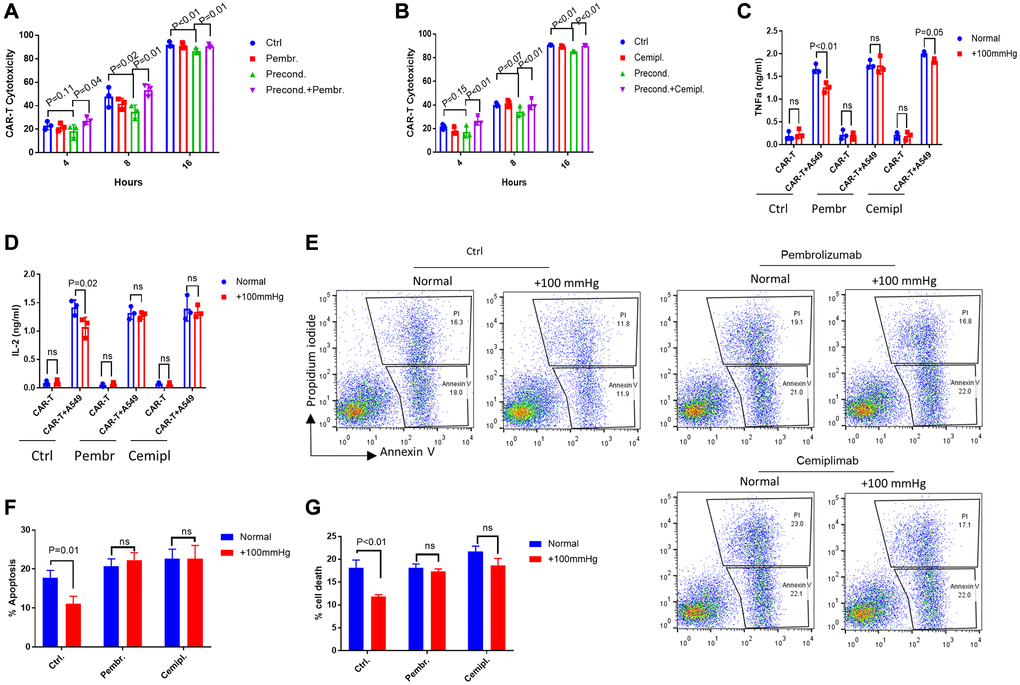
We asked if the increased expression of PD-L1/PD-L2 in A549 cells under elevated pressure could contribute to the decrease in CAR-T cell-mediated cytotoxicity. PD-L1/PD-L2 inhibits T cell cytotoxicity by interacting with PD-1 on T cell surface. The recent FDA-approved antibody drugs pembrolizumab and Cemiplimab block such interaction, increase cancer antigen recognition, therefore contribute to cancer eradication. We tested if these antibodies could also mitigate the pressure-induced resistance to CAR-T cell treatment. By adding Pembrolizumab (10 μg/ml) or Cemiplimab (10 μg/ml) directly into the co-cultured αROR1-CAR T and A549 cells, we found that the pressure-induced resistance was largely blocked (Figure 4A–4B). Consistently, the secretion of cytokines IFN-γ and TNF-α was largely rescued to the levels under normal conditions (Figure 4C–4D). In addition, the apoptotic cell death in pressure-preconditioned A549 cells was also robustly increased (Figure 4E–4G). Together, our data suggest that PD-L1 antibodies could enhance CAR-T-mediated cytotoxicity in solid tumors.
Pressure preconditioning increased tumor size in A549 xenograft mice, which was blocked by Pembrolizumab
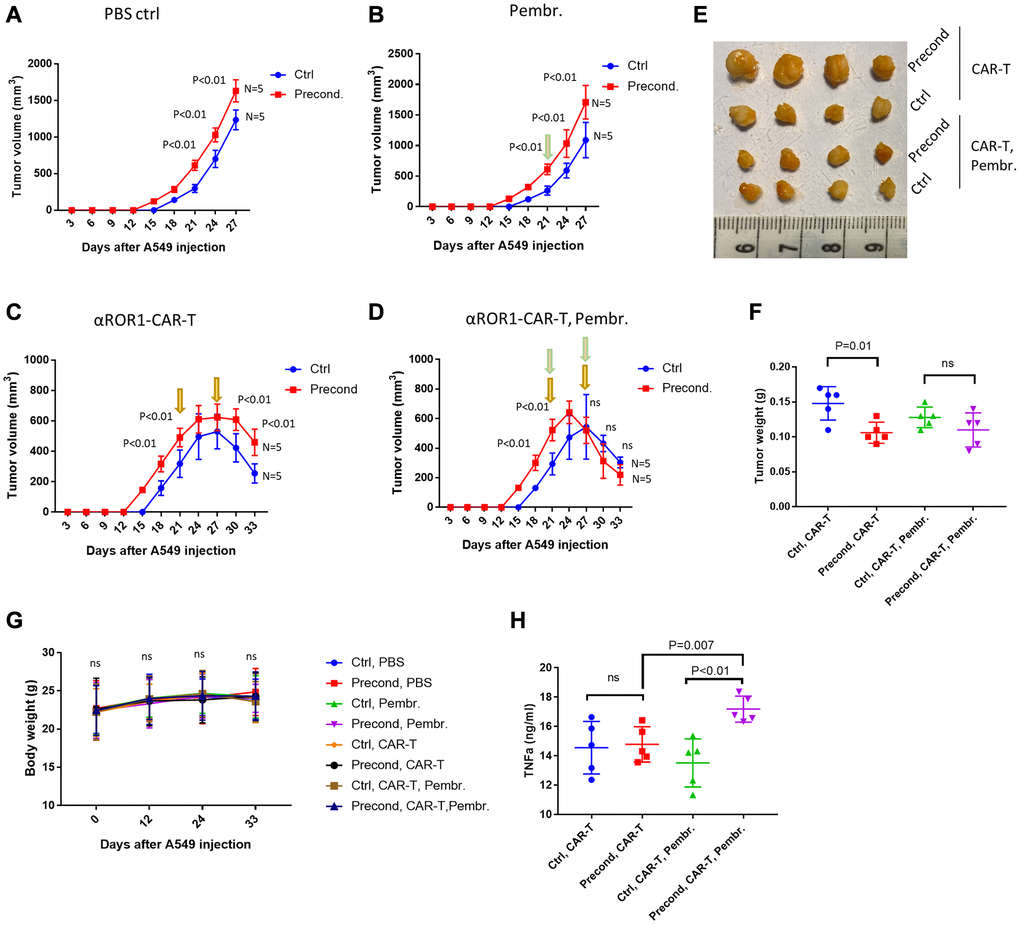
To further confirm our in vitro study, we established xenograft tumors in male BALB/c athymic nude mice by injecting A549 cells subcutaneously. We followed the growth of the tumors and found that, interestingly, pressure-preconditioned A549 cells formed tumors faster than normal A549 cells, resulting in larger tumor size at the same time following injection (Figure 5A). Larger tumor size was observed regardless of treatment with PD-L1 antibody pembrolizumab or αROR1-CAR T cells (Figure 5B–5C). However, when treated with pembrolizumab and αROR1-CAR T cells in combination, the larger size of pressure-preconditioned A549 tumors was shrinking faster, resulting in no difference after 6 days of treatment (Figure 5D–5F). All treatments, including pembrolizumab, αROR1-CAR T cells, or in combination did not change the weight of mice, nor did they change the appearance and mobility of the mice, suggesting a specific effect of the combined therapy (Figure 5G). Consistently, the plasma TNFα levels were increased specifically by combined therapy of pembrolizumab and αROR1-CAR T cells, but not by individual treatments (Figure 5H). These results confirmed our in vitro study and suggested that PD-L1 checkpoint inhibitors could enhance CAR T cells cytotoxicity in solid tumors.
Discussion
Hypoxia, nutrient starvation and tumor interstitial fluid pressure (TIFP) are the three major characteristics of solid tumors. TIFP was initially thought to dampen chemotherapy simply through blocking drug delivery [32]. However, recent studies show that TIFP can change genome-wide gene expression to remodel extracellular matrix [13, 14], suggesting that TIFP could be actively involved in cancer development. Indeed, TIFP was found to be correlated to poor prognosis, cancerous proliferation and metastasis [15–18]. In addition, lowering TIFP has shown promising results in improving cancer chemotherapy [20, 21]. However, compared to hypoxia and nutrient starvation, research on TIFP in vivo and in vitro remains scarce. In this study, by modeling TIFP in vitro, we show that elevated pressure (+100 mmHg) increased immune checkpoint PD-L1 expression, causing resistance to CAR T cell-mediated cytotoxicity. In addition, we show that the FDA-approved PD-1 blockage antibodies Pembrolizumab and Cemiplimab alleviated the pressure-induced resistance to CAR T cell therapy. In the xenograft mice, pressure preconditioning increases tumorigenesis, which was blocked by combining Pembrolizumab with CAR T cell therapy. Our study has obtained novel knowledge regarding TIFP’s role in cancer progression and could suggest better strategies to teat solid cancers.
The silence of CAR T and T cells in the tumor microenvironment is multilayers [7, 33]. Our study has examined only the pressure effect in a short period. In our system, although PD-L1 expression in A549 cells played a predominant role in CAR-T cell resistance, it is unlikely that this mechanism would be accountable for all aspects of CAR T cells inhibition in solid tumors. In addition, although αROR1-CAR T cells were not affected by 24 hours of elevated pressure in our system, most tumor infiltrating T cells reside in solid tumors for longer time and likely would be affected by TIFP. Consistently with this idea, in the xenograft mice, PD-1 inhibiting antibody readily increased cytotoxicity of CAR T cells, indicating that these CAR T cells have been hampered to some degree in the pressured tumor microenvironment.
The infiltration of immune cells into the solid tumors is limited. Decreasing TIFP is known to increase T cell infiltration and improve immunotherapy [20, 21]. However, in our case, αROR1 CAR-T is not likely functioning to decrease TIFP, because ROR1 is an immune checkpoint protein and has not been shown to decrease TIFP. In addition, our in vitro results show that αROR1 CAR-T eradiated A549 tumor cells effectively. Therefore, we believe that the infiltration of ROR1-CAR T cells into the solid tumors remains scarce. It is more likely that CAR-T cells are more active in combination with PD-1 antibodies, therefore contributing to improved cancer cell eradication. Based on above reasoning, strategies that reducing TIFP such as anti-VEGFR antibodies likely will increase αROR1-CAR T infiltration and further enhance cancer eradication.
Our study did not find any effect of TIFP on cytokine release and cytotoxicity CAR-T cells, consistent with a study in a hypertension mouse model [34]. In that study, increasing systolic pressure activated T cell; however, such pressure did not affect cytokine production in isolated human T cells and monocytes, nor did it affect the T-cell proliferation in these settings [34]. However, we cannot rule out the possibility that CAR-T cells are affected by pressure in vivo under the tumor microenvironment. The lack of activation of CAR-T cells by pressure in our study could simply be due to the ex vivo environment, where multiple cytokines required for T cell activation are missing. It would be interesting to study in vivo if CAR-T cells could be activated by elevated pressure either in mice models or human subjects.
Increasing PD-L1 and PD-L2 expression is a common strategy for cancer cells to evade immune surveillance [35]. Our findings of elevated PD-L1 and PD-L2 by pressure support several recent studies showing the matric stiffness in elevating PD-L1 expression in other cancer cells [36, 37]. There are several studies showing the TIFP to be around 5–40 mmHg [11]. However, in this range of pressure, we did not observe any change in either PD-L1 or PD-L2 expression in A549 cells (Supplementary Figure 2). Although higher than reported TIFP, we believe 100 mmHg is still valuable to be used as a model, as no in vitro model can fully reflect the complex in vivo system. In this study, we mostly use A549 cells as a model. However, since TIFP is a general feature of solid tumors, it is likely that elevated pressure would exert similar effect on CAR T cell therapy for other types of cancer. Similarly, although we use αROR1-CAR T cells in this study, it is likely that CAR-T cells targeting other cancer antigens will be inhibited by TIFP in vivo.
Methods
Cell culture
Human NSCLC cell line A549 stably expressing red firefly luciferase (A549-Red-Fluc) was purchased from PerkinElmer. A549 and HEK-293T cells are originally obtained from American Type Culture Collection. A549 and HEK-293T cells were maintained in Dulbecco's modified Eagle's medium (DMEM) supplemented with10% FBS. Fully anonymized human PBMCs were collected and frozen in Affiliated Hospital of Guilin Medical University during 12/2015–1/2017 with written consent from donors and approval from the Ethics Committee of the Hospital. PBMCs were accessed during 7/2018–3/2020 for this study. PBMCs were thawed and cultured in AIM-V™ Medium (Gibco) containing10% FBS and expanded by adding αCD3/αCD28 beads in a cell-to-bead ratio of 1:1 and IL-2 at 200 IU/ml. All cells were cultured in a humidified incubator with 5% CO2 at 37°C. The pressure was applied using the Continuous Flow Constant Pressure cell culture (CFCPcc) device purchased from BioExcellence International Tech (Beijing, China). The device consists of an adjustable pressured pump connected to a sealed chamber in a normal CO2 incubator (Supplementary Figure 3). The pressure was controlled at 100 mmHg automatically by a sensor inserted in the cell culture chamber. The pump compresses the air in the incubator (74% N2, 21% O2, and 5% CO2) to the chamber continuously.
CAR T cell generation
The αROR1-CAR was generated using the DNA fragment of scFv derived from a rabbit anti-human ROR1 mAb clone R12 published before [29], cloned into CAR lentivirus backbone encoding a CD3ζ signaling domain and a 4-1BB co-stimulatory domain. The resulting αROR1-CAR-encoding lentivirus was produced via transient transduction of HEK-293T cells using Gibco LV-MAX Lentiviral Production system according to the manufacturer’s manual. Frozen human PBMCs from healthy donors were thawed in AIM-V™ Medium (Gibco) supplemented with 10% FBS, then activated by adding αCD3/αCD28 beads in a cell-to-bead ratio of 1:1 and IL-2 at 200 IU/ml. After 24 h, αROR1-CAR lentivirus was added to PBMCs. AIM-V™ Medium containing IL-2 was added every 2–3 days to dilute the growing T cells. After expansion for 2 weeks, expression of αROR1-CAR was confirmed by flow cytometry and cytotoxicity assay was carried out with fresh αROR1-CAR T cells.
CAR T cell-mediated cytotoxicity assay
Cellular luciferase-based cytotoxicity was performed as in [38]. A549-Red-Fluc cells stably expressing red firefly luciferase were plated at the density of 20,000/well in a 96-well plate for 16 hours. αROR1-CAR T cells at effector-to-target (E:T) ratios of 10:1 were added to A549-Red-Fluc cells. After 4, 8 and 16 hours, A549-Red-Fluc cells on the plates were washed with PBS and 1X cell lysis buffer was added directly to lyse cell by shaking at room temperature for 5 min. For each well, 50 ul cell lysate was transferred to white opaque plates and 50 ul luciferin working solution (Firefly Luc One-Step Glow Assay Kit, Pierce) was added. After incubation at room temperature for 10 min, luminescence was detected by SpectraMax Microplate Reader using a default protocol. CAR-T cytotoxicity was calculated by measuring the percentage of decrease in luminescence: 100*(1–(Luminescence of CAR-T-treated wells)/(Luminescence of non-treated cells)).
Cytokine release assay
After incubation of αROR1-CAR T cells with A549 cells for 16 hours, cells on 96-well plates were centrifuged and supernatants were transferred to new plates. Cytokines released by CAR T cells were measured by using Human DuoSet ELISA kits according to the manufacturer’s protocol (R&D Systems). Cytokine concentrations were calculated by generating standard curves along with the experiments.
Flow cytometry
CAR T cells were removed by washing the plates with cold PBS. A549 cells were trypsinized to detach from plates and washed with cold PBS pH7.4 containing 0.5% albumin, then incubated with primary antibodies or IgG isotype controls at suggested dilutions for 1 hour. Cells were then washed extensively with (PBS, 0.5% albumin) and incubated with fluorochrome-conjugated secondary antibodies at suggested dilutions. For apoptosis, FTIC-Annexin V and Propidium iodide were added according to the manufacturer’s manual. Mouse monoclonal anti-human PD-L1 and PD-L2 antibodies (R&D Systems) were added to the cells at 200× dilution and PE-conjugated goat anti-mouse secondary antibody (BioLegend) was added at 500X dilution. For αROR1-CAR expression, ROR1 recombinant proteins were biotinylated and incubated with αROR1-CAR T cells for 1 hour. After washing, PE-conjugated streptavidin was then added. Flow cytometry analysis was performed on cytoFLEX S (BECKMAN). The remaining CAR-T cells were further removed by size gating (Supplementary Figure 4). Data were analyzed and plotted by using the FlowJo (V10.7) software.
Tumor xenograft model
Six-week-old male BALB/c athymic nude mice were obtained from Shanghai Jiao Tong University School of Medicine. Animal experiments were approved by Animal Care and Use Committee. Control or pressure-conditioned (+100 mmHg for 14 days) A549 cells (1 × 107 in 0.1 ml PBS) were injected subcutaneously into the right-lower flank of the nude mice (20 controls and 20 pressure-conditioned). Each group was further divided into 4 subgroups (5 animals/group) for 4 treatments: PBS, αROR1-CAR T cells, Pembrolizumab, and αROR1-CAR T cells plus Pembrolizumab. The tumors were measured every 3 days using a Vernier caliper and tumor volume calculated as follows: tumor volume (mm3) = (shorter diameter2 × longer diameter)/2. CAR-T cells (1 × 107 cells/mice) or/and Pembrolizumab (5 mg/kg) were injected intravenously 21 and 27 days after injection of A549 cells. At the end of the experiment, mice were sacrificed and tumors were surgically removed and imaged. In addition, plasma was collected from the blood for ELISA on human IFN-γ.
Statistical analysis
Data were plotted and analyzed by using GraphPad Prism 7 software. All experiments contain at least 3 biological repeats. The difference between the mean values was analyzed by paired student’s t-test if not otherwise indicated. P values less than 0.05 were considered statistically significant in this study.
Supplementary Materials
Author Contributions
J.L., Y.L., and Y.W. conceived and designed the experiments. J.L., Y.L., and X.F. performed the experiments and collected the data. J.L., Y.L., and Y.W. analyzed the data, prepared the figures and wrote the paper. All authors revised the manuscript.
Conflicts of Interest
The authors declare no conflicts of interest related to this study.
Funding
This work was supported by The Natural Science Foundation of Guangxi (2017GxNSFDA198022) and The National Natural Science Foundation of China (81460411 and 81660450).
References
- 1. Feins S, Kong W, Williams EF, Milone MC, Fraietta JA. An introduction to chimeric antigen receptor (CAR) T-cell immunotherapy for human cancer. Am J Hematol. 2019; 94:S3–9. https://doi.org/10.1002/ajh.25418 [PubMed]
- 2. Hong M, Clubb JD, Chen YY. Engineering CAR-T Cells for Next-Generation Cancer Therapy. Cancer Cell. 2020; 38:473–88. https://doi.org/10.1016/j.ccell.2020.07.005 [PubMed]
- 3. Aleksic M, Liddy N, Molloy PE, Pumphrey N, Vuidepot A, Chang KM, Jakobsen BK. Different affinity windows for virus and cancer-specific T-cell receptors: implications for therapeutic strategies. Eur J Immunol. 2012; 42:3174–79. https://doi.org/10.1002/eji.201242606 [PubMed]
- 4. Zhang C, Liu J, Zhong JF, Zhang X. Engineering CAR-T cells. Biomark Res. 2017; 5:22. https://doi.org/10.1186/s40364-017-0102-y [PubMed]
- 5. Halim L, Maher J. CAR T-cell immunotherapy of B-cell malignancy: the story so far. Ther Adv Vaccines Immunother. 2020; 8:2515135520927164. https://doi.org/10.1177/2515135520927164 [PubMed]
- 6. Petrova V, Annicchiarico-Petruzzelli M, Melino G, Amelio I. The hypoxic tumour microenvironment. Oncogenesis. 2018; 7:10. https://doi.org/10.1038/s41389-017-0011-9 [PubMed]
- 7. Lim AR, Rathmell WK, Rathmell JC. The tumor microenvironment as a metabolic barrier to effector T cells and immunotherapy. Elife. 2020; 9:e55185. https://doi.org/10.7554/eLife.55185 [PubMed]
- 8. Böckelmann LC, Schumacher U. Targeting tumor interstitial fluid pressure: will it yield novel successful therapies for solid tumors? Expert Opin Ther Targets. 2019; 23:1005–14. https://doi.org/10.1080/14728222.2019.1702974 [PubMed]
- 9. Lee I, Boucher Y, Demhartner TJ, Jain RK. Changes in tumour blood flow, oxygenation and interstitial fluid pressure induced by pentoxifylline. Br J Cancer. 1994; 69:492–96. https://doi.org/10.1038/bjc.1994.89 [PubMed]
- 10. Kim HG, Yu AR, Lee JJ, Lee YJ, Lim SM, Kim JS. Measurement of Tumor Pressure and Strategies of Imaging Tumor Pressure for Radioimmunotherapy. Nucl Med Mol Imaging. 2019; 53:235–41. https://doi.org/10.1007/s13139-019-00598-7 [PubMed]
- 11. Yu T, Liu K, Wu Y, Fan J, Chen J, Li C, Zhu G, Wang Z, Li L. High interstitial fluid pressure promotes tumor cell proliferation and invasion in oral squamous cell carcinoma. Int J Mol Med. 2013; 32:1093–100. https://doi.org/10.3892/ijmm.2013.1496 [PubMed]
- 12. Heldin CH, Rubin K, Pietras K, Ostman A. High interstitial fluid pressure - an obstacle in cancer therapy. Nat Rev Cancer. 2004; 4:806–13. https://doi.org/10.1038/nrc1456 [PubMed]
- 13. Yang P, Agapova O, Parker A, Shannon W, Pecen P, Duncan J, Salvador-Silva M, Hernandez MR. DNA microarray analysis of gene expression in human optic nerve head astrocytes in response to hydrostatic pressure. Physiol Genomics. 2004; 17:157–69. https://doi.org/10.1152/physiolgenomics.00182.2003 [PubMed]
- 14. Karjalainen HM, Sironen RK, Elo MA, Kaarniranta K, Takigawa M, Helminen HJ, Lammi MJ. Gene expression profiles in chondrosarcoma cells subjected to cyclic stretching and hydrostatic pressure. A cDNA array study. Biorheology. 2003; 40:93–100. [PubMed]
- 15. Hompland T, Ellingsen C, Øvrebø KM, Rofstad EK. Interstitial fluid pressure and associated lymph node metastasis revealed in tumors by dynamic contrast-enhanced MRI. Cancer Res. 2012; 72:4899–908. https://doi.org/10.1158/0008-5472.CAN-12-0903 [PubMed]
- 16. Yeo SG, Kim JS, Cho MJ, Kim KH, Kim JS. Interstitial fluid pressure as a prognostic factor in cervical cancer following radiation therapy. Clin Cancer Res. 2009; 15:6201–07. https://doi.org/10.1158/1078-0432.CCR-09-0560 [PubMed]
- 17. Rofstad EK, Ruud EB, Mathiesen B, Galappathi K. Associations between radiocurability and interstitial fluid pressure in human tumor xenografts without hypoxic tissue. Clin Cancer Res. 2010; 16:936–45. https://doi.org/10.1158/1078-0432.CCR-09-2718 [PubMed]
- 18. Lunt SJ, Kalliomaki TM, Brown A, Yang VX, Milosevic M, Hill RP. Interstitial fluid pressure, vascularity and metastasis in ectopic, orthotopic and spontaneous tumours. BMC Cancer. 2008; 8:2. https://doi.org/10.1186/1471-2407-8-2 [PubMed]
- 19. Hansem LMK, Huang R, Wegner CS, Simonsen TG, Gaustad JV, Hauge A, Rofstad EK. Intratumor Heterogeneity in Interstitial Fluid Pressure in Cervical and Pancreatic Carcinoma Xenografts. Transl Oncol. 2019; 12:1079–85. https://doi.org/10.1016/j.tranon.2019.05.012 [PubMed]
- 20. Hofmann M, Guschel M, Bernd A, Bereiter-Hahn J, Kaufmann R, Tandi C, Wiig H, Kippenberger S. Lowering of tumor interstitial fluid pressure reduces tumor cell proliferation in a xenograft tumor model. Neoplasia. 2006; 8:89–95. https://doi.org/10.1593/neo.05469 [PubMed]
- 21. Salnikov AV, Iversen VV, Koisti M, Sundberg C, Johansson L, Stuhr LB, Sjöquist M, Ahlström H, Reed RK, Rubin K. Lowering of tumor interstitial fluid pressure specifically augments efficacy of chemotherapy. FASEB J. 2003; 17:1756–58. https://doi.org/10.1096/fj.02-1201fje [PubMed]
- 22. Chen L, Han X. Anti-PD-1/PD-L1 therapy of human cancer: past, present, and future. J Clin Invest. 2015; 125:3384–91. https://doi.org/10.1172/JCI80011 [PubMed]
- 23. Alsaab HO, Sau S, Alzhrani R, Tatiparti K, Bhise K, Kashaw SK, Iyer AK. PD-1 and PD-L1 Checkpoint Signaling Inhibition for Cancer Immunotherapy: Mechanism, Combinations, and Clinical Outcome. Front Pharmacol. 2017; 8:561. https://doi.org/10.3389/fphar.2017.00561 [PubMed]
- 24. Na Z, Yeo SP, Bharath SR, Bowler MW, Balıkçı E, Wang CI, Song H. Structural basis for blocking PD-1-mediated immune suppression by therapeutic antibody pembrolizumab. Cell Res. 2017; 27:147–50. https://doi.org/10.1038/cr.2016.77 [PubMed]
- 25. Lei C, Peng X, Gong X, Fan Y, Wu S, Liu N, Li L, Huang J, Zheng G, Long Z. Prognostic role of programmed death-ligand 1 expression in patients with biliary tract cancer: a meta-analysis. Aging (Albany NY). 2019; 11:12568–80. https://doi.org/10.18632/aging.102588 [PubMed]
- 26. Wang A, Wang HY, Liu Y, Zhao MC, Zhang HJ, Lu ZY, Fang YC, Chen XF, Liu GT. The prognostic value of PD-L1 expression for non-small cell lung cancer patients: a meta-analysis. Eur J Surg Oncol. 2015; 41:450–56. https://doi.org/10.1016/j.ejso.2015.01.020 [PubMed]
- 27. Jenkins RW, Barbie DA, Flaherty KT. Mechanisms of resistance to immune checkpoint inhibitors. Br J Cancer. 2018; 118:9–16. https://doi.org/10.1038/bjc.2017.434 [PubMed]
- 28. Jiang X, Wang J, Deng X, Xiong F, Ge J, Xiang B, Wu X, Ma J, Zhou M, Li X, Li Y, Li G, Xiong W, et al. Role of the tumor microenvironment in PD-L1/PD-1-mediated tumor immune escape. Mol Cancer. 2019; 18:10. https://doi.org/10.1186/s12943-018-0928-4 [PubMed]
- 29. Hudecek M, Lupo-Stanghellini MT, Kosasih PL, Sommermeyer D, Jensen MC, Rader C, Riddell SR. Receptor affinity and extracellular domain modifications affect tumor recognition by ROR1-specific chimeric antigen receptor T cells. Clin Cancer Res. 2013; 19:3153–64. https://doi.org/10.1158/1078-0432.CCR-13-0330 [PubMed]
- 30. Balakrishnan A, Goodpaster T, Randolph-Habecker J, Hoffstrom BG, Jalikis FG, Koch LK, Berger C, Kosasih PL, Rajan A, Sommermeyer D, Porter PL, Riddell SR. Analysis of ROR1 Protein Expression in Human Cancer and Normal Tissues. Clin Cancer Res. 2017; 23:3061–71. https://doi.org/10.1158/1078-0432.CCR-16-2083 [PubMed]
- 31. Zhang S, Chen L, Wang-Rodriguez J, Zhang L, Cui B, Frankel W, Wu R, Kipps TJ. The onco-embryonic antigen ROR1 is expressed by a variety of human cancers. Am J Pathol. 2012; 181:1903–10. https://doi.org/10.1016/j.ajpath.2012.08.024 [PubMed]
- 32. Lunt SJ, Fyles A, Hill RP, Milosevic M. Interstitial fluid pressure in tumors: therapeutic barrier and biomarker of angiogenesis. Future Oncol. 2008; 4:793–802. https://doi.org/10.2217/14796694.4.6.793 [PubMed]
- 33. Scarfò I, Maus MV. Current approaches to increase CAR T cell potency in solid tumors: targeting the tumor microenvironment. J Immunother Cancer. 2017; 5:28. https://doi.org/10.1186/s40425-017-0230-9 [PubMed]
- 34. Itani HA, McMaster WG
Jr , Saleh MA, Nazarewicz RR, Mikolajczyk TP, Kaszuba AM, Konior A, Prejbisz A, Januszewicz A, Norlander AE, Chen W, Bonami RH, Marshall AF, et al. Activation of Human T Cells in Hypertension: Studies of Humanized Mice and Hypertensive Humans. Hypertension. 2016; 68:123–32. https://doi.org/10.1161/HYPERTENSIONAHA.116.07237 [PubMed] - 35. Sun C, Mezzadra R, Schumacher TN. Regulation and Function of the PD-L1 Checkpoint. Immunity. 2018; 48:434–52. https://doi.org/10.1016/j.immuni.2018.03.014 [PubMed]
- 36. Miyazawa A, Ito S, Asano S, Tanaka I, Sato M, Kondo M, Hasegawa Y. Regulation of PD-L1 expression by matrix stiffness in lung cancer cells. Biochem Biophys Res Commun. 2018; 495:2344–49. https://doi.org/10.1016/j.bbrc.2017.12.115 [PubMed]
- 37. Azadi S, Aboulkheyr Es H, Razavi Bazaz S, Thiery JP, Asadnia M, Ebrahimi Warkiani M. Upregulation of PD-L1 expression in breast cancer cells through the formation of 3D multicellular cancer aggregates under different chemical and mechanical conditions. Biochim Biophys Acta Mol Cell Res. 2019; 1866:118526. https://doi.org/10.1016/j.bbamcr.2019.118526 [PubMed]
- 38. Fu X, Tao L, Rivera A, Williamson S, Song XT, Ahmed N, Zhang X. A simple and sensitive method for measuring tumor-specific T cell cytotoxicity. PLoS One. 2010; 5:e11867. https://doi.org/10.1371/journal.pone.0011867 [PubMed]


